## Diagnosis & Urgency **Key Point:** Septic arthritis is a surgical emergency. The clinical presentation—acute monoarticular arthritis with fever, traumatic inoculation, and synovial fluid analysis meeting septic criteria (WBC >50,000/μL, low glucose, positive Gram stain)—mandates immediate intervention. ## Synovial Fluid Interpretation The synovial fluid profile is diagnostic of bacterial septic arthritis: | Parameter | Value | Significance | |-----------|-------|---------------| | WBC | 85,000/μL | Markedly elevated (septic: typically >50,000) | | Neutrophils | 95% | Predominant in bacterial infection | | Protein | 6.2 g/dL | Elevated (septic: >5 g/dL) | | Glucose | 18 mg/dL | Severely low; serum 110 → CSF/synovial ratio <0.25 | | Gram stain | Positive cocci | Presumptive *Staphylococcus aureus* | **High-Yield:** Gram stain positivity in synovial fluid is found in only 50–60% of culture-confirmed septic arthritis; when present, it strongly supports immediate surgical drainage. ## Management Algorithm ```mermaid flowchart TD A[Suspected septic arthritis]:::outcome --> B{Synovial fluid analysis}:::decision B -->|WBC >50k, low glucose,<br/>positive Gram stain| C[Confirmed septic arthritis]:::urgent C --> D[Start IV antibiotics<br/>immediately]:::action D --> E[Urgent surgical drainage<br/>arthroscopy/arthrotomy]:::action E --> F[Send culture & sensitivity]:::action F --> G[Adjust antibiotics at 48-72h<br/>based on culture]:::action ``` ## Antibiotic Choice **Key Point:** Empiric coverage must target the most common pathogen (*Staphylococcus aureus*) and account for Gram stain findings. - **Cefazolin** (1–2 g IV Q8H): First-line for Gram-positive cocci; excellent joint penetration - **Gentamicin** (1.5 mg/kg IV Q8H): Added for synergy and broader Gram-negative coverage in traumatic wounds - Vancomycin is reserved for MRSA risk or β-lactam allergy **Clinical Pearl:** In India, where open trauma and environmental contamination are common, gram-negative organisms (*E. coli*, *Pseudomonas*) and anaerobes may be co-pathogens; gentamicin addition is justified. ## Why Urgent Drainage? 1. **Bacterial proliferation:** Septic joints can develop irreversible cartilage damage within 24–48 hours 2. **Pus accumulation:** Increased intra-articular pressure compromises synovial blood flow and antibiotic delivery 3. **Diagnostic yield:** Culture from drained fluid confirms organism and guides antibiotic de-escalation **High-Yield:** Arthroscopic drainage is preferred over needle aspiration alone because it allows: - Complete evacuation of pus and debris - Visualization of cartilage damage - Irrigation and lavage - Lower recurrence rates ## Timing **Warning:** Delays in drainage >48 hours are associated with worse functional outcomes and higher rates of permanent joint damage. This patient has already waited 5 days since inoculation; surgery must not be delayed for further investigations. 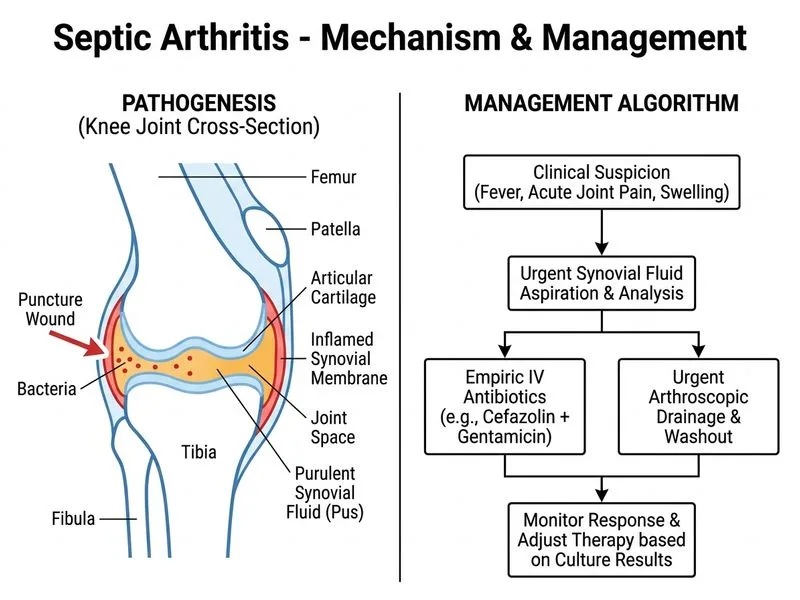
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.