## Clinical Context At 8 weeks post-immobilization with persistent pain and no radiographic evidence of bridging callus, this patient has a **delayed union or impending nonunion**. The waist location carries the highest nonunion risk due to tenuous blood supply. Operative intervention is now indicated. ## Nonunion Risk Stratification in Scaphoid Fractures | Risk Factor | Impact | Nonunion Rate | |---|---|---| | **Fracture location** | Proximal > waist > distal | Proximal: 10–15%; Waist: 5–10%; Distal: <5% | | **Displacement** | >2 mm increases risk | 2–3× higher | | **Associated injuries** | Ligament damage, comminution | Increased | | **Smoking, poor compliance** | Impaired healing | Increased | | **Time to diagnosis** | Delayed treatment | Increased | ## Management Algorithm for Scaphoid Nonunion/Delayed Union ```mermaid flowchart TD A[8+ weeks post-immobilization]:::outcome --> B{Bridging callus on X-ray?}:::decision B -->|Yes| C[Continue immobilization]:::action B -->|No| D[Obtain CT scan]:::action D --> E{Assess: Fracture pattern, vascularity, displacement}:::outcome E --> F{Nonunion confirmed?}:::decision F -->|Yes| G[Operative fixation: ORIF ± bone graft]:::action F -->|No| H[Continue immobilization, consider advanced imaging]:::action G --> I[Screw fixation ± vascularized bone graft if AVN]:::action ``` ## Key Point: **CT scan is the gold standard for assessing scaphoid nonunion.** It provides: (1) fracture geometry and displacement, (2) assessment of fracture surfaces (sclerosis, gap), (3) evaluation of proximal pole vascularity (indirectly), and (4) guidance for operative planning. ## High-Yield Facts: - **Delayed union:** No bridging callus at 8–12 weeks but fracture surfaces remain viable and in contact. - **Nonunion:** No bridging callus after 12–16 weeks; fracture surfaces may show sclerosis, gap, or cystic changes. - **Waist fractures** have the highest nonunion risk (5–10%) due to retrograde blood supply and limited collaterals. - **Operative fixation** (percutaneous screw fixation ± bone graft) is indicated for confirmed nonunion or impending nonunion with no bridging callus at 8+ weeks. - **Vascularized bone graft** is added if there is evidence of avascular necrosis of the proximal pole (seen on CT as sclerosis, cystic changes, or on MRI as signal changes). ## Clinical Pearl: **Persistent pain + no callus at 8 weeks = CT scan and prepare for surgery.** Waiting longer increases the risk of irreversible avascular necrosis and chronic wrist dysfunction. Early operative intervention has better outcomes than delayed intervention. ## Operative Options for Nonunion | Technique | Indication | Graft Type | |---|---|---| | **Percutaneous screw fixation alone** | Nonunion with viable fracture surfaces, no AVN | No graft | | **ORIF + cancellous bone graft** | Nonunion with gap or comminution | Autograft (iliac crest) | | **ORIF + vascularized bone graft** | Nonunion with AVN of proximal pole | Vascularized graft (1,2-ICSRA, medial femoral condyle) | | **Proximal row carpectomy (PRC)** | Salvage for chronic nonunion with AVN and arthritis | N/A | ## Tip: In the exam, when you see "8+ weeks post-immobilization + no callus + persistent pain," think **CT scan → operative fixation**. MRI is not the next step; CT is. Arthroscopy is not indicated for nonunion assessment. 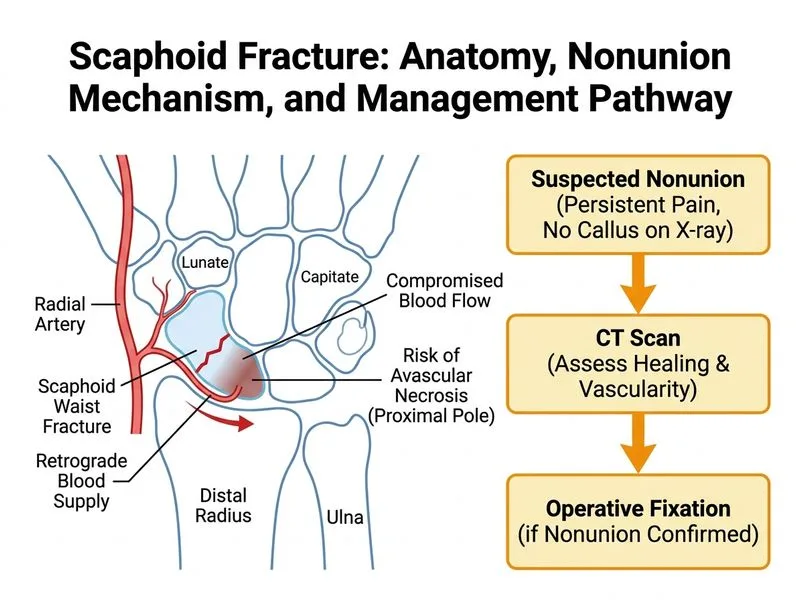
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.