## Diagnosis and Management of Scabies ### Clinical Presentation Recognition **Key Point:** The combination of nocturnal pruritus, burrows on characteristic sites (wrists, interdigital spaces, abdomen), and household contact with similar symptoms is pathognomonic for scabies. **High-Yield:** Burrows are the hallmark lesion — they are linear or S-shaped tunnels in the stratum corneum created by the gravid female mite. KOH mount confirmation showing the mite, eggs, or feces is diagnostic. ### First-Line Treatment Algorithm ```mermaid flowchart TD A[Confirmed Scabies]:::outcome --> B{Patient age & pregnancy status?}:::decision B -->|Adult, non-pregnant| C[Permethrin 5% cream]:::action B -->|Child < 2 yrs or pregnant| D[Sulfur 10% ointment]:::action B -->|Severe/crusted or immunocompromised| E[Ivermectin + topical]:::action C --> F[Apply to entire body neck down]:::action C --> G[Repeat after 1 week]:::action D --> H[Apply daily for 3 days]:::action F --> I[Treat household contacts simultaneously]:::action G --> I ``` ### Why Permethrin 5% is First-Line | Feature | Permethrin 5% | Ivermectin | Sulfur 10% | Lindane | |---------|---------------|-----------|-----------|----------| | **Efficacy** | 95% (single application) | 95% (needs 2 doses) | 90% | 90% | | **Safety** | Safe in children, pregnancy | Avoid in pregnancy, <15 kg | Safe in all ages | Neurotoxicity risk | | **Application** | Once, repeat week 1 | Oral, systemic | Daily × 3 days | Single application | | **Resistance** | Rare | Emerging in some areas | None | Increasing | | **Cost** | Moderate | Higher | Low | Low | **Clinical Pearl:** Permethrin is the WHO-recommended first-line agent because it has excellent efficacy, minimal systemic absorption, and a favorable safety profile even in young children and pregnant women. ### Treatment Protocol 1. **Application:** Apply permethrin 5% cream to entire body from neck downward, including intertriginous areas, palms, soles, and genital region. 2. **Duration:** Leave on skin for 8–14 hours (typically overnight), then wash off. 3. **Repeat:** Apply again 1 week later to catch any mites that may have hatched from eggs missed in the first application. 4. **Household contacts:** All household members and close contacts should be treated simultaneously, even if asymptomatic, to prevent reinfection. 5. **Fomite management:** Wash bedding, clothing, and towels in hot water; items that cannot be washed should be sealed in a plastic bag for 1 week. **High-Yield:** The 1-week repeat application is crucial because permethrin does not reliably kill eggs; the second application targets mites that emerge from unhatched eggs. ### Why Other Options Are Not First-Line Here - **Ivermectin:** Requires 2 oral doses 1–2 weeks apart; reserved for crusted scabies, immunocompromised patients, or institutional outbreaks. Single dose is insufficient. - **Sulfur 10%:** Safe in infants and pregnancy but requires daily application for 3 days; more cumbersome than permethrin and less cosmetically acceptable. - **Lindane:** Historically used but now largely avoided due to neurotoxicity risk (seizures, aplastic anemia) and increasing resistance; contraindicated in young children and pregnancy. **Warning:** Lindane is banned or restricted in many countries and should not be used as first-line therapy. ### Prognosis and Follow-Up **Key Point:** Pruritus may persist for 2–4 weeks after successful treatment due to residual inflammation and mite antigen; this does not indicate treatment failure. - Review at 2 weeks to assess clinical response. - If burrows or new lesions persist, repeat permethrin application or switch to ivermectin. - Educate patient on household decontamination and simultaneous treatment of contacts to prevent reinfection. 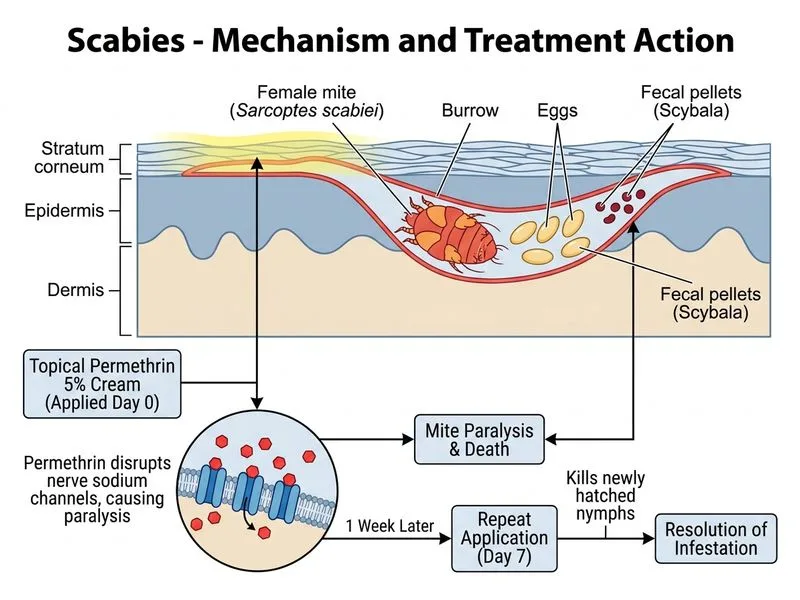
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.