## Pleomorphic Adenoma: The Most Common Salivary Tumor ### Clinical Presentation **Key Point:** Pleomorphic adenoma is the most common salivary gland tumor (60% of parotid tumors), presenting as a slow-growing, painless, mobile mass. **High-Yield:** The classic presentation — long duration (months to years), painless swelling, no facial nerve involvement — is pathognomonic for pleomorphic adenoma. ### Epidemiology & Location | Feature | Pleomorphic Adenoma | |---------|---------------------| | **Frequency** | 60% of parotid tumors; 50% of submandibular tumors | | **Age of onset** | 40–60 years | | **Growth rate** | Slow (years) | | **Pain** | Absent unless malignant transformation | | **Facial nerve involvement** | Rare (only if transformed) | ### Pathological Features 1. **Mixed tumor** — epithelial and mesenchymal (myoepithelial) components 2. **Well-circumscribed** — pseudo-encapsulated, not truly encapsulated 3. **Benign histology** — no cellular atypia, mitoses, or necrosis 4. **Pleomorphic appearance** — variable histological patterns (hence the name) **Mnemonic:** **P**leomorphic = **P**erfectly benign (unless left untreated for decades). ### Malignant Transformation Risk **Key Point:** Pleomorphic adenoma has a 5–15% risk of malignant transformation, typically after prolonged duration (>5 years). - **Risk increases with time** — tumors present >5 years have higher transformation risk - **Carcinoma ex pleomorphic adenoma** — the transformed malignancy; highly aggressive - **Triggers for transformation:** - Incomplete surgical excision with recurrence - Long-standing untreated tumor - Radiation exposure - Repeated fine-needle aspiration (controversial) ### Management 1. **Superficial or total parotidectomy** — with facial nerve preservation 2. **Avoid enucleation** — risk of spillage and recurrence 3. **Avoid repeated FNA** — may increase transformation risk 4. **Prognosis** — excellent if treated surgically; 5-year recurrence rate ~2–5% **Clinical Pearl:** A patient with a "benign" parotid tumor that suddenly enlarges or becomes painful should raise suspicion for malignant transformation. ### Why Other Options Are Wrong | Tumor | Why Not the Answer | |-------|--------------------| | **Mucoepidermoid Ca** | Malignant from onset (not benign with transformation risk); more common in younger patients; often presents with pain/nerve involvement | | **Acinic Cell Ca** | Low-grade malignancy; 80% is too high a malignant potential; usually low-risk with excellent prognosis | | **Adenoid Cystic Ca** | Malignant from onset; 100% malignancy; presents with facial nerve paralysis and perineural invasion | 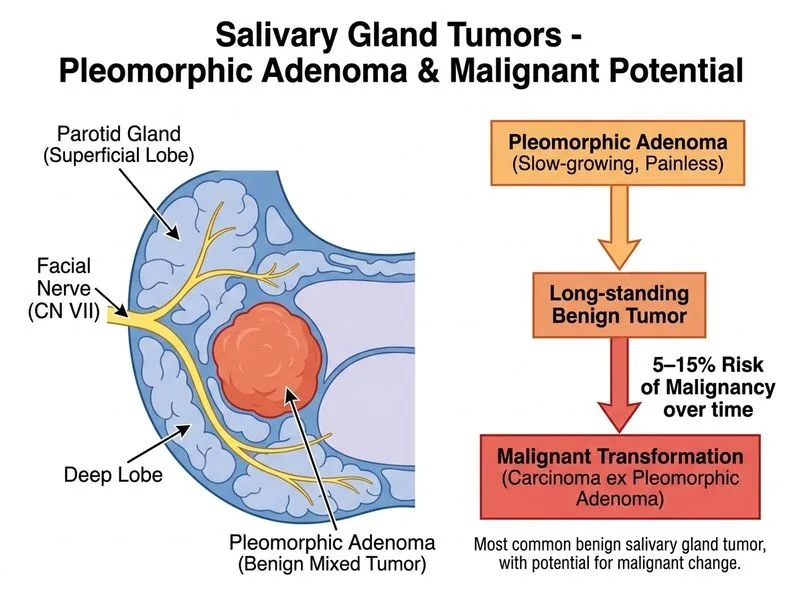
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.