## Diagnosis: Serotonin Syndrome ### Clinical Presentation This patient presents with the classic triad of serotonin syndrome: 1. **Neuromuscular signs**: tremor, hyperreflexia, clonus, muscle rigidity 2. **Autonomic instability**: fever (39.2°C), tachycardia (118/min), hypertension (156/92 mmHg) 3. **Altered mental status**: agitation ### Key Diagnostic Features **High-Yield:** Serotonin syndrome occurs when two or more serotonergic agents are combined without adequate washout. In this case: - **Sertraline** (SSRI) — ongoing - **Phenelzine** (MAOI) — started without 2-week washout of sertraline This is a **high-risk drug combination** because MAOIs and SSRIs both increase synaptic serotonin, creating a dangerous additive effect. ### Hunter Criteria for Serotonin Syndrome Presence of serotonergic agent + one of the following: - Spontaneous clonus - Inducible clonus + agitation or diaphoresis - Ocular clonus + agitation or diaphoresis - Tremor + hyperreflexia - Hypertonia + temperature >38.5°C + ocular clonus or inducible clonus This patient meets multiple criteria (clonus, hyperreflexia, tremor, fever, agitation, mydriasis). ### Severity Grading | Feature | Mild | Moderate | Severe | |---------|------|----------|--------| | Clonus | Spontaneous | Inducible | Sustained | | Rigidity | Mild | Moderate | Severe | | Fever | <38.5°C | 38.5–40°C | >40°C | | Renal involvement | No | Mild elevation | Rhabdomyolysis (Cr 1.8) | | Outcome | Self-limited | May require ICU | Life-threatening | This patient has **moderate-to-severe** serotonin syndrome with evidence of rhabdomyolysis (elevated creatinine). ### Management 1. **Immediate**: Stop all serotonergic agents 2. **Supportive care**: IV fluids, cooling measures, benzodiazepines for agitation 3. **Severe cases**: Cyproheptadine (serotonin antagonist) 12 mg loading, then 2 mg every 2 hours 4. **Monitor**: CK, myoglobin, urine output (rhabdomyolysis risk) **Key Point:** Serotonin syndrome is a medical emergency but is reversible if recognized early and offending agents are discontinued. NMS (neuroleptic malignant syndrome) requires antipsychotic exposure, which this patient does not have. **Clinical Pearl:** The **washout period** between SSRIs and MAOIs is critical: - SSRI to MAOI: 2 weeks (5 weeks for fluoxetine due to long half-life) - MAOI to SSRI: 2 weeks minimum - Failure to observe this is a common cause of serotonin syndrome in psychiatric practice. 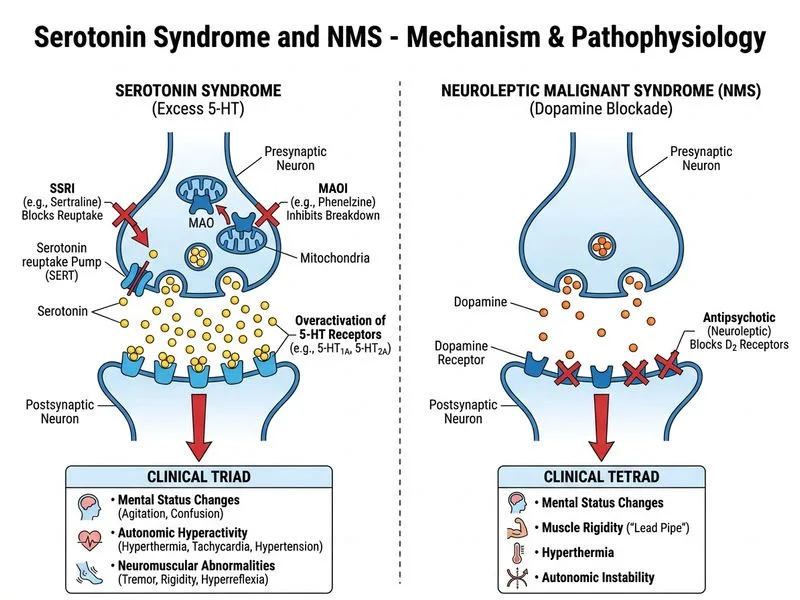
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.