## Crusted Scabies: Recognition and Management ### Clinical Diagnosis **Key Point:** This patient has crusted scabies (also called Norwegian scabies), characterized by widespread distribution, thick crusts, high mite burden (>1 million mites vs. 10–15 in typical scabies), and failure to respond to standard topical therapy. **High-Yield:** Crusted scabies occurs in: - Immunocompromised patients (CD4 <200 cells/μL, advanced HIV/AIDS) - Elderly patients with poor hygiene or immobility - Patients with severe malnutrition or systemic illness - Individuals on immunosuppressive therapy **Clinical Pearl:** The presence of >50% body surface involvement, thick crusts, and failure after two courses of permethrin strongly suggests crusted scabies rather than typical scabies. ### Why Standard Topical Therapy Fails in Crusted Scabies ```mermaid flowchart TD A[Crusted Scabies]:::outcome --> B[Massive mite burden]:::outcome B --> C[Thick keratinous crust barrier]:::outcome C --> D[Topical agents cannot penetrate adequately]:::outcome D --> E[Permethrin monotherapy fails]:::urgent E --> F[Requires systemic therapy]:::action F --> G[Oral ivermectin + topical permethrin]:::action ``` ### Treatment Algorithm for Crusted Scabies | Aspect | Typical Scabies | Crusted Scabies | |--------|-----------------|------------------| | **Mite burden** | 10–15 mites | >1 million mites | | **Presentation** | Burrows, papules | Thick crusts, nodules, widespread | | **First-line** | Permethrin 5% × 2 doses | Ivermectin + permethrin | | **Ivermectin dosing** | Not indicated | 200 μg/kg, repeat at 1–2 weeks | | **Topical agent** | Permethrin alone | Permethrin + sulfur or benzoyl benzoate | | **Crust removal** | Not needed | May require keratolytic pre-treatment | | **Hospitalization** | Rarely | Often required | | **Contact tracing** | Essential | Urgent; high transmissibility | **Key Point:** Oral ivermectin achieves systemic distribution and penetrates crusts; combined with topical permethrin, it provides synergistic efficacy. ### Recommended Management Protocol 1. **Oral ivermectin:** 200 μg/kg (typically 12 mg for adults), repeat dose after 1–2 weeks. 2. **Topical permethrin 5%:** Apply to entire body, especially under crusts; repeat weekly or twice weekly for 4 weeks. 3. **Optional crust removal:** Gentle debridement or keratolytic ointment (salicylic acid 10%) may enhance penetration of topical agents. 4. **Hospitalization:** Consider for: - Severe immunosuppression (CD4 <200) - Extensive body surface involvement - Secondary bacterial infection - Poor home hygiene or inability to self-treat 5. **Infection control:** Strict isolation precautions; simultaneous treatment of all household and healthcare contacts. 6. **Fomite management:** Aggressive decontamination of bedding, clothing, and environment. **High-Yield:** The combination of systemic ivermectin and topical permethrin is superior to either agent alone in crusted scabies; permethrin monotherapy has unacceptably high failure rates. ### Why This Patient Requires Ivermectin - **Failed topical therapy:** Two courses of permethrin indicate inadequate penetration through thick crusts. - **High mite burden:** Dermoscopy showing abundant mites, eggs, and feces confirms crusted scabies. - **Immunocompromise:** CD4 count of 450 cells/μL (approaching AIDS threshold) predisposes to severe infestation. - **Systemic absorption needed:** Oral ivermectin achieves therapeutic levels throughout the body, including under keratinous crusts. **Clinical Pearl:** Crusted scabies is a public health emergency due to high transmissibility; patients should be isolated and all contacts treated prophylactically. ### Prognosis and Monitoring - **Clinical response:** Expect improvement in pruritus within 1–2 weeks and resolution of crusts within 4–6 weeks. - **Persistent crusts:** May indicate inadequate treatment or reinfection; consider repeat ivermectin and intensified topical therapy. - **Secondary infection:** If present, treat with appropriate antibiotics (typically staphylococcal coverage). - **Follow-up:** Reassess at 2 weeks; if no improvement, consider hospitalization and more intensive regimen. 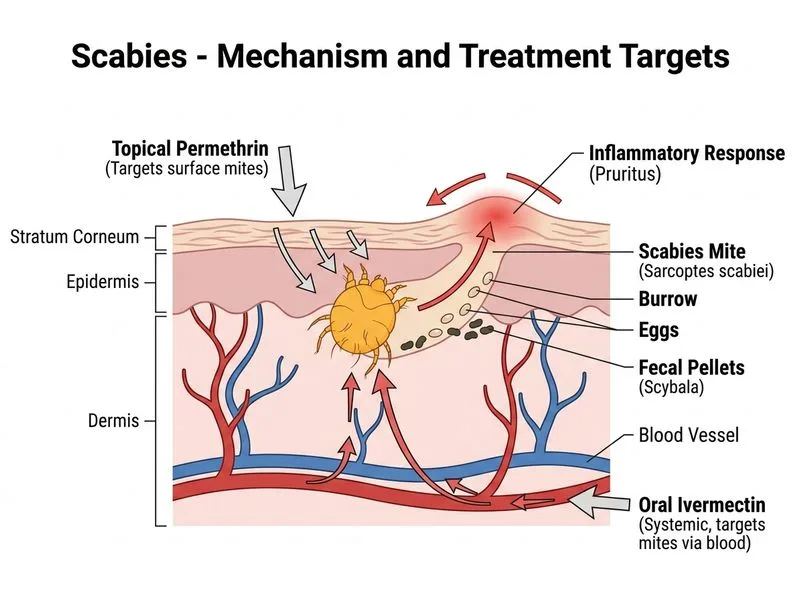
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.