## Clinical Context and Complication Risk **Key Point:** Scabies complicated by secondary bacterial infection (impetigo) is one of the most common and clinically significant complications, particularly in tropical climates like India where hygiene and overcrowding facilitate bacterial superinfection. **High-Yield:** Topical corticosteroids, while temporarily reducing itching, suppress local immunity and increase the risk of secondary bacterial infection. This is a common pitfall in scabies management. ## Complications of Scabies ```mermaid flowchart TD A[Scabies Infestation]:::outcome --> B{Untreated or Mismanaged}:::decision B -->|Scratching + Poor Hygiene| C[Secondary Bacterial Infection]:::urgent B -->|Immunosuppression/Corticosteroids| D[Crusted Scabies]:::urgent B -->|Chronic Inflammation| E[Scabies Nodules]:::outcome B -->|Severe Scratching| F[Post-inflammatory Changes]:::outcome C --> G[Impetigo, Cellulitis, Abscess]:::urgent D --> H[Hyperkeratotic plaques, High mite load]:::urgent E --> I[Pruritic nodules on genitals/buttocks]:::outcome F --> J[Hyperpigmentation, mild scarring]:::outcome G --> K[Risk: Acute Glomerulonephritis, Rheumatic Fever]:::urgent ``` ## Why Secondary Bacterial Infection is Most Likely | Complication | Incidence | Risk Factors | Clinical Features | Outcome | |--------------|-----------|--------------|-------------------|----------| | **Secondary Impetigo** | 10–15% | Scratching, poor hygiene, corticosteroids | Pustules, crusts, honey-colored exudate | AGN, RF if untreated | | **Crusted Scabies** | 1–3% | Immunosuppression (HIV, malignancy) | Hyperkeratotic plaques, high mite burden | Highly contagious, difficult to treat | | **Scabies Nodules** | 5–10% | Chronic inflammation, delayed treatment | Firm nodules on genitals/buttocks | Pruritic, may persist months | | **Post-inflammatory Changes** | Common | Severe scratching | Hyperpigmentation, mild atrophy | Cosmetic concern only | **Clinical Pearl:** In India, scabies complicated by impetigo is a major cause of acute post-streptococcal glomerulonephritis (APSGN) and acute rheumatic fever (ARF), especially in children and young adults. This makes early recognition and treatment critical. **High-Yield:** The patient's use of topical corticosteroids for 2 weeks is a major red flag. Corticosteroids: - Suppress local Th1 immunity - Reduce inflammatory response to mite antigens - Increase risk of secondary bacterial infection - May worsen scabies by allowing mite proliferation ## Pathophysiology of Secondary Infection 1. **Mite-induced inflammation** → intense pruritus 2. **Scratching** → disruption of skin barrier 3. **Bacterial colonization** → *Staphylococcus aureus* (most common) or *Streptococcus pyogenes* 4. **Impetigo** → pustules, crusts, exudate 5. **Systemic complications** → APSGN (if streptococcal), cellulitis, abscess ## Management of Scabies with Secondary Infection **Key Point:** Treat both the scabies AND the bacterial infection simultaneously. 1. **Acaricide:** Permethrin 5% cream (apply twice, 7 days apart) 2. **Antibiotics:** - Topical: Mupirocin 2% for localized impetigo - Systemic: Amoxicillin-clavulanate 625 mg TDS or cephalexin 500 mg QID for 7–10 days 3. **Avoid corticosteroids** until scabies is treated 4. **Symptomatic relief:** Antihistamines (cetirizine 10 mg daily) 5. **Hygiene:** Daily bathing, clean clothing, nail trimming to prevent scratching **Mnemonic:** **SCABIES + IMPETIGO** = **S**cabies treatment (permethrin), **C**ease corticosteroids, **A**ntibiotics (systemic), **B**acteria (culture if severe), **I**ntense hygiene, **E**arly intervention, **S**ymptomatic relief ## Why Other Options Are Less Likely **Crusted scabies** (Option A): - Occurs primarily in immunocompromised patients (HIV/AIDS, malignancy, immunosuppressive therapy) - No mention of immunosuppression in this case - Requires systemic ivermectin + topical acaricide - Less common than secondary bacterial infection **Scabies nodules** (Option C): - Develop in 5–10% of scabies cases - Represent hypersensitivity reaction to mite antigens - Occur on genitals, buttocks, and axillae - Are pruritic but do not lead to systemic complications - Develop over weeks to months, not acutely **Post-inflammatory changes** (Option D): - Cosmetic concern only - Do not represent an acute complication - Occur after resolution of scabies - Mild scarring is rare; hyperpigmentation is common but reversible 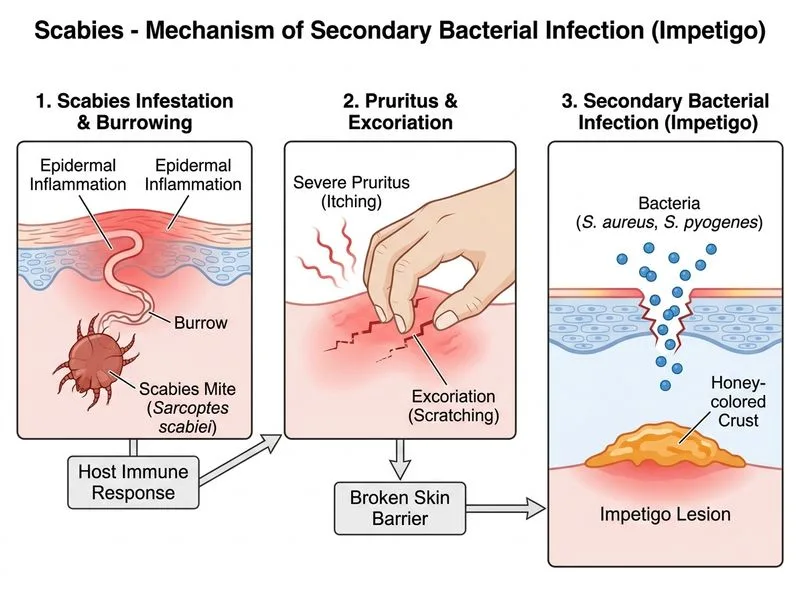
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.