## Retinoblastoma vs Retinopathy of Prematurity (ROP) ### Clinical Discriminators **Key Point:** The single best discriminator is **history of prematurity + ROP risk factors** (low birth weight, prolonged oxygen therapy) VERSUS **no prematurity history + discrete intraocular mass on imaging**. ### Comparison Table | Feature | Retinoblastoma | ROP | | --- | --- | --- | | **Risk factor** | Germline/somatic RB1 mutation | Prematurity (BW <2000 g, GA <32 weeks) | | **Leukocoria** | Yes (60% of cases) | Yes (if advanced stage) | | **Presentation** | Unilateral or bilateral; discrete mass | Usually bilateral; vascular abnormalities | | **Imaging (B-scan/MRI)** | Well-defined intraocular mass; calcification common | Retinal folds, tractional detachment; no mass | | **Age at presentation** | <5 years (peak 18–24 months) | Premature infants; detected on screening | | **Prematurity history** | None | Essential (by definition) | | **Retinal location** | Any location (central or peripheral) | Peripheral retina (zone I, II, III) | | **Vitreous involvement** | Vitreous seeding; hemorrhage | Vitreous haze, no discrete mass | ### Clinical Pearl **ROP screening protocol:** All premature infants (GA ≤32 weeks OR BW ≤1500 g) require retinal screening starting at 4–6 weeks postnatal age (or 31 weeks postmenstrual age). This child has **no prematurity history**, which immediately shifts the differential away from ROP. **Retinoblastoma red flags in this case:** - Non-premature child - Unilateral leukocoria - Discrete mass on imaging - No history of oxygen therapy or NICU admission ### High-Yield Mnemonic **ROP = Premature + Oxygen + Peripheral retina** **RB = No prematurity + Discrete mass + Any retinal location** [cite:American Academy of Pediatrics Screening Guidelines for ROP; Boyd & Melia, Pediatric Ophthalmology] 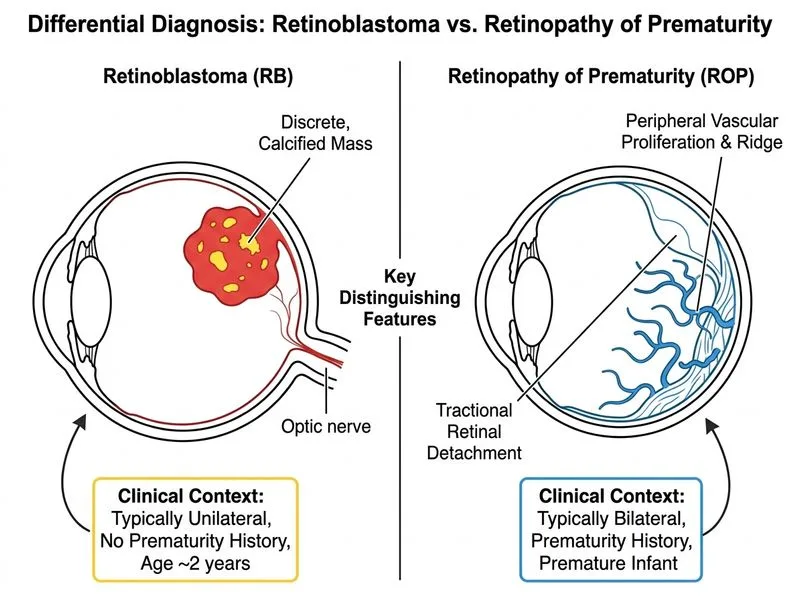
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.