## Clinical Diagnosis: Serotonin Syndrome ### Key Diagnostic Features **Key Point:** Serotonin syndrome is a potentially life-threatening condition caused by excessive serotonergic activity in the central nervous system, typically resulting from drug interactions or overdose. This patient presents with the classic triad of serotonin syndrome: 1. **Neuromuscular hyperactivity** — tremor, hyperreflexia, agitation 2. **Autonomic instability** — fever (39.2°C), hypertension, tachycardia 3. **Altered mental status** — agitation ### Mechanism of Toxicity The patient was on sertraline (SSRI) for 3 weeks when phenelzine (MAOI) was added. This is a direct serotonergic drug interaction: - SSRIs block reuptake of serotonin from the synapse - MAOIs block degradation of serotonin via monoamine oxidase - Combined effect → massive accumulation of serotonin → overstimulation of 5-HT receptors ### Hunter Criteria for Serotonin Syndrome **High-Yield:** The Hunter Criteria are the gold standard for diagnosis. This patient meets multiple criteria: - Spontaneous clonus (hyperreflexia, tremor) - Inducible clonus (hyperreflexia) - Ocular clonus (likely present) - Agitation + fever - Recent addition of serotonergic agent ### Differential Features vs. NMS | Feature | Serotonin Syndrome | NMS | | --- | --- | --- | | **Onset** | Minutes to hours | 24–72 hours | | **Trigger** | Serotonergic drugs (SSRI + MAOI, SSRI + tramadol, etc.) | Antipsychotics (typical > atypical) | | **Clonus** | **Present** (spontaneous, inducible, ocular) | **Absent** | | **Reflexes** | **Hyperactive** | Normal or increased | | **Rigidity** | Mild or absent | **Lead-pipe or cogwheel** | | **CK elevation** | Mild to moderate (usually < 1000) | Marked (often > 1000) | | **Progression** | Rapid, within hours | Gradual, over days | | **Treatment** | Serotonergic agent withdrawal, benzodiazepines, cyproheptadine | Antipsychotic withdrawal, supportive care, dantrolene | ### Clinical Pearl **Clinical Pearl:** The **rapid onset (6 hours)** after adding phenelzine to sertraline is pathognomonic for serotonin syndrome. NMS develops over 24–72 hours and is associated with antipsychotics, not SSRIs + MAOIs. ### Management 1. **Immediate:** Discontinue all serotonergic agents 2. **Supportive care:** IV fluids, cooling measures, benzodiazepines for agitation 3. **Cyproheptadine:** 12 mg loading dose, then 2 mg every 2 hours (competitive 5-HT antagonist) — specific for serotonin syndrome 4. **Monitor:** CK, electrolytes, renal function for rhabdomyolysis ### Mnemonic: SEROTONIN SYNDROME Risk Factors **Mnemonic:** **S.S.R.I. + M.A.O.I. = DANGER** - SSRIs (sertraline, fluoxetine, paroxetine) - Serotonin-norepinephrine reuptake inhibitors (SNRIs: venlafaxine, duloxetine) - Tramadol, meperidine, dextromethorphan (OTC cough suppressants) - St. John's Wort (herbal) - Linezolid (antibiotic) - Lithium - Monoamine oxidase inhibitors (phenelzine, tranylcypromine, isocarboxazid) [cite:Harrison 21e Ch 397] 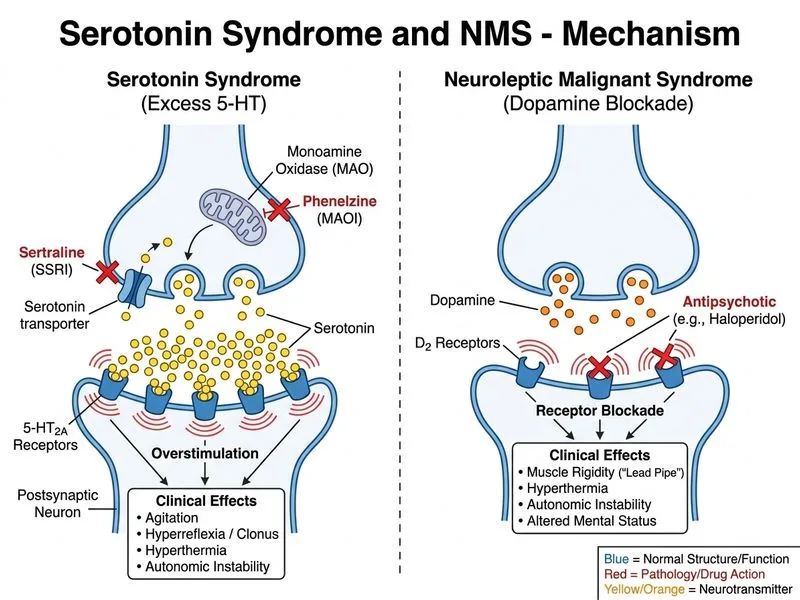
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.