## Diagnosis and Rationale **Key Point:** Scabies is a highly contagious infestation caused by *Sarcoptes scabiei* that spreads through prolonged skin-to-skin contact, making household-wide treatment essential even if asymptomatic. ## Management Principles ### Why Household Treatment is Mandatory - Scabies spreads to close contacts (family members) before symptoms appear, often within 2–6 weeks of exposure. - Asymptomatic family members harbour mites and will develop symptoms if left untreated. - Failure to treat all household contacts leads to re-infestation cycles. ### First-Line Treatment: Topical Permethrin | Parameter | Details | |-----------|----------| | **Agent** | Permethrin 5% cream | | **Application** | Apply to entire body surface (neck to toes, including intertriginous areas) | | **Timing** | Leave on for 8–14 hours (typically overnight) | | **Repeat** | After 7 days (to kill newly hatched mites) | | **Advantage** | Safe in pregnancy, infants >2 months, and breastfeeding | **High-Yield:** The 7-day repeat application is critical because the first application kills adult mites and nymphs but may not reliably kill eggs; the second application targets newly emerged mites. ### Why Other Options Are Suboptimal **Clinical Pearl:** Treating only symptomatic members leaves asymptomatic carriers untreated, perpetuating transmission within the household. - **Ivermectin (oral):** Reserved for crusted scabies, immunocompromised patients, or when topical therapy is impractical; not first-line for typical scabies in an immunocompetent family. - **Sulfur ointment:** Slower acting, requires daily application for 5–7 days, and is less effective than permethrin; reserved for infants <2 months and pregnant women. - **Localized application only:** Scabies is a systemic infestation; burrows and mites can be present on any body surface, including the scalp, genitalia, and soles. ## Post-Treatment Advice 1. Wash all bedding, towels, and clothing in hot water (>60°C) and dry at high heat. 2. Items that cannot be washed should be sealed in a plastic bag for ≥72 hours. 3. Pruritus may persist for 2–4 weeks post-treatment due to residual inflammation; antihistamines or topical steroids may be used. 4. Patients should be reviewed at 2 weeks to assess treatment response and retreat if necessary. **Warning:** Secondary bacterial infection (impetigo) is common due to scratching; educate the patient on avoiding excoriation and consider prophylactic antiseptic measures. 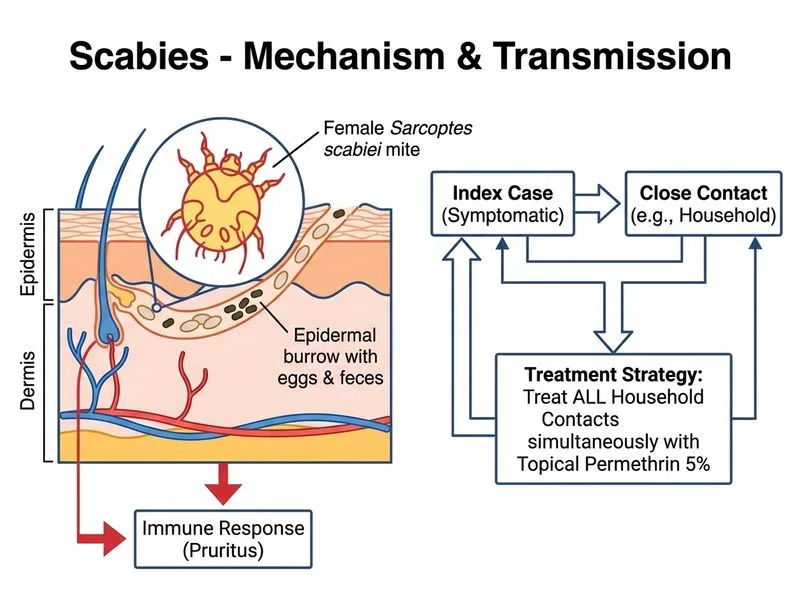
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.