## Investigation of Choice for Suspected Scaphoid Fracture with Normal Plain Radiographs ### Clinical Context Scaphoid fractures are frequently missed on initial plain radiographs, particularly non-displaced or minimally displaced fractures. When clinical suspicion is high (anatomical snuffbox tenderness, positive scaphoid compression test, mechanism of injury) but plain films are negative, advanced imaging is essential to avoid complications such as avascular necrosis (AVN) and nonunion. ### Why MRI is the Investigation of Choice **Key Point:** MRI is the gold standard for detecting occult scaphoid fractures and has the highest sensitivity (100%) and specificity (99%) for acute fractures, even within 24–48 hours of injury. **High-Yield:** MRI can: - Detect fracture lines not visible on plain radiographs - Assess bone marrow edema (earliest sign of fracture) - Evaluate soft tissue injuries (ligamentous injuries, cartilage damage) - Determine fracture displacement and angulation (important for treatment planning) - Identify complications (AVN, nonunion) in chronic cases ### Comparison of Imaging Modalities | Modality | Sensitivity | Specificity | Advantages | Disadvantages | |----------|-------------|-------------|-----------|---------------| | **MRI** | 100% | 99% | Detects bone marrow edema, soft tissue assessment, no radiation | Cost, time, contraindications (metallic implants) | | **CT Scan** | 95% | 98% | Good for fracture geometry, 3D reconstruction, faster than MRI | Radiation exposure, less sensitive for early edema | | **Bone Scan** | 90–95% | 85–90% | Detects metabolic activity, useful for dating fractures | Radiation, poor anatomical detail, delayed imaging (48–72 hrs) | | **Ultrasound** | 60–80% | Variable | No radiation, portable, operator-dependent | Poor specificity, limited by bone acoustic properties | **Clinical Pearl:** In acute scaphoid fracture suspicion with negative plain radiographs, MRI within 24–48 hours is preferred because it can detect bone marrow edema before fracture lines become radiographically visible. This allows early immobilization and prevents complications. ### Treatment Implications - **Confirmed fracture on MRI:** Immobilization (cast or splint) for 8–12 weeks (non-displaced) or surgical fixation (displaced, unstable). - **No fracture on MRI:** Reassurance; clinical follow-up; plain radiographs repeated at 10–14 days if symptoms persist (to detect stress-induced changes). **Mnemonic:** **SCAPHOID MRI** = **S**ensitivity 100%, **C**lear bone marrow edema, **A**cute detection, **P**erfect for occult fractures, **H**igh specificity, **O**ptimal soft tissue, **I**mmediate diagnosis, **D**ecision-making for treatment. 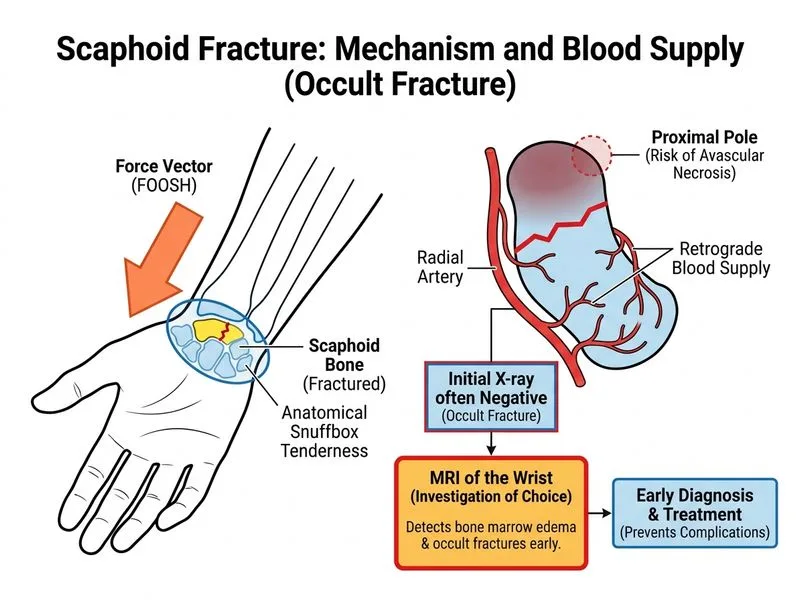
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.