## Peroneal Nerve Injury Post Hip Arthroplasty ### Clinical Recognition The patient has a **common peroneal nerve (CPN) injury**, evidenced by: - Foot drop (loss of ankle dorsiflexion) - Loss of sensation over dorsum of foot and lateral leg - **Preserved hip extension and knee flexion** (tibial nerve intact) The common peroneal nerve is the **most commonly injured nerve during hip arthroplasty**, accounting for ~60% of iatrogenic lower limb nerve injuries in this setting. ### Mechanism of Injury in Hip Arthroplasty **Key Point:** The common peroneal nerve is vulnerable because it: - Branches from the sciatic nerve at the proximal thigh - Winds around the fibular neck (superficial location) - Can be stretched by hip flexion/adduction during retraction - May be compressed by hematoma, swelling, or tight closure ### Why Conservative Management First? **High-Yield:** The vast majority of postoperative CPN injuries after total hip arthroplasty are **neurapraxia** — a physiological conduction block without axonal disruption — caused by traction, positioning, or mild compression. These injuries have an excellent prognosis for spontaneous recovery over 3–6 months. | Presentation | Likely Cause | Next Step | |---|---|---| | **Immediate (intraop), complete loss** | Direct trauma, transection | Urgent exploration | | **Delayed (24–72 hrs), partial/complete** | Neurapraxia, mild hematoma | **Observation + AFO + serial exam** | | **Progressive worsening >48 hrs** | Expanding hematoma | MRI + surgical consideration | | **No recovery at 3–6 weeks** | Axonotmesis/neurotmesis | EMG + neurosurgery consult | This patient has **delayed onset (postop day 2)** with a stable, non-progressive deficit — the classic presentation of compressive neurapraxia. There is no indication of an expanding hematoma (which would present with worsening deficits, increasing pain, or wound swelling). ### Management Algorithm **Step 1:** Assess for red flags requiring urgent intervention: - Rapidly progressive neurological deficit → suggests expanding hematoma → MRI + surgical evacuation - Intraoperative complete nerve transection → immediate exploration **Step 2:** In the absence of red flags (as in this patient): - Apply **ankle-foot orthosis (AFO)** to prevent equinus contracture and facilitate ambulation - **Serial clinical examination** at 2-week intervals to monitor for recovery or progression - EMG/NCS at 3–6 weeks if no improvement (to characterize injury severity) - Physiotherapy and foot drop management **Clinical Pearl:** Immediate return to OR (Option A) is not indicated without evidence of a surgically correctable lesion (e.g., confirmed hematoma on imaging). MRI (Option C) is reserved for cases with progressive deficits or failure to improve, not as the first step in a stable postoperative neurapraxia. High-dose IV methylprednisolone (Option B) has no evidence base in acute compressive peripheral neuropathy and is not recommended in modern practice (per Campbell's Operative Orthopaedics and AAOS guidelines). **Mnemonic — CPN Injury Features (FOOT DROP):** - **F**oot drop (ankle dorsiflexion loss) - **O**ver dorsum sensation loss - **O**uter leg sensory loss - **T**ibial nerve spared (hip/knee function preserved) - **D**elayed presentation (post-op neurapraxia) - **R**ecovers spontaneously in most cases - **O**bservation + AFO is first-line - **P**eroneal nerve at fibular neck (vulnerable site) ### Why Not Immediate Surgery or MRI? - **Option A (Immediate OR):** No evidence of transection or expanding hematoma; unnecessary re-exploration increases morbidity - **Option B (IV methylprednisolone):** No RCT evidence supports steroids for acute compressive peripheral neuropathy post-arthroplasty; risk of wound complications, infection - **Option C (MRI + neurosurgery):** Appropriate if deficits are progressive or worsening, but not as the initial step in a stable, delayed-onset deficit **High-Yield (per Campbell's Operative Orthopaedics & Harrison's Principles):** Most CPN injuries after hip arthroplasty are neurapraxia with spontaneous recovery. Initial management is **observation with AFO and serial neurological examination**. Imaging and surgical consultation are escalated only if deficits worsen or fail to improve. 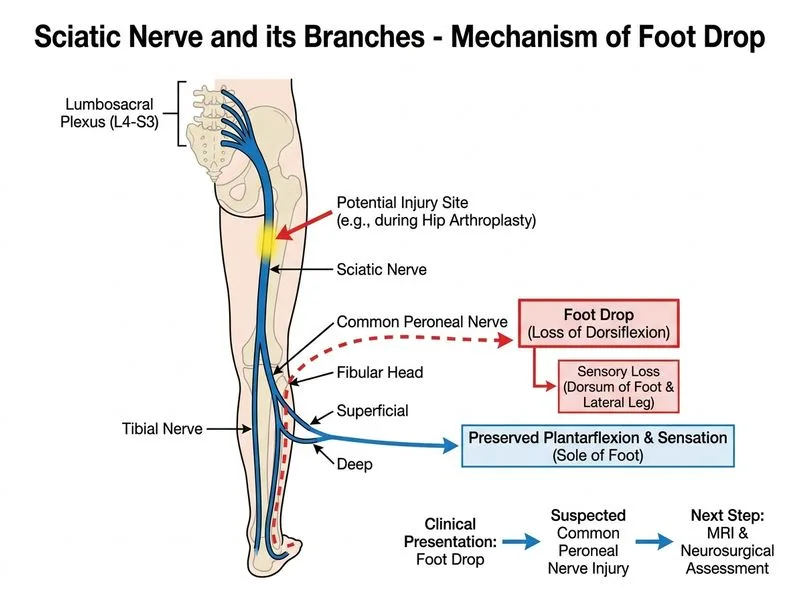
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.