## Clinical Scenario Analysis This patient presents with a classic **clinical suspicion of scaphoid fracture** — FOOSH mechanism, anatomical snuffbox tenderness, and pain on thumb axial loading — despite **normal initial radiographs**. This is a high-yield NEET PG scenario because 10–20% of scaphoid fractures are radiographically occult on initial imaging. ## Management Algorithm for Suspected Scaphoid Fracture ```mermaid flowchart TD A[FOOSH injury + snuffbox tenderness]:::outcome --> B{Radiographs show fracture?}:::decision B -->|Yes| C[Confirm with scaphoid views]:::action B -->|No, but high clinical suspicion| D[Immobilize in thumb spica cast]:::action D --> E[Repeat radiographs at 10-14 days]:::action E --> F{Fracture visible?}:::decision F -->|Yes| G[Continue immobilization per fracture type]:::action F -->|No, but persistent symptoms| H[MRI or CT for confirmation]:::action C --> I[Classify fracture: proximal/middle/distal]:::outcome I --> J{Displacement or comminution?}:::decision J -->|No| K[Conservative: thumb spica 8-12 weeks]:::action J -->|Yes| L[Surgical fixation]:::urgent ``` ## Key Point: The "Treat the Patient, Not the X-ray" Principle **High clinical suspicion + normal initial radiographs = immobilize and repeat imaging in 10–14 days.** This is the standard of care because: 1. **Fracture lines become visible** as callus forms and bone resorption occurs at the fracture site (10–14 days post-injury). 2. **Immobilization prevents displacement** of an occult fracture during the diagnostic period. 3. **Early immobilization improves union rates** and reduces risk of avascular necrosis (AVN) of the proximal pole. ## High-Yield Facts **Key Point:** Scaphoid fractures are **radiographically occult in 10–20% of cases** on initial presentation, especially if non-displaced. **Clinical Pearl:** The **anatomical snuffbox tenderness** (pain between extensor carpi radialis longus and brevis tendons) is the most sensitive clinical sign for scaphoid injury; **axial loading of the thumb** (longitudinal compression) is highly specific. **High-Yield:** Repeat radiographs at **10–14 days** show the fracture in ~90% of initially occult cases due to: - Bone resorption at fracture margins - Callus formation - Widening of fracture line ## Why Immobilization First? | Intervention | Timing | Rationale | |---|---|---| | **Thumb spica cast** | Immediately | Prevents displacement, reduces pain, allows early callus formation | | **Repeat radiographs** | 10–14 days | Fracture becomes radiographically visible | | **MRI/CT** | If repeat X-rays negative but symptoms persist | Definitive imaging if fracture still not visible | **Warning:** Do NOT discharge without immobilization — an occult fracture left untreated risks **nonunion, delayed union, and AVN of the proximal pole** (especially if proximal third fracture). ## Citation [cite:Rockwood & Green's Fractures in Adults Ch 7 — Scaphoid Fractures] 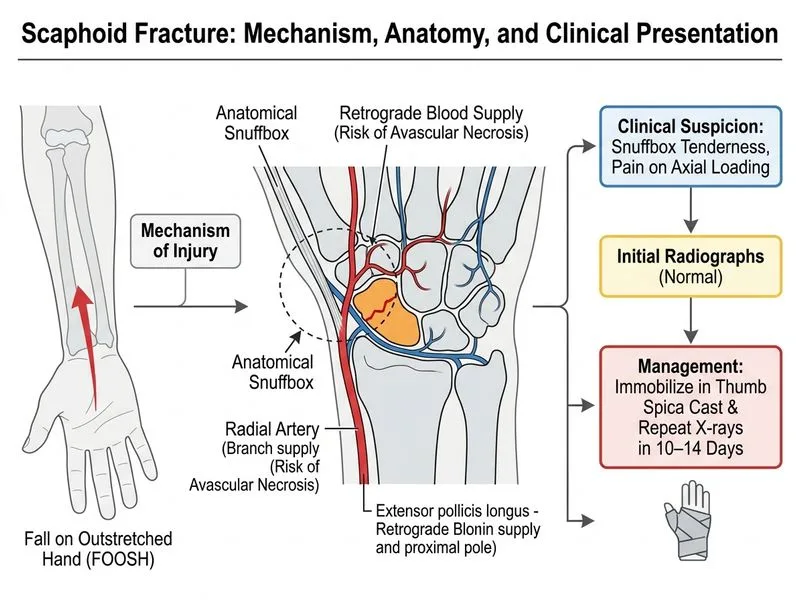
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.