## Clinical Presentation & Diagnosis **Key Point:** Scaphoid fractures are frequently occult on initial plain radiographs, especially non-displaced fractures. Clinical suspicion based on mechanism (FOOSH) and anatomical snuffbox tenderness must guide management. **High-Yield:** The gold standard approach for suspected scaphoid fracture with normal initial radiographs is **immobilization in a thumb spica cast and repeat imaging in 10–14 days**. During this period, bone resorption at the fracture site makes the fracture line more radiographically visible. ## Why Immobilization First? 1. **Prevents displacement** — early immobilization reduces the risk of converting a non-displaced fracture into a displaced one. 2. **Allows fracture line to become visible** — resorption of bone at fracture margins increases radiographic lucency. 3. **Cost-effective** — avoids unnecessary advanced imaging in the acute phase. 4. **Prevents complications** — early immobilization reduces avascular necrosis (AVN) risk by maintaining blood supply stability. ## Imaging Timeline | Timing | Imaging | Sensitivity | Use | |--------|---------|-------------|-----| | **Acute (Day 0–3)** | Plain X-rays (PA, lateral, scaphoid views) | 60–70% | Initial screening; may miss non-displaced fractures | | **10–14 days** | Repeat plain X-rays | 90–95% | Fracture line becomes visible due to resorption | | **If high suspicion + negative repeat X-rays** | CT or MRI | >95% | Confirms/excludes fracture; MRI also assesses soft tissue | **Clinical Pearl:** Anatomical snuffbox tenderness + FOOSH mechanism = treat as scaphoid fracture until proven otherwise, even with normal initial radiographs. The cost of immobilization is far less than the cost of missing a scaphoid fracture and developing AVN. **Mnemonic: FOOSH** — Fall On OutStretched Hand (classic mechanism for scaphoid injury). 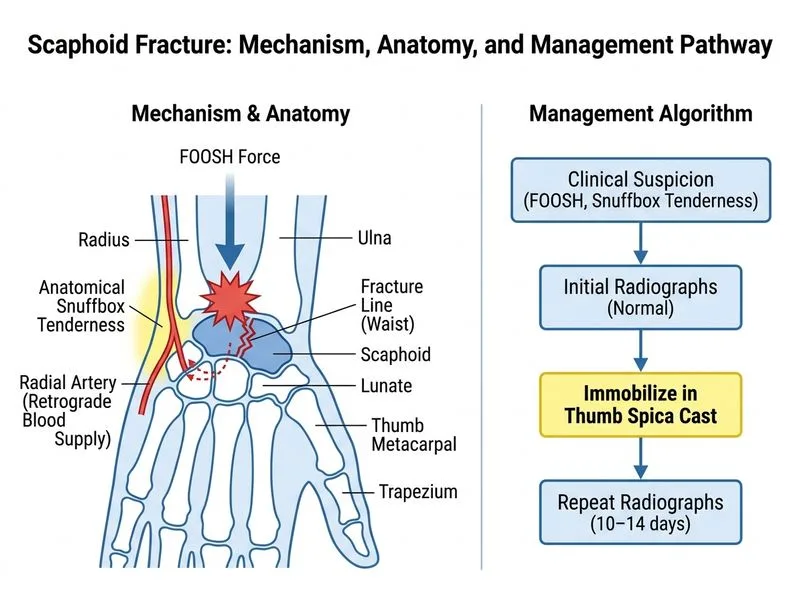
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.