## Distinguishing Pleomorphic Adenoma from Mucoepidermoid Carcinoma ### Clinical Presentation Comparison | Feature | Pleomorphic Adenoma | Mucoepidermoid Carcinoma | |---------|-------------------|------------------------| | **Growth rate** | Slow (months to years) | Rapid (weeks to months) | | **Facial nerve involvement** | Absent | Present (paralysis common) | | **Skin fixation** | Absent; skin mobile | Present; fixed to skin | | **Pain** | Absent | Often present | | **Overlying skin** | Intact, normal | Erythematous, ulcerated | | **Prognosis** | Excellent (benign) | Variable (low to high grade) | ### Key Point: **Rapid growth with facial nerve paralysis and skin fixation is the hallmark of mucoepidermoid carcinoma and distinguishes it from the indolent pleomorphic adenoma.** ### Clinical Pearl: Facial nerve involvement in a parotid mass is a RED FLAG for malignancy. Pleomorphic adenoma, despite being the most common parotid tumor overall, does NOT typically cause nerve compression or paralysis unless it reaches massive size or undergoes malignant transformation (carcinoma ex pleomorphic adenoma). ### High-Yield: Mucoepidermoid carcinoma is the **most common malignant parotid tumor** in adults. Its aggressive behavior (rapid growth, nerve invasion, skin involvement) contrasts sharply with the benign, slow-growing pleomorphic adenoma. This distinction is critical for surgical planning: pleomorphic adenoma requires superficial or total parotidectomy with facial nerve preservation; mucoepidermoid carcinoma often requires wide excision with possible neck dissection and adjuvant therapy. ### Mnemonic: **RAPID** = Rapid growth, Aggressive behavior, Paralysis of facial nerve, Infiltration of skin, Diagnosis: malignancy (Mucoepidermoid). [cite:Robbins 10e Ch 16] 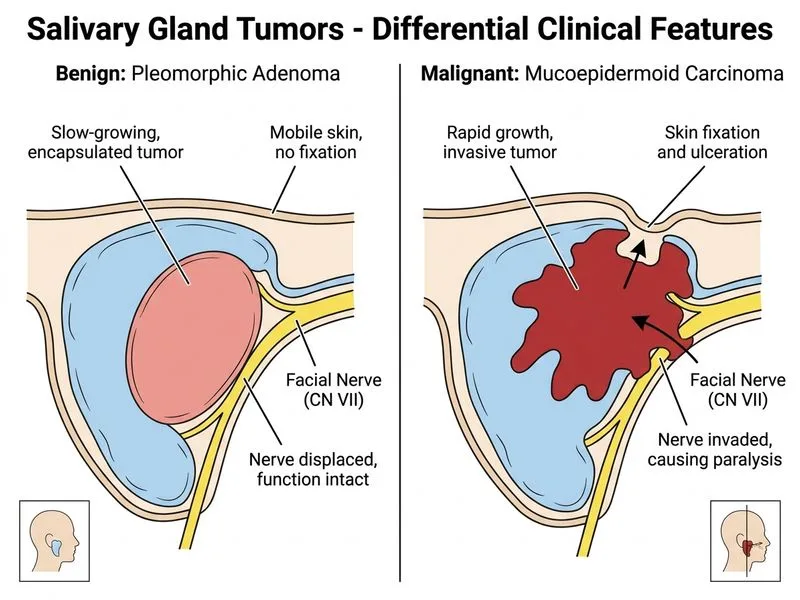
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.