## Septic Shock Management — Early Recognition and Resuscitation Bundle **Key Point:** The Surviving Sepsis Campaign guidelines (2021) mandate that broad-spectrum antibiotics be administered within 1 hour of recognition of sepsis or septic shock, regardless of source identification. This is a time-critical intervention. ### Clinical Presentation Analysis This patient meets criteria for septic shock: - Fever + hypotension requiring vasopressor support (or lactate ≥2 mmol/L) - Altered mental status (organ dysfunction) - Tachycardia and elevated lactate (4.2 mmol/L) indicating tissue hypoperfusion ### The 1-Hour Bundle (Sepsis Bundle) 1. **Lactate measurement** — ✓ already done 2. **Blood cultures** — ✓ already drawn 3. **Broad-spectrum antibiotics** — **MUST be given NOW** (within 60 minutes) 4. **IV fluid resuscitation** — concurrent with antibiotics 5. **Vasopressors** — only if hypotension persists after fluid resuscitation **High-Yield:** Antibiotic administration is the single most time-sensitive intervention in septic shock. Every hour of delay increases mortality by ~7–8%. ### Why Antibiotics First? - Empiric coverage (e.g., ceftriaxone + fluoroquinolone or piperacillin-tazobactam) must begin immediately - Source identification (CT, cultures) happens *in parallel*, not *before* antibiotics - Delaying antibiotics to obtain imaging is a major cause of preventable sepsis mortality **Clinical Pearl:** In septic shock, the adage is: **"Treat first, investigate second."** Imaging and source control procedures are arranged urgently *after* initial resuscitation begins, not before. ### Fluid and Vasopressor Sequencing - Initial crystalloid bolus: 30 mL/kg over first 3 hours (typically 1–2 L in adults) - Vasopressors (norepinephrine preferred) added if MAP remains <65 mmHg after fluids - This patient's BP (88/52) warrants both fluids AND likely vasopressors, but antibiotics must be concurrent [cite:Harrison 21e Ch 325] 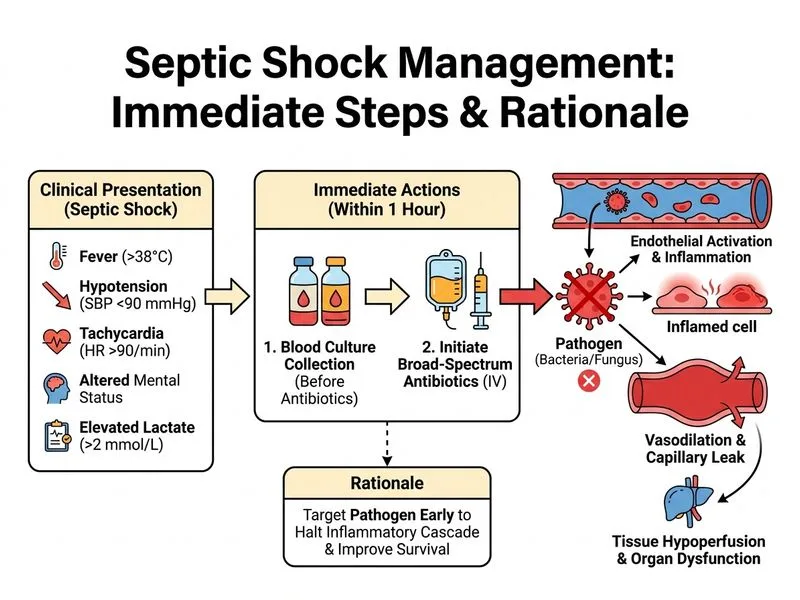
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.