## Diagnosis: Carcinoma ex Pleomorphic Adenoma ### Clinical Presentation The patient presents with **classic red flag features of malignant transformation in a salivary gland tumor**: - **Long-standing mass (2 years)** with **recent acceleration** of growth — hallmark of carcinoma ex PA - New onset **pain** (perineural/tissue invasion) - **Skin erythema and ulceration** (direct invasion) - **Fixation** to underlying tissues - **Intraoral displacement** of soft palate (mass effect from submandibular/parapharyngeal extension) ### Why Carcinoma ex Pleomorphic Adenoma (and NOT Primary SCC)? **High-Yield:** The single most important distinguishing feature in this vignette is the **2-year history of a pre-existing, slowly growing submandibular mass** that has recently undergone rapid change. Primary squamous cell carcinoma of the submandibular gland is exceedingly rare (the submandibular gland has virtually no squamous epithelium), whereas carcinoma ex pleomorphic adenoma is a well-recognized entity accounting for **3–15% of salivary gland malignancies** (Scott-Brown's Otorhinolaryngology; Cummings Otolaryngology). The FNAC showing **squamoid cells with high mitotic activity and keratinization** reflects the **malignant epithelial component** of carcinoma ex PA — the most common malignant component in carcinoma ex PA is indeed a poorly differentiated carcinoma with squamoid/undifferentiated features. The long pre-existing history anchors the diagnosis to malignant transformation rather than de novo SCC. **Key Point:** Per Cummings Otolaryngology (7th ed.), carcinoma ex pleomorphic adenoma is defined as a carcinoma arising within or from a pre-existing pleomorphic adenoma. The risk of malignant transformation increases with duration: ~1.5% at <5 years, rising to ~9.5% at >15 years. ### Diagnostic Criteria Met in This Case 1. ✅ **Long-standing mass** (2 years) followed by **rapid growth, pain, and skin involvement** 2. ✅ **Malignant cytology** on FNAC (high mitotic rate, squamoid cells, keratinization = malignant epithelial component) 3. ✅ **Clinical signs of malignancy** (fixation, skin ulceration, soft palate displacement) 4. ✅ **CT: heterogeneous mass with necrosis** (consistent with high-grade malignancy) ### Differential Diagnosis | Tumor | Key Feature | Why Less Likely Here | | --- | --- | --- | | **Carcinoma ex PA** ✓ | Pre-existing long-standing mass → rapid change | Best fits 2-year history + malignant FNAC | | Squamous cell carcinoma | De novo; submandibular gland has no squamous epithelium | Extremely rare as primary; no pre-existing mass history | | Adenoid cystic carcinoma | Basaloid cells, cribriform pattern, perineural invasion | FNAC would show basaloid/cribriform, not squamoid keratinizing cells | | Undifferentiated carcinoma | Pleomorphic cells, no keratinization | FNAC would lack keratinization | ### Clinical Pearl **Warning:** Any patient with a **long-standing salivary gland mass** who develops **sudden pain, rapid growth, skin involvement, or fixation** must be suspected for **carcinoma ex pleomorphic adenoma** until proven otherwise. This is a classic NEET PG / INI-CET high-yield scenario. Primary SCC of the submandibular gland is a diagnosis of exclusion and requires histological absence of any pre-existing pleomorphic adenoma component. ### Management 1. **Wide surgical resection** (submandibulectomy ± adjacent tissue) 2. **Neck dissection** (high nodal metastasis risk) 3. **Adjuvant radiation therapy** (improves locoregional control) 4. Chemotherapy for advanced/metastatic disease [cite: Cummings Otolaryngology 7e Ch 85; Scott-Brown's Otorhinolaryngology 8e; Harrison 21e Ch 94] 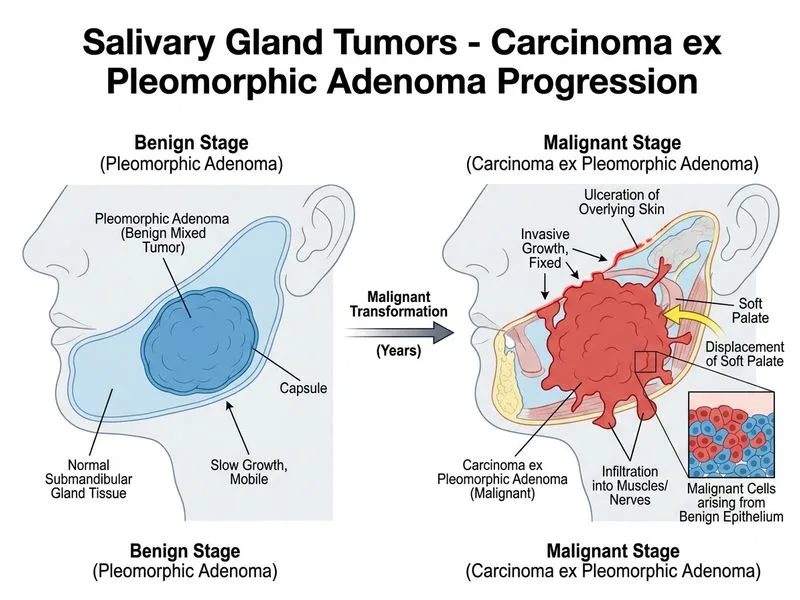
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.