## Clinical Diagnosis: Retinoblastoma ### Key Clinical Features **Key Point:** Leukocoria (white pupillary reflex or cat's eye reflex) is the most common presenting sign of retinoblastoma, occurring in 60% of cases. The combination of leukocoria, elevated intraocular pressure, and a retinal mass with calcification on imaging is pathognomonic. ### Diagnostic Criteria Met | Feature | Finding | Significance | |---------|---------|---------------| | **Age** | 2 years | Peak incidence 18–24 months; 90% diagnosed before age 5 | | **Presentation** | Leukocoria | Most common presenting sign (60%) | | **Unilateral involvement** | Left eye only | Unilateral in 60% of cases | | **IOP elevation** | 28 mmHg | Suggests mass effect or neovascular glaucoma | | **Fundoscopic finding** | White retinal mass with calcification | Pathognomonic for retinoblastoma | | **Ultrasound** | High internal reflectivity | Indicates calcification, typical of retinoblastoma | ### Classification & Staging **High-Yield:** Retinoblastoma is classified by the **International Classification for Intraocular Retinoblastoma (ICRB):** - **Group A:** Small tumours, good prognosis - **Group B:** Medium tumours, intermediate prognosis - **Group C:** Large tumours or vitreous seeding - **Group D:** Very large tumours or extensive vitreous seeding - **Group E:** Eyes with no light perception or phthisical changes (enucleation indicated) ### Differential Diagnosis Exclusion | Condition | Why Excluded | |-----------|---------------| | **Persistent fetal vasculature (PFV)** | Presents at birth; white reflex is less prominent; no calcification on imaging; no elevated IOP typically | | **Toxoplasmosis** | Causes focal retinochoroiditis with white granular lesions; no calcification; no leukocoria; usually in older children | | **Retinopathy of prematurity (ROP)** | History of prematurity required; bilateral involvement typical; no calcification; different fundoscopic appearance (neovascularization, tractional detachment) | ### Pathophysiology **Key Point:** Retinoblastoma arises from malignant transformation of immature retinal cells (retinoblasts). It is caused by biallelic inactivation of the **RB1 gene** (chromosome 13q14). Approximately 40% are hereditary (germline RB1 mutation) and 60% are sporadic (somatic mutation). ### Management Overview ```mermaid flowchart TD A[Suspected Retinoblastoma]:::outcome --> B[Confirm diagnosis: Imaging + Genetics]:::action B --> C{Unilateral or Bilateral?}:::decision C -->|Unilateral| D{ICRB Group?}:::decision C -->|Bilateral| E[Systemic chemotherapy + focal therapy]:::action D -->|A-B| F[Focal therapy: laser, cryotherapy, brachytherapy]:::action D -->|C-D| G[Systemic chemotherapy + focal therapy]:::action D -->|E| H[Enucleation]:::urgent F --> I[Surveillance every 4-6 weeks]:::action G --> I H --> J[Histopathology + adjuvant therapy if high-risk]:::action ``` ### Clinical Pearl **Clinical Pearl:** The **"cat's eye reflex"** or **leukocoria** is best detected by asking the parent about photographs taken with flash — the affected eye will show a white reflex instead of the normal red reflex. This simple screening question can lead to early diagnosis and eye salvage. ### Prognosis **High-Yield:** With modern multimodal therapy, the cure rate in developed countries exceeds 95%. However, in resource-limited settings (India), late presentation and enucleation rates remain high. Bilateral disease has a worse prognosis but is salvageable with aggressive chemotherapy and focal therapy. ### Follow-up & Surveillance - Regular ophthalmologic examination every 4–6 weeks during active treatment - Imaging (MRI/CT) to assess response - Genetic counselling for families with hereditary disease - Screening of contralateral eye and siblings in bilateral/hereditary cases 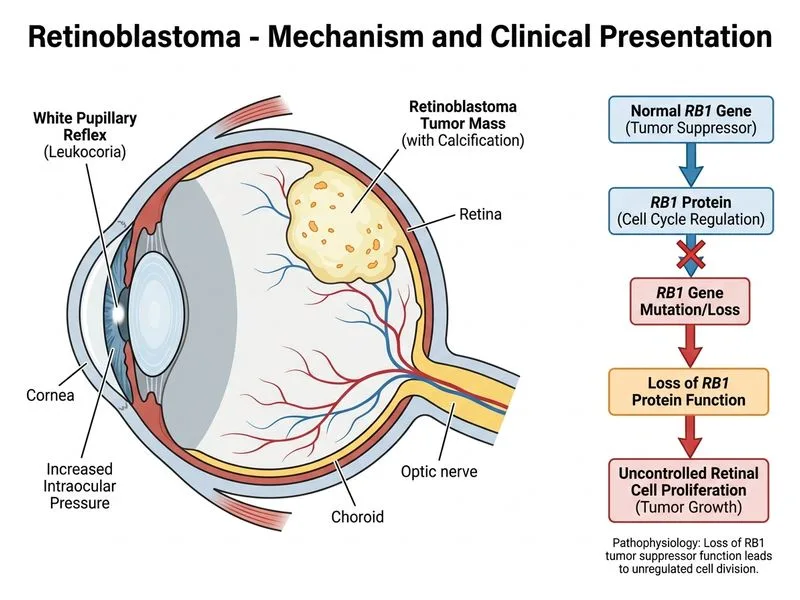
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.