## Diagnosis and Management: Neuroleptic Malignant Syndrome (NMS) ### Clinical Presentation of NMS This patient presents with the **classic tetrad of NMS**: 1. **Fever** (40.1°C) — high, often >39°C 2. **Muscle rigidity** ('lead pipe' rigidity) — uniform, sustained 3. **Altered mental status** — confusion, decreased consciousness 4. **Autonomic instability** — hypertension, tachycardia, tachypnea, diaphoresis ### Diagnostic Criteria (DSM-5) **High-Yield:** NMS is a clinical diagnosis. The presence of: - Exposure to dopamine antagonist (haloperidol) ✓ - Hyperthermia ✓ - Muscle rigidity ✓ - Altered mental status ✓ - Plus elevated CK and creatinine (rhabdomyolysis) ✓ ### Laboratory Findings | Parameter | Finding | Significance | |-----------|---------|---------------| | CK | 3200 IU/L | Elevated; indicates muscle breakdown | | Creatinine | 2.1 (↑ from 1.0) | Acute kidney injury from myoglobinuria | | Temperature | 40.1°C | Severe hyperthermia | | Rigidity pattern | Lead pipe | Uniform, sustained (vs. cogwheel in Parkinson's) | ### Immediate Management Algorithm ```mermaid flowchart TD A[Suspected NMS]:::outcome --> B[Stop dopamine antagonist immediately]:::action B --> C[Supportive care]:::action C --> D[IV fluids aggressive]:::action D --> E[Active cooling measures]:::action E --> F{Severe/Deteriorating?}:::decision F -->|Yes| G[Dantrolene 1 mg/kg IV q4-6h]:::action F -->|No| H[Monitor CK, Cr, urine output]:::action G --> H H --> I{Improvement?}:::decision I -->|Yes| J[Supportive care continues]:::action I -->|No| K[Consider ICU, dialysis]:::urgent ``` ### Why Discontinuation is Critical **Key Point:** The FIRST and most important step in NMS management is **immediate discontinuation of the dopamine antagonist**. Continuing or switching to another antipsychotic (option C) risks perpetuating or worsening the syndrome. **Clinical Pearl:** NMS can persist for 24–72 hours even after drug discontinuation due to the long half-lives of depot antipsychotics (like haloperidol). Supportive care is the cornerstone of treatment. ### Role of Dantrolene **High-Yield:** Dantrolene sodium is a skeletal muscle relaxant that acts on the sarcoplasmic reticulum to reduce intracellular calcium release. It is indicated in: - **Severe NMS** with rapidly rising CK, severe hyperthermia, or organ dysfunction - **Malignant hyperthermia** (anesthetic emergency) Dantrolene is **adjunctive**, not primary therapy. It does NOT replace stopping the antipsychotic. ### Comparison: Serotonin Syndrome vs. NMS | Feature | Serotonin Syndrome | NMS | |---------|-------------------|-----| | **Trigger** | Serotonergic drugs (SSRI, MAOI, tramadol) | Dopamine antagonist (antipsychotic, metoclopramide) | | **Onset** | Hours to days | Days to weeks | | **Rigidity** | Variable; often hyperreflexia, clonus | Lead pipe; uniform | | **GI symptoms** | Diarrhea common | Rare | | **CK elevation** | Mild to moderate | Severe (often >1000) | | **Management** | Stop serotonergic agent; cyproheptadine optional | Stop dopamine antagonist; dantrolene in severe cases | | **Mortality** | <5% | 10–20% if untreated | ### Supportive Care Priorities 1. **Aggressive IV hydration**: 200–300 mL/hour to maintain urine output >200 mL/hour 2. **Active cooling**: Ice packs, cooling blanket, cold IV saline 3. **Monitor urine myoglobin**: Risk of acute tubular necrosis 4. **Benzodiazepines**: For agitation, NOT as primary treatment 5. **Avoid rechallenge**: Do not restart antipsychotic for at least 2 weeks; consider atypical agents with lower NMS risk (quetiapine, aripiprazole) **Warning:** Continuing haloperidol (option A) or switching to another antipsychotic (option C) during acute NMS is dangerous and can worsen outcomes. Dantrolene alone without stopping the antipsychotic (option D) is insufficient. 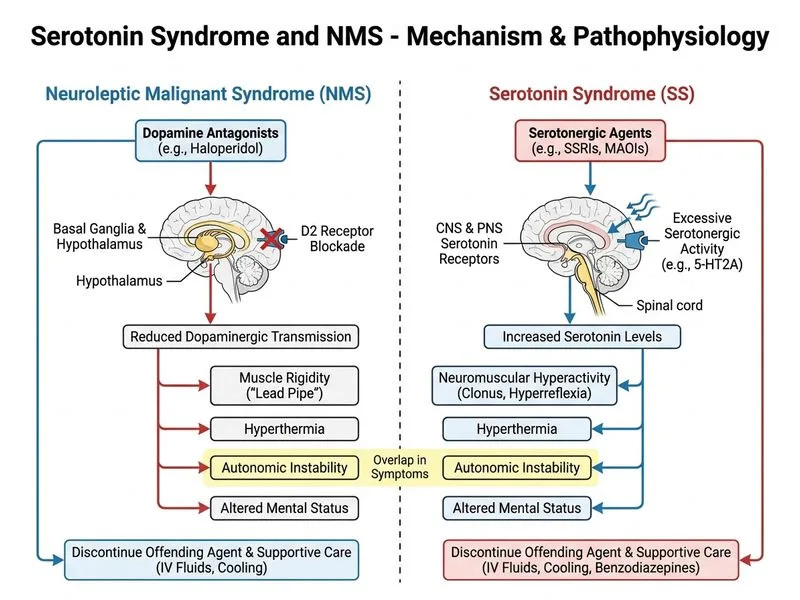
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.