## Clinical Scenario: Retinal Hole Without Detachment The patient has: - **Retinal hole** (confirmed on dilated fundus examination) - **No retinal detachment** (yet) - **Risk factors:** High myopia, positive family history - **Asymptomatic** status The question asks for the **best investigation to assess risk of progression** and guide management decisions. ## Investigation of Choice **Key Point:** Optical coherence tomography (OCT) of the posterior pole is the most appropriate investigation to assess the structural integrity of the vitreoretinal interface and risk of progression to detachment. ### Why OCT Is Superior for Risk Stratification 1. **Vitreoretinal interface assessment** — Detects posterior vitreous detachment (PVD) status - Presence of PVD = lower risk of progression - Absence of PVD = higher risk of progression 2. **Macular involvement** — Determines if the hole is in or near the macula - Macular holes require urgent surgery - Peripheral holes can be observed if PVD is present 3. **Epiretinal membrane (ERM) detection** — Identifies tractional forces that may promote detachment 4. **Quantifies subretinal fluid** — Even minimal fluid changes are visible on OCT 5. **Non-invasive, high-resolution imaging** — Provides cross-sectional anatomy without dye injection 6. **Guides management** — Determines whether observation, laser, or vitrectomy is indicated ## Management Algorithm Based on OCT Findings ```mermaid flowchart TD A[Retinal hole without detachment]:::outcome --> B{PVD present on OCT?}:::decision B -->|Yes| C[Low risk of progression]:::outcome C --> D[Observation with regular follow-up]:::action B -->|No| E[Higher risk of progression]:::outcome E --> F{Hole location?}:::decision F -->|Macula| G[Urgent vitrectomy]:::urgent F -->|Peripheral| H[Laser or vitrectomy]:::action A --> I{Subretinal fluid on OCT?}:::decision I -->|Present| J[Indicates early detachment]:::urgent I -->|Absent| K[Stable for now]:::outcome ``` **High-Yield:** OCT is the **single best investigation** for risk stratification in retinal holes because it reveals the vitreoretinal interface status — the key determinant of progression risk. ## Comparison of Investigations | Investigation | Role in Retinal Hole | Utility for Risk Assessment | | --- | --- | --- | | **OCT** | Visualizes hole, PVD, subretinal fluid | **Gold standard** — guides management | | **B-scan** | Used only if media opaque | Not applicable — media is clear | | **FFA** | Assesses retinal circulation, leakage | Not useful for structural hole assessment | | **OCTA** | Evaluates retinal/choroidal vasculature | Not relevant to mechanical hole progression | **Clinical Pearl:** The presence or absence of **posterior vitreous detachment (PVD)** on OCT is the single most important factor determining whether a retinal hole will progress to detachment. If PVD is complete, the hole is unlikely to progress; if PVD is absent or partial, the risk is significantly higher. 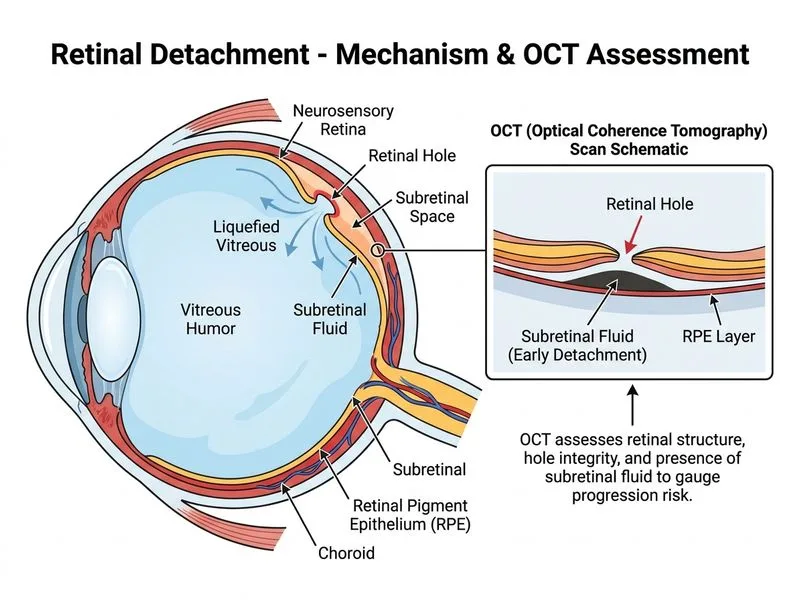
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.