## Thromboembolism Prevention in Rheumatic Mitral Stenosis with LA Thrombus ### Clinical Context: Why Anticoagulation Is Urgent **Key Point:** A patient with rheumatic mitral stenosis (MS), atrial fibrillation (indicated by irregular pulse), LA enlargement (5.5 cm), spontaneous echo contrast ("smoke"), and **documented LAA thrombus** is at extreme risk of systemic thromboembolism (stroke, peripheral arterial occlusion). Anticoagulation is the single most important intervention to prevent catastrophic stroke. ### Pathophysiology of Thromboembolism in RHD 1. **Mitral stenosis** → increased LA pressure → LA dilatation 2. **LA enlargement** → atrial fibrillation (AF) develops 3. **AF + dilated LA** → blood stasis in LAA 4. **Stasis + endothelial injury** → spontaneous echo contrast ("smoke") and thrombus formation 5. **LAA thrombus** → systemic embolism (stroke in 60–90% of untreated cases) **Clinical Pearl:** Spontaneous echo contrast ("smoke") is a marker of severe blood stasis and high thrombotic risk — it precedes visible thrombus formation. ### Anticoagulation Strategy for LAA Thrombus | Agent | Target INR / Dosing | Indication | |-------|-------------------|------------| | **Warfarin** | INR 2–3 | Gold standard for RHD + AF + thrombus | | **DOACs** (apixaban, dabigatran, edoxaban) | Fixed dose | Acceptable alternative; less data in RHD | | **Aspirin alone** | 75–325 mg daily | **Inadequate** for documented thrombus; only for AF without structural heart disease | | **Heparin bridge** | aPTT 1.5–2.5× control | Acute phase; transition to warfarin | **High-Yield:** In RHD with AF and documented LAA thrombus, **warfarin (INR 2–3) is preferred** over DOACs because: - RHD is a specific indication where warfarin has the strongest evidence - DOACs have limited data in moderate-to-severe MS - LAA thrombus requires aggressive anticoagulation ### Why Other Options Are Incorrect or Delayed **Key Point:** While mitral valve intervention (PMBC or MVR) and diuretics are important for symptom management and hemodynamic stabilization, they do **not** address the immediate life-threatening risk of thromboembolism. 1. **Mitral valve replacement (emergency):** Not indicated acutely. Valve intervention is planned electively after thrombus resolution and anticoagulation is therapeutic. 2. **Diuretics + urgent PMBC:** Appropriate for hemodynamic decompensation and dyspnea, but **secondary** to anticoagulation. PMBC cannot be performed safely with an unresolved LAA thrombus (risk of embolization during manipulation). 3. **Aspirin alone:** Inadequate for documented thrombus; increases stroke risk by 50–70% compared to warfarin. ### Management Timeline ```mermaid flowchart TD A[RHD + AF + LA enlargement + LAA thrombus]:::outcome A --> B[Initiate anticoagulation immediately]:::action B --> C[Warfarin INR 2-3 or DOAC]:::action C --> D[Repeat echo in 3-4 weeks]:::action D --> E{Thrombus resolved?}:::decision E -->|Yes| F[Plan PMBC or MVR]:::action E -->|No| G[Continue anticoagulation, reassess]:::action A --> H[Diuretics for pulmonary edema]:::action H --> I[Symptom relief, not primary therapy]:::action ``` ### Anticoagulation in RHD: Indications **Mnemonic: RHD AF CLOT** - **R**heumatic heart disease (any valve lesion) - **H**istory of thromboembolism - **D**ocumented thrombus (LAA or LV) - **A**trial fibrillation - **F**unctional impairment (NYHA Class III–IV) - **C**oagulation risk (hypercoagulable state) - **L**arge LA (>5 cm) - **O**ther risk factors (age >65, HTN, DM) - **T**ransient ischemic attack or stroke This patient meets **multiple** criteria (RHD + AF + documented thrombus + LA 5.5 cm). **Clinical Pearl:** Even if the thrombus is not visible on repeat echo, anticoagulation should continue indefinitely in RHD + AF (CHA₂DS₂-VASc score typically ≥2 in RHD patients). [cite:Robbins 10e Ch 12; Harrison 21e Ch 295] 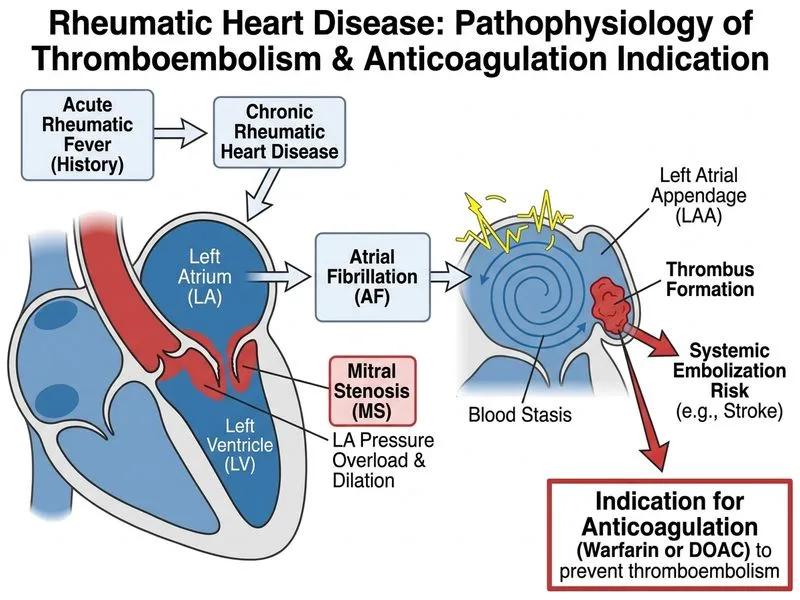
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.