## Diagnosis and Management: Neuroleptic Malignant Syndrome (NMS) ### Clinical Diagnosis **Key Point:** NMS is a rare but life-threatening idiosyncratic reaction to antipsychotics (especially typical antipsychotics like haloperidol) characterized by the tetrad of fever, rigidity, altered mental status, and autonomic instability. This patient meets all diagnostic criteria for NMS: 1. **Antipsychotic exposure** — haloperidol 10 mg daily for 2 months 2. **Fever** — 38.8°C 3. **Muscle rigidity** — severe, described as lead-pipe type 4. **Altered consciousness** — altered mental status 5. **Autonomic instability** — hypertension, tachycardia, diaphoresis 6. **Elevated CK** — 4200 IU/L (markedly elevated) 7. **Myoglobinuria** — positive urine myoglobin ### Pathophysiology NMS results from dopamine antagonism in the hypothalamus and basal ganglia, leading to: - Loss of thermoregulation → hyperthermia - Increased muscle tone via basal ganglia dysfunction → rigidity - Sympathetic hyperactivity → autonomic instability - Muscle breakdown → rhabdomyolysis with myoglobinuria and acute kidney injury ### Diagnostic Criteria Comparison: NMS vs. Serotonin Syndrome | Feature | NMS | Serotonin Syndrome | | --- | --- | --- | | **Onset** | 24–72 hours | Minutes to hours | | **Trigger** | Antipsychotics (haloperidol, risperidone, etc.) | Serotonergic drugs (SSRI + MAOI, tramadol, etc.) | | **Rigidity** | **Lead-pipe or cogwheel** (prominent) | Mild or absent | | **Clonus** | **Absent** | **Present** (spontaneous, inducible, ocular) | | **Reflexes** | Normal or brisk | **Hyperactive** | | **CK elevation** | Often **> 1000 IU/L** | Usually < 1000 IU/L | | **Myoglobinuria** | **Common** | Rare | | **GI symptoms** | Rare | **Common** (diarrhea) | ### Immediate Management Algorithm ```mermaid flowchart TD A[Suspected NMS]:::outcome --> B[Discontinue antipsychotic immediately]:::action B --> C[Supportive care: IV fluids, cooling]:::action C --> D{Severe rhabdomyolysis<br/>or CK > 3000?}:::decision D -->|Yes| E[Add dantrolene sodium]:::action D -->|No| F[Monitor CK, urine output, renal function]:::action E --> G[Dantrolene 1 mg/kg IV q4-6h<br/>up to 10 mg/kg/day]:::action G --> H[Benzodiazepines for agitation]:::action F --> I[Benzodiazepines for agitation]:::action H --> J[Monitor for complications:<br/>AKI, DIC, aspiration]:::action I --> J ``` ### Immediate Management Steps **High-Yield:** The cornerstone of NMS management is **immediate discontinuation of the antipsychotic** — this is non-negotiable. 1. **Discontinue haloperidol immediately** — continuation worsens outcomes 2. **Aggressive supportive care:** - IV fluids (0.9% saline, 200–300 mL/hr) to maintain urine output > 200 mL/hr - Active cooling measures (ice packs, cooling blankets, cold IV saline) - Oxygen supplementation if needed 3. **Dantrolene sodium** (indicated here due to CK 4200 and myoglobinuria): - Loading dose: 1 mg/kg IV push, repeat every 5–10 minutes up to 10 mg/kg/day - Mechanism: Reduces muscle rigidity by blocking calcium release from sarcoplasmic reticulum - Efficacy: Reduces mortality from ~11% to ~5% when used early 4. **Benzodiazepines** (lorazepam 2–4 mg IV q4–6h) for agitation and muscle relaxation 5. **Monitoring:** - Serial CK (peak at 24–72 hours) - Urine myoglobin - Serum creatinine and electrolytes - Coagulation studies (risk of DIC) - ECG (hyperkalemia risk) ### Clinical Pearl **Clinical Pearl:** The **3-day timeline and lead-pipe rigidity** are classic for NMS (not serotonin syndrome, which is acute). The **markedly elevated CK (4200) with myoglobinuria** indicates severe rhabdomyolysis and is an indication for dantrolene. Continuing the antipsychotic or switching to another antipsychotic immediately is dangerous. ### Why NOT the Other Options **Warning:** Continuing haloperidol or switching to another antipsychotic (clozapine) without a washout period risks perpetuating or worsening NMS. Cyproheptadine is used for serotonin syndrome, not NMS. ### Recovery and Re-challenge - Most patients recover within 24–72 hours of antipsychotic discontinuation - Antipsychotics can be cautiously re-introduced after 2–4 weeks (if necessary), but atypical agents (e.g., aripiprazole) are preferred - Clozapine has the lowest risk of NMS recurrence but requires careful monitoring [cite:Harrison 21e Ch 397; Sadock's Comprehensive Textbook of Psychiatry 11e Ch 29] 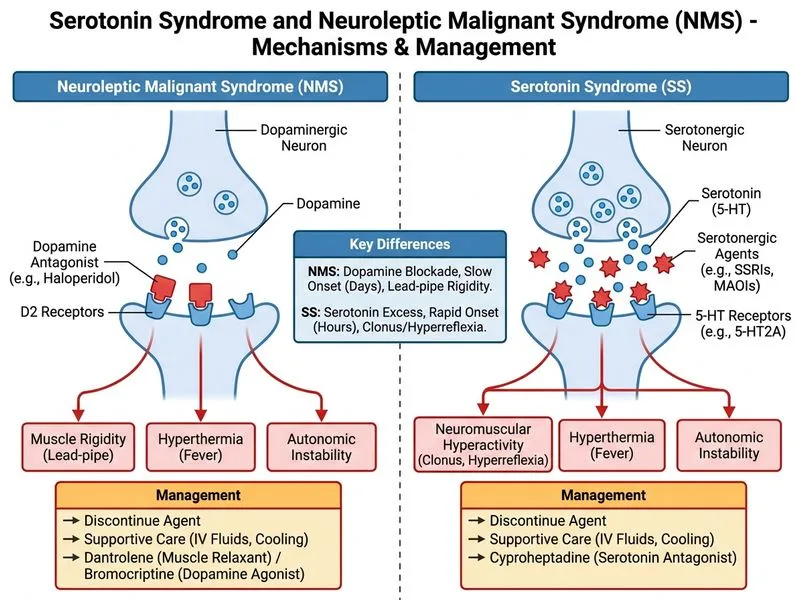
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.