## Diagnosis of Rocky Mountain Spotted Fever (RMSF) ### Clinical Context The patient presents with the classic tetrad of RMSF: fever, headache, petechial/maculopapular rash (trunk and extremities), and tick bite history. Thrombocytopenia and elevated transaminases are typical laboratory findings. ### Investigation Hierarchy for RMSF **Key Point:** Immunofluorescence antibody (IFA) test is the **gold standard and most specific confirmatory test** for RMSF in the acute phase. | Investigation | Organism Detected | Sensitivity | Specificity | Timing | Clinical Use | |---|---|---|---|---|---| | **IFA (IgM/IgG)** | Rickettsia rickettsii | 90–95% | 95–100% | Day 5–7 onwards | **Gold standard for acute diagnosis** | | Weil-Felix test | Heterophile antibodies | 50–80% | 50–70% | Day 5–7 onwards | Low specificity; not recommended | | Skin biopsy + IHC | Direct antigen in tissue | 70–90% | 95–100% | Any time | Invasive; reserved for unclear cases | | Electron microscopy | Rickettsial morphology | Variable | Variable | Early phase | Research tool; not practical | ### Why IFA Is Correct 1. **Highest specificity:** 95–100% specificity for Rickettsia rickettsii. 2. **Rapid positivity:** IgM antibodies appear by day 5–7 of illness (this patient is on day 5). 3. **Distinguishes RMSF from scrub typhus:** IFA can differentiate rickettsial species using species-specific antisera. 4. **Non-invasive:** Simple serology; no tissue biopsy needed. 5. **Widely available:** Standard reference laboratory test in most centers. **High-Yield:** IFA is the **reference standard** for rickettsial diagnosis and is recommended by CDC for RMSF confirmation. ### Role of Other Tests **Weil-Felix Test:** - Detects heterophile antibodies against Proteus OX-19, OX-2, and OX-K strains. - **Low specificity (50–70%):** Cross-reacts with multiple rickettsial species; cannot differentiate RMSF from scrub typhus or other rickettsial diseases. - **Sensitivity 50–80%:** Many false negatives. - **Not recommended** for diagnosis; historical test only. **Skin Biopsy with Immunohistochemistry (IHC):** - **Highest sensitivity (70–90%)** and **specificity (95–100%)** for direct detection of rickettsiae in tissue. - Useful when diagnosis is unclear or IFA is negative despite high clinical suspicion. - **Invasive procedure:** Requires biopsy from petechial lesion or eschar. - **Not first-line:** Reserved for confirmation in atypical presentations or when serology is negative. - Requires specialized immunohistochemistry expertise. **Electron Microscopy:** - Can visualize rickettsial morphology (pleomorphic coccobacilli). - **Not practical** for routine diagnosis; requires specialized equipment and expertise. - **Low sensitivity:** Difficult to find organisms in blood smears. - **Research tool only.** **Clinical Pearl:** Tick bite + fever + petechial rash + thrombocytopenia in a non-endemic area (Himachal Pradesh has sporadic RMSF cases) should raise suspicion for RMSF. IFA is the confirmatory test of choice. ### Diagnostic Algorithm for Rickettsial Diseases ```mermaid flowchart TD A[Suspected rickettsial infection]:::outcome --> B{Clinical presentation?}:::decision B -->|Eschar + regional LAD| C[Scrub typhus]:::outcome B -->|Petechial rash + tick bite| D[RMSF]:::outcome C --> E[IgM ELISA vs PCR]:::action D --> F[IFA against R. rickettsii]:::action E --> G{Positive?}:::decision F --> H{Positive?}:::decision G -->|Yes| I[Confirm scrub typhus]:::outcome H -->|Yes| J[Confirm RMSF]:::outcome G -->|No| K[Consider skin biopsy + IHC]:::action H -->|No| K ``` 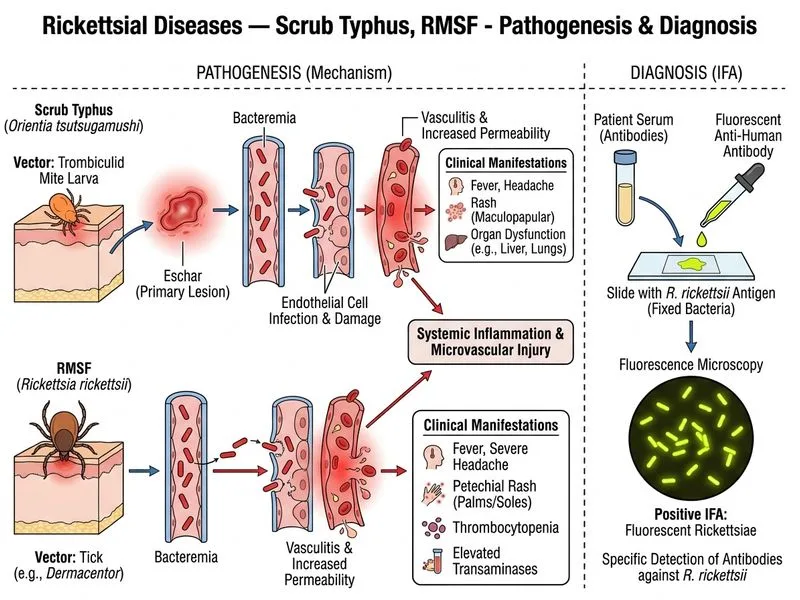
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.