## Distinguishing RRD from TRD ### Key Pathophysiologic Difference **Key Point:** The defining feature of rhegmatogenous retinal detachment is the presence of a full-thickness retinal break (hole or tear) through which vitreous fluid seeps into the subretinal space, separating the neurosensory retina from the retinal pigment epithelium. Tractional detachment, by contrast, occurs without any break — the retina is mechanically pulled off by scar tissue contraction. ### Comparative Table | Feature | Rhegmatogenous RD | Tractional RD | |---------|-------------------|---------------| | **Retinal break** | **Present (diagnostic)** | Absent | | Primary mechanism | Vitreous fluid ingress through break | Scar tissue traction | | Common causes | Myopia, lattice degeneration, PVD | Proliferative diabetic retinopathy, ROP, trauma | | Onset | Often acute | Insidious, gradual | | Macula involvement | Variable | Often spared initially | | Progression | Rapid (days–weeks) | Slow (weeks–months) | | PVR association | Common | Less common | ### High-Yield Distinction **High-Yield:** On indirect ophthalmoscopy or OCT, the presence of a retinal hole or tear is the single most discriminating feature. RRD will show a break; TRD will not. This is the gold standard for differentiation and drives management (RRD requires break closure; TRD requires release of traction). ### Clinical Pearl **Clinical Pearl:** In diabetic patients with retinal detachment, always look for the break in RRD — if none is found despite careful examination, suspect TRD from proliferative diabetic retinopathy, which may require vitrectomy and membrane peeling rather than pneumatic retinopexy or scleral buckle. ### Why Other Features Are Not Discriminating - **Macula involvement:** Both RRD and TRD can involve the macula; this is not specific to either. - **Rapid progression:** While RRD tends to progress faster, TRD can also progress rapidly in aggressive cases (e.g., ROP). - **PVR association:** Although PVR is more common in RRD, it can occur in TRD as well, especially after trauma or advanced diabetic disease. 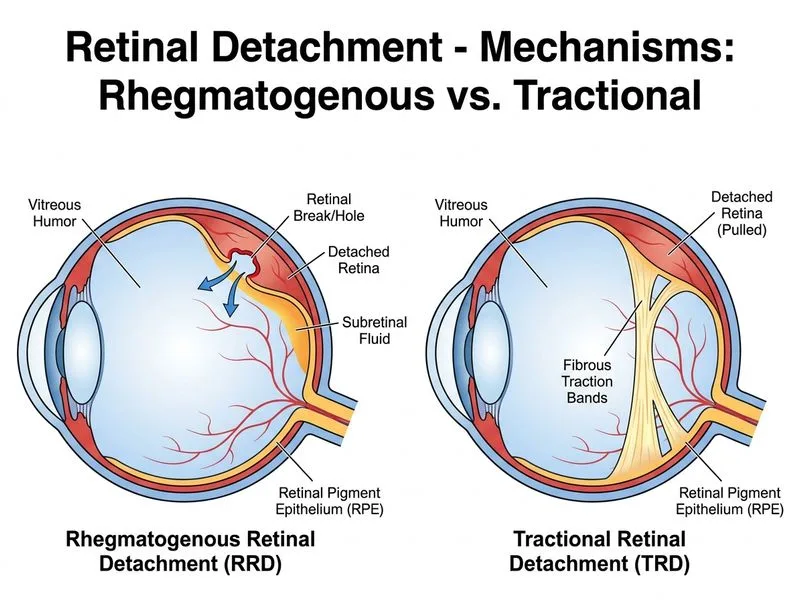
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.