## Diagnosis: Pleomorphic Adenoma **Key Point:** Pleomorphic adenoma is the most common benign salivary gland tumor, accounting for 60–80% of parotid tumors and 40–50% of submandibular tumors. ### Clinical Features Supporting Diagnosis - **Slow growth:** 6-month history is typical; often present for years before diagnosis - **Firm, non-tender mass:** characteristic of benign tumors - **Fixed to surrounding tissue:** suggests capsular involvement but NOT invasion - **Intact facial nerve:** rules out aggressive malignancy - **Superficial lobe location:** most common site (80% of parotid tumors arise here) ### FNAC Findings - **Cribriform (sieve-like) pattern:** hallmark of pleomorphic adenoma - **Mixed epithelial and myoepithelial cells:** defines the "pleomorphic" (many-shaped) nature - **Chondroid/hyaline stroma:** may be visible on cytology ### Pathology Snapshot | Feature | Pleomorphic Adenoma | |---------|---------------------| | Origin | Intercalated duct cells | | Growth rate | Slow (years) | | Facial nerve involvement | Rare (intact function) | | Malignant potential | 2–5% over 15–20 years (carcinoma ex pleomorphic adenoma) | | Treatment | Superficial or total parotidectomy with facial nerve preservation | **High-Yield:** The cribriform pattern on FNAC is pathognomonic for pleomorphic adenoma and is the single most useful diagnostic clue. **Clinical Pearl:** Although benign, pleomorphic adenoma should be surgically excised because of the risk of malignant transformation (carcinoma ex pleomorphic adenoma), especially if left untreated for >15 years. ### Why Superficial Parotidectomy? Since the mass is in the superficial lobe and facial nerve function is intact, superficial parotidectomy with facial nerve preservation is the gold standard. This removes the tumor with adequate margins while preserving the nerve. [cite:Robbins 10e Ch 17] 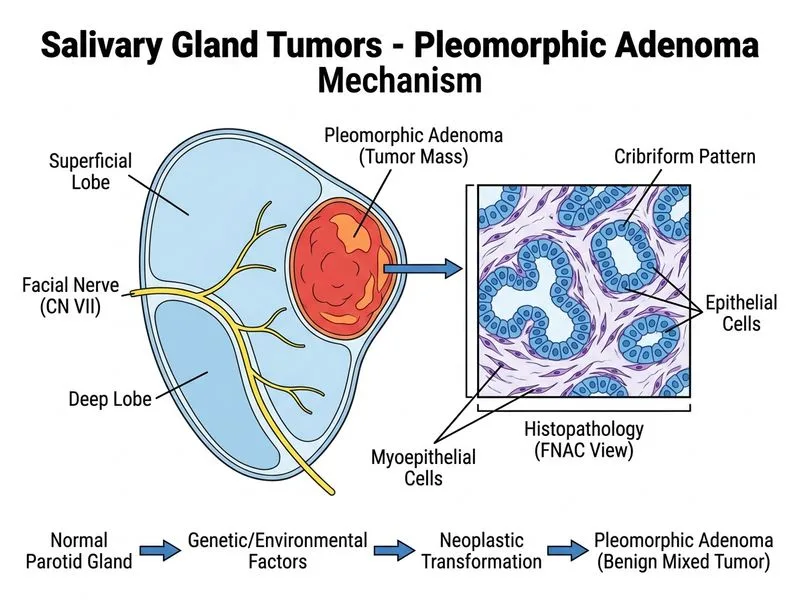
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.