## Diagnosis and Management of Neuroleptic Malignant Syndrome (NMS) ### Clinical Diagnosis: NMS This patient presents with the **classic tetrad of NMS**: 1. **Fever** (40.1°C) — hyperthermia 2. **Rigidity** — lead-pipe type (characteristic of NMS) 3. **Altered mental status** — confusion, decreased consciousness 4. **Autonomic instability** — hypertension, tachycardia ### Risk Factors Present - **Antipsychotic exposure:** Haloperidol (typical/first-generation antipsychotic) — high-risk agent - **Chronicity:** 8 years on same agent increases vulnerability - **Acute decompensation:** Withdrawal, reduced medication compliance, or environmental stress may precipitate ### Laboratory Findings: Evidence of Rhabdomyolysis **Key Point:** The elevated CK (3200 IU/L), acute kidney injury (creatinine 1.8), hyperkalemia (5.8), and dark urine (myoglobinuria) indicate **rhabdomyolysis with acute renal failure** — a life-threatening complication of NMS. ### Pathophysiology **Clinical Pearl:** NMS results from dopamine D~2~ receptor blockade in the hypothalamus and basal ganglia, leading to: - Loss of thermoregulation → hyperthermia - Increased muscle tone → rigidity and rhabdomyolysis - Sympathetic hyperactivity → autonomic instability ### Immediate Management Algorithm ```mermaid flowchart TD A[Suspected NMS]:::outcome --> B[Stop antipsychotic immediately]:::action B --> C[Supportive care]:::action C --> D[IV fluids for rhabdomyolysis]:::action D --> E[Dantrolene sodium 1 mg/kg IV]:::action E --> F{CK declining?<br/>Renal function stable?}:::decision F -->|Yes| G[Continue dantrolene 1 mg/kg Q4-6H]:::action F -->|No| H[Escalate fluids, monitor urine output]:::action I[Avoid re-exposure to antipsychotics] --> J[Consider atypical antipsychotic<br/>after full recovery]:::action ``` ### Why Dantrolene Sodium? **High-Yield:** Dantrolene works by: - Inhibiting calcium release from sarcoplasmic reticulum in skeletal muscle - Reducing muscle contractility and heat generation - **Dose:** 1 mg/kg IV bolus, then 1 mg/kg every 4–6 hours (max 10 mg/kg/day) - **Monitoring:** Continue until signs of NMS resolve or max dose reached ### Supportive Care Priorities 1. **Aggressive IV hydration** — maintain urine output >200 mL/hr to prevent myoglobin precipitation in renal tubules 2. **Urinary alkalinization** — sodium bicarbonate to raise urine pH >6.5 (myoglobin is more soluble in alkaline urine) 3. **Electrolyte monitoring** — hyperkalemia (5.8 here) requires urgent management; consider calcium gluconate, insulin + glucose, or dialysis if severe 4. **Cooling measures** — ice packs, cooling blankets 5. **Monitoring:** Serial CK, creatinine, potassium, urine myoglobin ### Comparison: NMS vs. Serotonin Syndrome | Feature | NMS | Serotonin Syndrome | |---------|-----|--------------------| | **Trigger** | Antipsychotic (D~2~ blockade) | Serotonergic drugs (SSRI + MAOI, etc.) | | **Onset** | 24–72 hours | Hours to 24 hours | | **Rigidity type** | Lead-pipe | Hyperreflexia, clonus prominent | | **GI symptoms** | Rare | Common (diarrhea) | | **CK elevation** | Marked (often >1000) | Mild to moderate | | **Treatment** | Dantrolene, bromocriptine | Cyproheptadine, benzodiazepines | ### Why NOT the Other Options? **Option A (Continue haloperidol + dantrolene):** Continuing the offending agent is contraindicated; it perpetuates dopamine blockade and prevents recovery. **Option C (Switch to second-generation antipsychotic):** Switching antipsychotics during acute NMS is dangerous — cross-sensitivity can occur, and the patient is already in rhabdomyolysis. Wait for full recovery (days to weeks) before reintroduction. **Option D (Bromocriptine + continue haloperidol):** While bromocriptine (dopamine agonist) is an alternative agent for NMS, it is **secondary** to dantrolene in acute management. Continuing haloperidol is contraindicated. ### Prognosis and Recovery - Mortality: 5–20% (higher with rhabdomyolysis and AKI) - Recovery: 24–72 hours after stopping antipsychotic; full neurological recovery may take weeks - **Re-exposure:** Avoid the same antipsychotic; if antipsychotic is necessary, use a low-potency typical or atypical agent after full recovery [cite:Harrison 21e Ch 470; Kaplan & Sadock's Synopsis of Psychiatry 12e Ch 28] 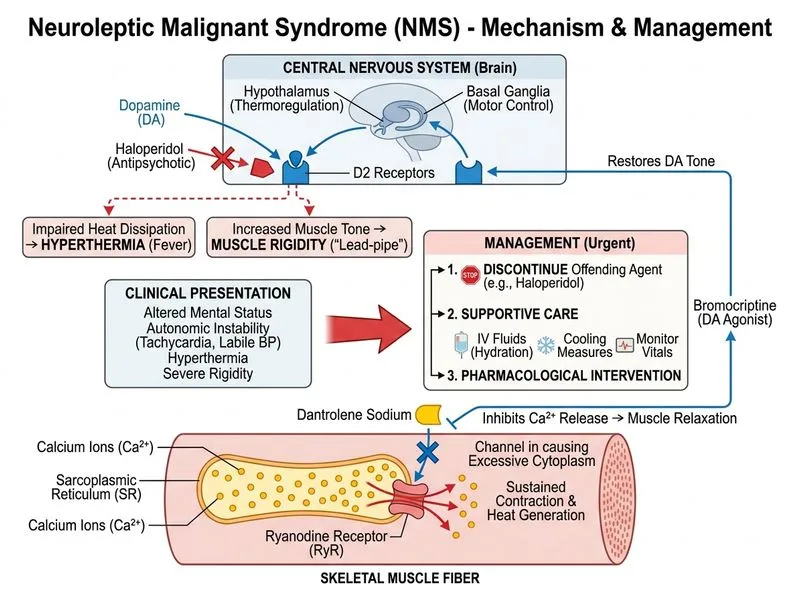
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.