## Investigation for Assessing Scaphoid Fracture Complications and Treatment Planning ### Clinical Context After confirmation of scaphoid fracture on MRI, subsequent imaging is needed to: 1. Assess fracture healing and union status 2. Evaluate fracture displacement or angulation (which may change treatment from conservative to surgical) 3. Detect complications (nonunion, malunion, AVN) 4. Guide surgical planning if intervention is required ### Why CT Scan with 3D Reconstruction is Most Appropriate **Key Point:** CT scan with 3D reconstruction is the gold standard for preoperative assessment and detailed fracture geometry evaluation in scaphoid fractures, particularly when surgical intervention is being considered. **High-Yield:** CT provides: - **Precise fracture geometry:** Fracture line orientation, comminution, angulation (critical for surgical approach selection) - **3D reconstruction:** Allows assessment of fracture displacement and alignment in all planes - **Nonunion/malunion detection:** Identifies hypertrophic or atrophic nonunion patterns - **Surgical planning:** Determines optimal fixation method (screw placement, bone graft need) - **Faster imaging:** Quicker than MRI, suitable for acute decision-making ### Comparison of Imaging Modalities in Chronic/Complicated Scaphoid Fractures | Modality | Best For | Advantages | Limitations | |----------|----------|-----------|-------------| | **CT with 3D** | Fracture geometry, surgical planning, nonunion assessment | Precise anatomy, 3D reconstruction, fast | Radiation, less sensitive for AVN | | **Repeat MRI** | Vascular assessment, AVN detection, soft tissue | Excellent for AVN (T2 hyperintensity), no radiation | Slower, expensive, less detail on fracture geometry | | **Bone Scan** | Metabolic activity, healing assessment | Detects nonunion (cold spot) | Poor anatomical detail, delayed imaging, radiation | | **Plain Radiographs** | Initial assessment, follow-up at 6–8 weeks | Simple, quick, low cost | Poor sensitivity for early complications, limited detail | **Clinical Pearl:** In the context of persistent pain 3 weeks post-injury with a confirmed non-displaced fracture, CT is superior because it can detect subtle displacement or angulation that may have occurred during healing, and it provides the anatomical detail needed if surgical fixation becomes necessary. ### Fracture Geometry and Treatment Decision ```mermaid flowchart TD A[Confirmed scaphoid fracture on MRI]:::outcome --> B{Persistent symptoms or displacement suspected?}:::decision B -->|Yes| C[CT with 3D reconstruction]:::action B -->|No| D[Continue conservative management]:::action C --> E{Fracture geometry assessment}:::decision E -->|Non-displaced, good alignment| F[Continue immobilization]:::action E -->|Displaced or angulated| G[Surgical fixation indicated]:::action E -->|Nonunion pattern| H[Assess for AVN with MRI]:::action G --> I[Preoperative planning complete]:::outcome ``` **Mnemonic:** **CT 3D SCAPHOID** = **C**lear fracture geometry, **T**hree-dimensional detail, **S**urgical planning, **C**omplications detected, **A**ngulation assessment, **P**recise anatomy, **H**elps decide conservative vs. operative, **O**ptimal for nonunion, **I**mmediate decision-making, **D**etails for fixation. 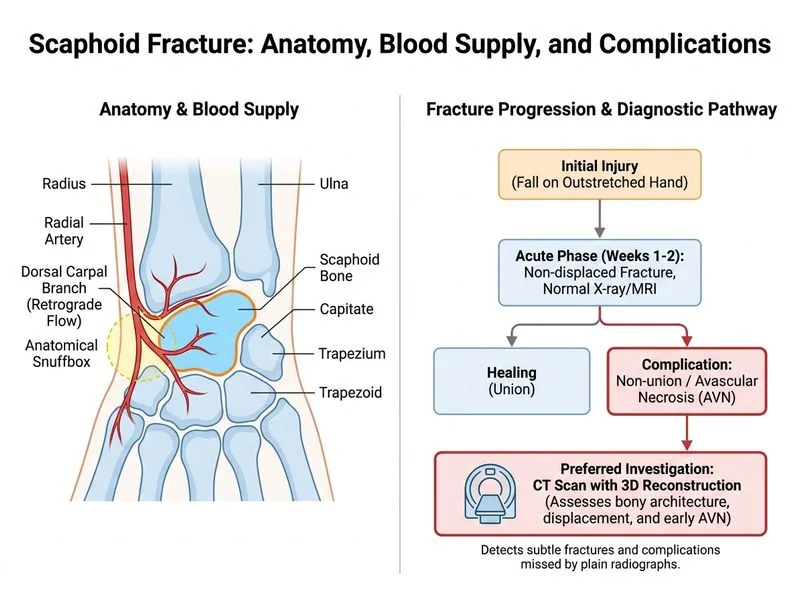
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.