## Clinical Diagnosis This patient has **distributive shock** (likely septic shock secondary to severe acute pancreatitis with organ dysfunction) that is **refractory to fluid resuscitation**. Despite adequate fluid bolus (CVP now 6 mmHg, indicating adequate preload), hypotension persists and lactate worsens, signaling ongoing tissue hypoperfusion and the need for vasopressor support. ## Vasopressor Selection in Septic/Distributive Shock **Key Point:** The Surviving Sepsis Campaign 2021 guidelines recommend **noradrenaline (norepinephrine) as first-line vasopressor** in septic shock. It combines: - **α₁-adrenergic effects** (vasoconstriction) → restores mean arterial pressure (MAP) - **β₁-adrenergic effects** (mild inotropic support) → maintains cardiac output **High-Yield:** Noradrenaline is superior to dopamine in septic shock because: 1. **Lower arrhythmia risk** compared to dopamine 2. **More predictable vasoconstriction** at therapeutic doses 3. **Reduced tachycardia** compared to dopamine 4. **Better splanchnic perfusion** preservation ## Vasopressor Comparison Table | Vasopressor | α-Effect | β₁-Effect | β₂-Effect | Mechanism | Role in Sepsis | Caution | |---|---|---|---|---|---|---| | **Noradrenaline** | +++ | ++ | 0 | α > β | **First-line** | Peripheral vasoconstriction | | Dopamine | Dose-dependent | +++ (mid-dose) | + | Dose-dependent | Second-line | Arrhythmias, tachycardia | | Dobutamine | 0 | +++ | ++ | Inotrope + vasodilator | **Avoid monotherapy** | Hypotension, tachycardia | | Epinephrine | +++ (high dose) | +++ | ++ (high dose) | Mixed | Refractory shock only | Severe tachycardia, arrhythmias | | Vasopressin | V₁ (direct vasoconstriction) | 0 | 0 | Non-catecholamine | Adjunct only | Limited role | ## Why Noradrenaline (Option 1) Is Correct 1. **SSC 2021 Guideline:** Noradrenaline is the **first-line vasopressor** for septic shock, targeting MAP ≥65 mmHg 2. **Dose:** 0.01–0.05 μg/kg/min IV (titrate upward every 5–10 minutes until target MAP achieved) 3. **Mechanism:** Balanced α and β₁ activity restores vascular tone while maintaining cardiac output 4. **Evidence:** Superior to dopamine in septic shock (SOAP II trial: lower 28-day mortality with noradrenaline) 5. **Administration:** Requires central line (peripheral infusion risks tissue necrosis) **Clinical Pearl:** The goal is MAP ≥65 mmHg, not systolic BP. In this patient, noradrenaline should be titrated to achieve MAP ≈70 mmHg while reassessing lactate clearance at 3 hours. Persistent lactate elevation despite adequate MAP suggests ongoing tissue hypoperfusion or multi-organ failure requiring escalation (addition of vasopressin or hydrocortisone). ## Vasopressor Escalation Algorithm ```mermaid flowchart TD A[Septic shock<br/>Fluid resuscitated]:::outcome --> B[Start noradrenaline<br/>0.01-0.05 μg/kg/min]:::action B --> C{MAP ≥ 65 mmHg?}:::decision C -->|Yes| D[Titrate to effect<br/>Reassess lactate]:::action C -->|No| E[Increase noradrenaline<br/>every 5-10 min]:::action E --> F{MAP goal achieved?}:::decision F -->|Yes| G[Continue noradrenaline<br/>Monitor ScvO₂]:::action F -->|No| H[Add second vasopressor<br/>Vasopressin or epinephrine]:::action G --> I{Lactate clearing?}:::decision I -->|Yes| J[Wean vasopressor<br/>as shock resolves]:::action I -->|No| K[Consider hydrocortisone<br/>if refractory]:::action ``` **Mnemonic:** **NAE** = **N**oradrenaline first, **A**dd vasopressin if refractory, **E**pinephrine for cardiogenic component. [cite:Surviving Sepsis Campaign 2021 Guidelines, Harrison 21e Ch 325] 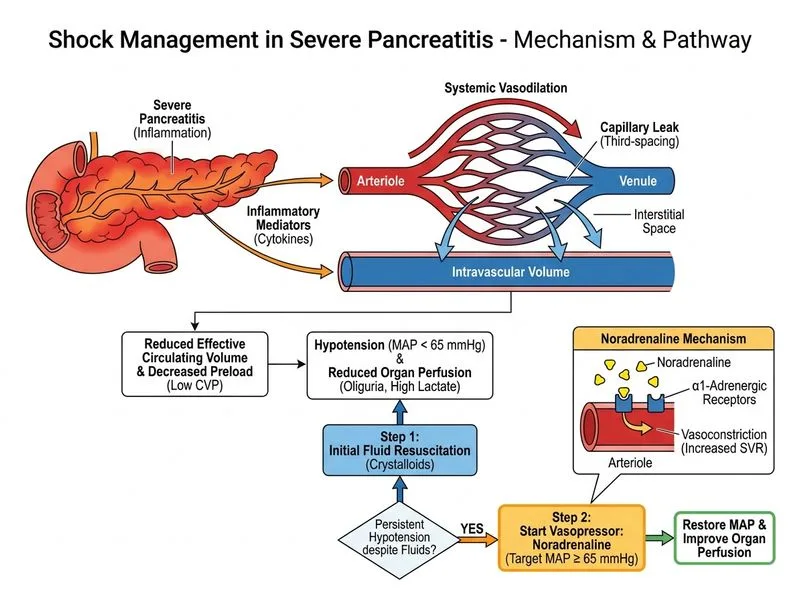
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.