## Diagnosis & Management of Scaphoid Non-Union **Key Point:** Persistent fracture line with fragment separation after 12 weeks of immobilization indicates **scaphoid non-union**, not delayed union. Non-union requires surgical intervention. ### Clinical Features of Non-Union **High-Yield:** Non-union is defined as: - Fracture line still visible on imaging **after 12–16 weeks of immobilization** - Absence of callus bridging - Persistent symptoms (pain, clicking, weakness) - Scaphoid waist fractures have higher non-union risk (10–15%) than tubercle fractures (< 5%) ### Risk Factors for Non-Union | Factor | Mechanism | |--------|----------| | Waist/proximal pole fracture | Poor blood supply (retrograde flow) | | Non-displaced fracture | Minimal periosteal stripping; less callus | | Delayed diagnosis | Occult fracture; inadequate early immobilization | | Smoking | Impaired osteoblast function | | Non-compliance | Inadequate immobilization | | Comminution | Increased fracture surface area | **Clinical Pearl:** The scaphoid has a **retrograde blood supply** entering at the waist and distal pole. Proximal pole fractures are at risk of avascular necrosis (AVN), but this patient's fracture is at the waist with persistent vascularity, making non-union more likely than AVN. ### Management Algorithm for Scaphoid Non-Union ```mermaid flowchart TD A[Scaphoid fracture + 12 weeks immobilization]:::outcome --> B{Imaging findings?}:::decision B -->|Fracture line visible + no callus| C[Non-union]:::outcome B -->|Partial callus bridging| D[Delayed union]:::outcome C --> E{Proximal pole involved?}:::decision E -->|No| F[Percutaneous screw fixation]:::action E -->|Yes| G[Assess vascularity with MRI]:::action G --> H{AVN present?}:::decision H -->|Yes| I[Vascularized bone graft + screw]:::action H -->|No| J[Percutaneous screw fixation]:::action D --> K[Continue immobilization 4-6 weeks]:::action K --> L{Union achieved?}:::decision L -->|Yes| M[Discharge]:::outcome L -->|No| N[Proceed to surgery]:::action ``` ### Surgical Options for Non-Union | Procedure | Indication | Success Rate | |-----------|-----------|---------------| | Percutaneous screw fixation | Non-union without AVN, adequate vascularity | 85–95% | | Open reduction + screw + bone graft | Comminuted, displaced, or with AVN | 80–90% | | Vascularized bone graft (e.g., 1,2-ICSRA) | Proximal pole AVN, failed prior surgery | 75–85% | | Wrist fusion (4-corner, STT) | Chronic non-union with SLAC wrist | 70–80% | **High-Yield:** Percutaneous screw fixation is the **gold standard** for uncomplicated scaphoid non-union (waist fracture, no AVN). It provides rigid fixation, allows early mobilization, and has high union rates (85–95%). ### Why NOT the Other Options? - **Delayed union:** Delayed union shows **partial callus bridging** and may resolve with continued immobilization. This patient has a persistent fracture line with no callus—this is non-union, not delayed union. - **Malunion with secondary OA:** Malunion occurs when the fracture heals in an abnormal position. This patient has a visible fracture line (non-union), not a healed fracture in bad position. Conservative treatment is inadequate for symptomatic non-union. - **AVN of proximal pole:** While AVN is a risk with proximal pole fractures, this is a **waist fracture** with persistent vascularity (evidenced by lack of sclerosis on X-ray). AVN would require vascularized bone graft, not simple screw fixation. **Mnemonic:** **WAIST NON-UNION = SCREW; PROXIMAL AVN = VASCULARIZED GRAFT** 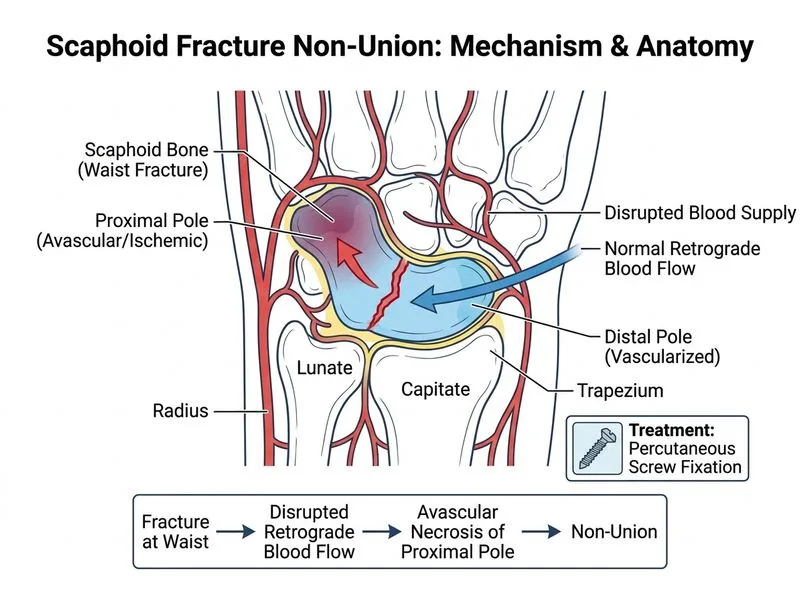
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.