## Scaphoid Waist vs. Proximal Pole Fracture: Critical Distinctions ### Vascular Anatomy — The Key Differentiator **Key Point:** The scaphoid's retrograde blood supply (distal to proximal) makes proximal pole fractures at highest risk for osteonecrosis (avascular necrosis), distinguishing them from waist fractures. ### Blood Supply Pattern The scaphoid receives its arterial supply via: 1. **Distal branches** (80% of blood supply) — enter through distal tubercle and waist 2. **Proximal branches** (20% of blood supply) — enter proximal pole directly Proximal pole fractures disrupt the fragile proximal blood supply, leaving the proximal fragment dependent on small intraosseous anastomoses. ### Comparison: Waist vs. Proximal Pole | Feature | Scaphoid Waist | Scaphoid Proximal Pole | |---------|---|---| | **Blood supply** | Relatively preserved (distal supply intact) | Compromised (proximal supply disrupted) | | **Nonunion rate** | 5–10% | 10–15% | | **Osteonecrosis rate** | <1% | 10–50% | | **Immobilization duration** | 8–12 weeks (uncomplicated) | 12–16 weeks minimum | | **Surgical indication** | Displaced (>2 mm), nonunion | Often primary ORIF | | **Prognosis** | Generally favorable | Guarded; osteonecrosis common | **High-Yield:** Proximal pole fractures are the most feared scaphoid fracture type due to osteonecrosis risk. This is the single most important clinical distinction that drives management decisions. **Clinical Pearl:** A proximal pole fracture with osteonecrosis may require scaphoid excision, four-corner fusion, or scapholunate advanced collapse (SLAC) wrist reconstruction — far more complex than waist fracture management. **Mnemonic:** **PROXIMAL = Poor blood supply, Risky osteonecrosis, Osteonecrosis (10–50%), Xrays show nonunion, Immobilization longer, Morbidity higher, Aggressive surgery needed, Longevity of wrist compromised** 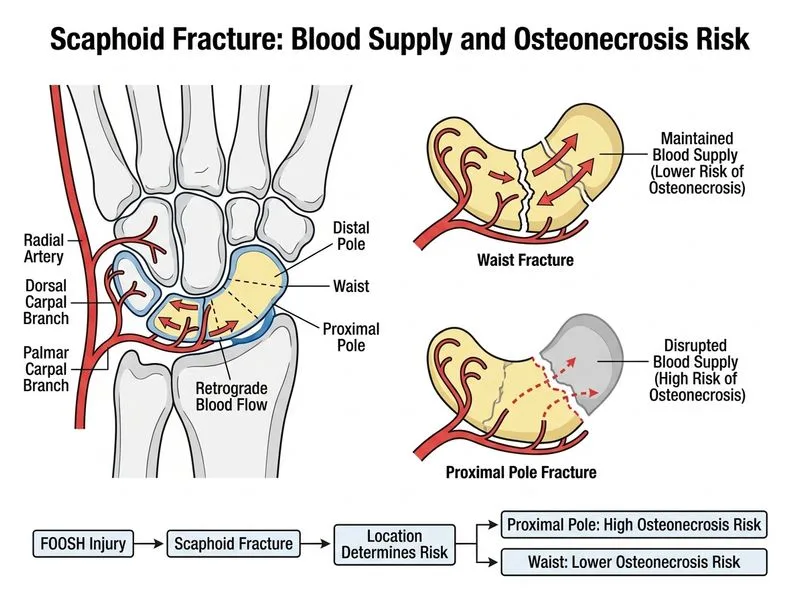
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.