## Lactate as a Marker of Tissue Hypoperfusion **Key Point:** Lactate > 4 mmol/L (36 mg/dL) is the critical threshold associated with significantly increased mortality and indicates severe tissue hypoperfusion requiring urgent intervention. ### Lactate Interpretation in Shock | Lactate Level | Clinical Significance | Mortality Risk | Action | |---|---|---|---| | < 2 mmol/L | Normal | Baseline | Routine monitoring | | 2–4 mmol/L | Mild hypoperfusion | Increased | Assess and optimize | | **> 4 mmol/L** | **Severe hypoperfusion** | **Significantly elevated** | **Aggressive resuscitation** | | > 8 mmol/L | Profound shock | Very high | ICU care, vasopressors | **High-Yield:** In septic shock and other shock states, lactate clearance (reduction of > 10% in 6 hours) is a better prognostic indicator than absolute lactate level. Persistent elevation despite resuscitation predicts poor outcome. **Clinical Pearl:** Lactate is produced when cells switch to anaerobic metabolism due to inadequate oxygen delivery. It reflects tissue-level hypoperfusion more accurately than blood pressure alone, making it a cornerstone of early goal-directed therapy (EGDT) protocols. **Mnemonic:** **"4 is the floor"** — Lactate > 4 mmol/L is the threshold where aggressive intervention becomes mandatory in shock management. ### Why Lactate Matters 1. Reflects anaerobic metabolism and tissue hypoperfusion 2. Independent predictor of mortality in shock 3. Guides resuscitation endpoints (lactate clearance) 4. More sensitive than blood pressure for detecting inadequate perfusion 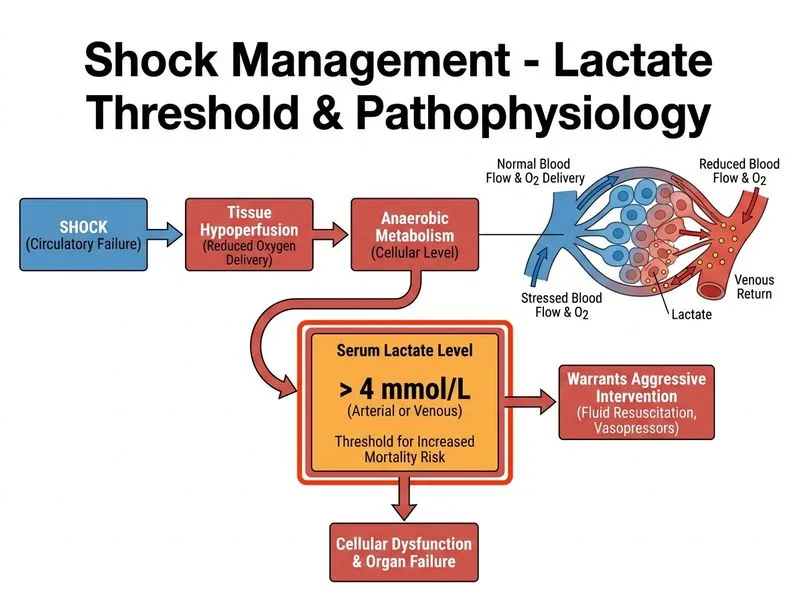
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.