## Clinical Diagnosis This patient presents with **septic shock** secondary to community-acquired pneumonia in a diabetic patient. The clinical triad of sepsis is evident: hypotension (88/54), tachycardia (118/min), and altered mental status (drowsy). Lactate elevation (4.2 mmol/L) and metabolic acidosis confirm tissue hypoperfusion. ## Sepsis Bundle and Early Goal-Directed Therapy (EGDT) **Key Point:** The Surviving Sepsis Campaign (SSC) 2021 guidelines mandate a **1-hour bundle** for septic shock: 1. Measure lactate and obtain blood cultures **before** antibiotics 2. Administer **30 mL/kg crystalloid bolus** for hypotension or lactate ≥4 mmol/L 3. Initiate **broad-spectrum antibiotics** within 1 hour 4. Apply vasopressors (noradrenaline first-line) if hypotension persists after fluid resuscitation 5. Re-measure lactate at 3 hours **High-Yield:** The sequence is **fluid first, then vasopressors**—not simultaneous or vasopressor-first. Crystalloid is the initial resuscitation fluid of choice in sepsis. ## Why Option 0 Is Correct This option encapsulates the complete 1-hour sepsis bundle: - **30 mL/kg bolus** (approximately 1.5–2 L for a 58 kg patient) addresses hypovolemia and restores perfusion pressure - **Broad-spectrum antibiotics** (e.g., piperacillin-tazobactam or ceftriaxone + fluoroquinolone for respiratory coverage) within 1 hour improve survival - **Central venous catheter (CVC)** allows measurement of central venous pressure (CVP) and ScvO₂ to guide further resuscitation and vasopressor titration **Clinical Pearl:** In septic shock, the warm peripheries and flushed skin indicate **vasodilatory shock** (loss of systemic vascular resistance). Fluid resuscitation restores intravascular volume; vasopressors restore vascular tone only *after* adequate preload. ## Pathophysiology of Septic Shock ```mermaid flowchart TD A[Gram-negative bacteremia]:::outcome --> B[Endotoxin LPS release]:::outcome B --> C[Toll-like receptor activation]:::outcome C --> D[TNF-α, IL-1, IL-6 surge]:::outcome D --> E[Nitric oxide & vasodilators]:::outcome E --> F[Systemic vasodilation<br/>Capillary leak]:::outcome F --> G[Hypovolemia + Hypotension]:::urgent G --> H[Tissue hypoperfusion<br/>Lactate rise]:::urgent H --> I{Fluid resuscitation?}:::decision I -->|Yes| J[Restore preload<br/>Improve CO]:::action I -->|No| K[Multi-organ failure]:::urgent J --> L{Persistent hypotension?}:::decision L -->|Yes| M[Add vasopressor<br/>Noradrenaline]:::action L -->|No| N[Continue monitoring<br/>Reassess lactate]:::action ``` ## Why Metabolic Acidosis Requires Antibiotics, Not Bicarbonate **Warning:** The patient's metabolic acidosis (pH 7.28, HCO₃⁻ 12) is **lactic acidosis** secondary to tissue hypoperfusion, not primary DKA. Sodium bicarbonate is **contraindicated** in lactic acidosis—it worsens intracellular acidosis and does not address the underlying cause. The acidosis will correct once perfusion is restored via fluid and vasopressor support. **Mnemonic:** **SAFE SEPSIS** = Source control, Antibiotics, Fluids, Evaluation (lactate), Supportive care, Early vasopressors, Procalcitonin/cultures, Source drainage, Infection source identification, Source removal. [cite:Surviving Sepsis Campaign 2021 Guidelines] 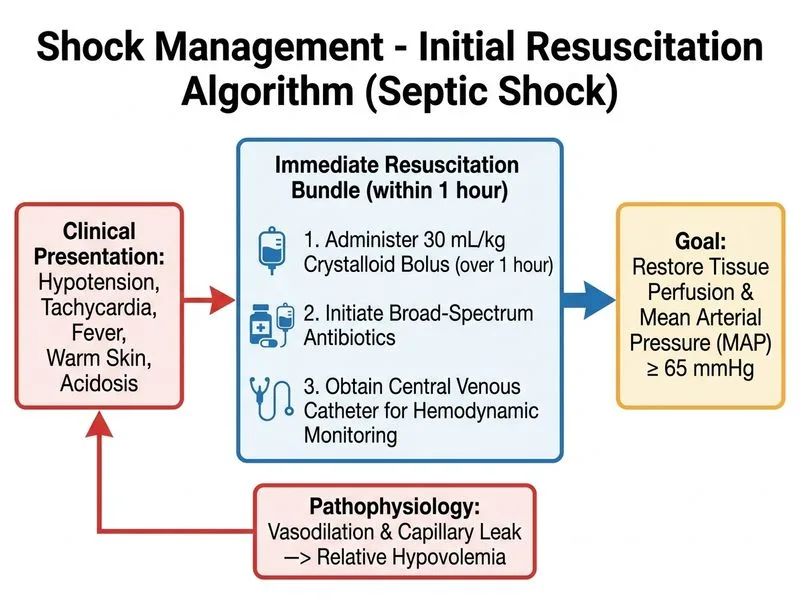
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.