## Diagnosis and Clinical Reasoning **Key Point:** This is acute bacterial septic arthritis with Staphylococcus aureus (Gram-positive cocci in clusters) in an IVDU, presenting with classic triad of fever, joint effusion, and elevated synovial WBC (>50,000/μL with PMN predominance). ### Synovial Fluid Analysis Interpretation | Parameter | Value | Interpretation | |-----------|-------|----------------| | WBC | 68,000/μL | Highly suggestive of septic arthritis (>50,000/μL) | | PMN % | 92% | Bacterial infection (>90% PMN is hallmark) | | Glucose | 18 mg/dL (serum 120) | Synovial:serum ratio <0.5 = bacterial | | Protein | 5.2 g/dL | Elevated; consistent with infection | | Gram stain | Gram+ cocci clusters | S. aureus (IVDU risk factor) | **High-Yield:** Septic arthritis is a **surgical emergency**. Delay in drainage >7 days increases risk of permanent joint damage, cartilage erosion, and functional loss. ### Management Algorithm ```mermaid flowchart TD A[Acute monoarthritis + fever + synovial WBC >50k]:::outcome --> B{Septic arthritis?}:::decision B -->|Yes| C[Blood culture + start empiric IV antibiotics]:::action C --> D[Vancomycin + 3rd gen cephalosporin]:::action D --> E[Urgent arthroscopic/open washout]:::urgent E --> F[Repeat aspiration if no improvement in 48h]:::action F --> G[Culture-directed therapy after 48-72h]:::action ``` ### Antibiotic Choice Rationale **Key Point:** Empiric coverage must include methicillin-resistant S. aureus (MRSA) in IVDU populations. 1. **Vancomycin 15–20 mg/kg IV 8-hourly** (or 12-hourly if renal function normal) - Covers MRSA, streptococci, and Gram-positive organisms - Achieves therapeutic synovial fluid levels 2. **Ceftriaxone 2 g IV 12-hourly** (or cefotaxime 2 g 6-hourly) - Covers Gram-negative bacilli and streptococci - Good synovial penetration - Alternative: fluoroquinolone if β-lactam allergy **Clinical Pearl:** Once culture and sensitivities return (typically 48–72 hours), narrow to organism-specific therapy (e.g., oxacillin or nafcillin if MSSA; continue vancomycin if MRSA). ### Surgical Drainage Indications **High-Yield:** Arthroscopic washout is indicated in ALL cases of acute septic arthritis except: - Hip joint in infants <3 months (percutaneous needle aspiration may suffice, but most require drainage) - Some small joints with minimal effusion (rare) **Urgent surgical drainage is mandatory because:** - Purulent synovial fluid is cytotoxic to cartilage - Enzymatic degradation of proteoglycans begins within hours - Irreversible cartilage loss occurs within 7 days if untreated ### Follow-up and Monitoring - Repeat joint aspiration at 48 hours if fever/pain persist or WBC not declining - Synovial fluid sterilization typically occurs within 24–48 hours of appropriate antibiotics + drainage - Duration of IV antibiotics: 2–4 weeks depending on organism and clinical response - Transition to oral antibiotics only after clinical improvement and negative repeat cultures **Warning:** Do NOT rely on needle aspiration alone without surgical drainage in acute septic arthritis — mortality and morbidity increase significantly. **Mnemonic:** **SAFE** approach to septic arthritis: - **S**ynovial fluid analysis (WBC, glucose, culture, Gram stain) - **A**ntibiotics (empiric, then culture-directed) - **F**luid removal (arthroscopic washout urgently) - **E**valuation (repeat aspiration if no improvement in 48 h) 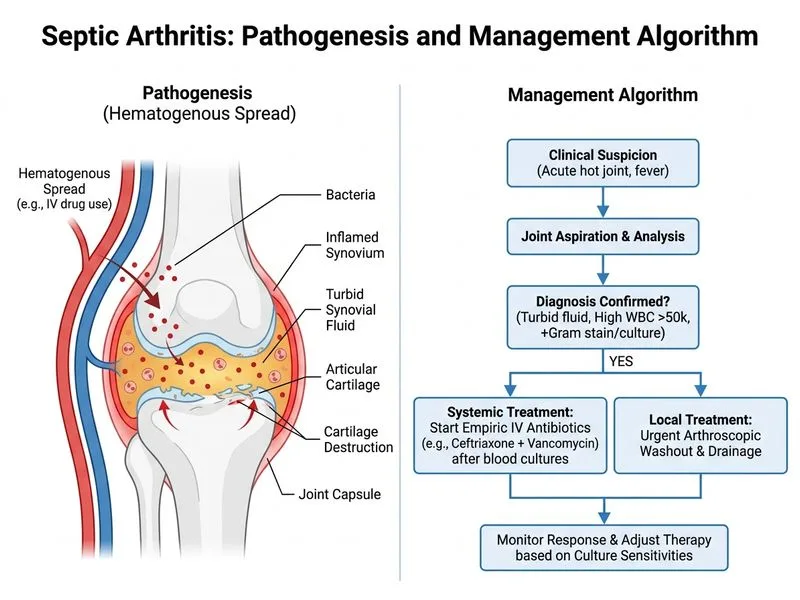
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.