## Crusted (Norwegian) Scabies in Immunocompromised Host ### Clinical Recognition **Key Point:** The combination of **severe immunosuppression** (CD4 <50), **extensive crusted plaques** (palms, soles, face), **high mite burden** (hundreds per field), and **minimal pruritus** is pathognomonic for **crusted scabies**. ### Why Crusted Scabies Is Different **High-Yield:** Crusted scabies occurs almost exclusively in severely immunocompromised patients (HIV CD4 <50, hematologic malignancy, organ transplant). The host cannot mount an adequate immune response, allowing mites to proliferate unchecked (up to 1 million per patient vs. 10–15 in classical scabies). #### Pathophysiology - Defective Th1/Th2 response → impaired itch sensation - Massive mite replication → hyperkeratotic crusted lesions - High transmissibility → infection control priority ### Treatment Algorithm for Crusted Scabies ```mermaid flowchart TD A[Crusted Scabies Diagnosis]:::outcome --> B{Severity & CD4 Count?}:::decision B -->|CD4 <50, extensive| C[Ivermectin 200 mcg/kg]:::action C --> D[Repeat at Day 7 & Day 14]:::action D --> E[Add topical sulfur 10% daily]:::action E --> F[Immune reconstitution with ART]:::action F --> G[Cure achieved]:::outcome B -->|Mild/localized| H[Permethrin monotherapy]:::action H --> I[May fail; escalate to ivermectin]:::urgent ``` ### Ivermectin for Crusted Scabies **Clinical Pearl:** Ivermectin is the treatment of choice for crusted scabies because: 1. **Systemic penetration** → reaches mites in thick crusts where topical agents fail 2. **High mite burden** → requires multiple doses (day 1, 7, 14) to kill successive generations 3. **Immunocompromised host** → cannot rely on host immune response; need aggressive pharmacotherapy #### Ivermectin Dosing for Crusted Scabies - **Dose:** 200 mcg/kg orally - **Schedule:** Day 1, then repeat at day 7 and day 14 (minimum 3 doses) - **Adjunct:** Topical sulfur 10% ointment daily during treatment - **Monitoring:** Clinical response by week 4; repeat if necessary ### Comparison: Topical vs. Systemic in Crusted Scabies | Agent | Route | Efficacy in Crusted | Rationale | Limitations | |-------|-------|-------------------|-----------|-------------| | **Ivermectin** | Oral | **Excellent** | Penetrates crusts; systemic; multiple doses | Teratogenic; requires repeat dosing | | Permethrin 5% | Topical | **Poor** | Cannot penetrate thick crusts | High failure rate; inadequate for crusted disease | | Sulfur 10% | Topical | **Moderate** | Adjunctive; slow-acting | Never monotherapy for crusted; requires weeks | | Crotamiton 10% | Topical | **Poor** | Insufficient penetration | Not recommended for crusted scabies | **Mnemonic:** **CRISP** — **C**rusted scabies, **R**equires **I**vermectin **S**ystemic, **P**lus topical sulfur. ### Why Permethrin Fails Here **Warning:** Permethrin is ineffective in crusted scabies because the thick hyperkeratotic crusts prevent adequate drug penetration. Topical agents alone have failure rates >50% in this population. Permethrin should NOT be used as monotherapy for crusted disease. ### Immune Reconstitution **Clinical Pearl:** Concurrent initiation or optimization of antiretroviral therapy (ART) is essential. As CD4 count recovers (>200), the host immune response improves and scabies may spontaneously resolve or become easier to treat. [cite:Irvine 3e Ch 8; Harrison 21e Ch 197] 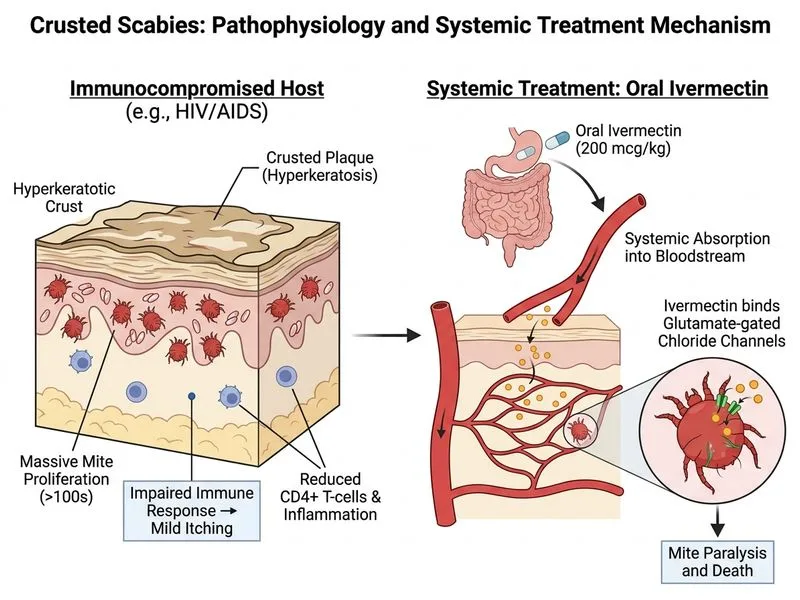
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.