## Cardiogenic Shock from Acute Mitral Regurgitation — Mechanical Complication of MI ### Clinical Recognition This patient has **cardiogenic shock** from a mechanical complication of acute MI: - **Acute mitral regurgitation** (holosystolic murmur at apex) - **Papillary muscle rupture** (confirmed on echo) - **Hypotension** (82/48 mmHg) + elevated JVP + clear lungs = **RV infarction pattern** or acute LV failure with pulmonary edema developing - **Time-critical surgical emergency** **Key Point:** Acute mitral regurgitation from papillary muscle rupture is a mechanical complication of MI that causes acute, severe cardiogenic shock. Medical management alone is futile; emergency surgical repair is the only definitive treatment. ### Why IABP is the Correct Immediate Step | Feature | Role in Papillary Muscle Rupture | |---------|-----------------------------------| | **IABP mechanism** | Reduces afterload (decreases regurgitant volume), increases diastolic BP (improves coronary perfusion) | | **Hemodynamic effect** | Improves forward cardiac output by reducing regurgitation fraction | | **Bridge to surgery** | Stabilizes patient during urgent surgical preparation and transport | | **Timing** | Inserted immediately in ICU/cath lab; surgery arranged in parallel | **High-Yield:** In acute mechanical complications of MI (papillary muscle rupture, VSD, free wall rupture), IABP is the **bridge to definitive surgical repair**. It is NOT a definitive treatment but buys time and stabilizes hemodynamics. ### Why Other Options Fail **Nitroprusside + repair alone:** - Nitroprusside reduces afterload but does NOT improve forward flow as effectively as IABP - Arranging repair without hemodynamic support risks cardiogenic arrest during transport - IABP must be initiated first to stabilize the patient **Furosemide + fluid optimization:** - Diuretics worsen cardiogenic shock by reducing preload further - This is a mechanical problem, not fluid overload; it requires surgical correction - Medical management alone has 0% survival in papillary muscle rupture **High-dose dobutamine:** - Inotropes increase myocardial oxygen demand and worsen ischemia - In the setting of acute MI, dobutamine increases arrhythmia risk - Does not address the underlying mechanical defect ### Management Algorithm ```mermaid flowchart TD A[Acute MI + Mechanical Complication]:::outcome --> B{Hemodynamically Stable?}:::decision B -->|Yes| C[Urgent surgery within 24-48 hrs]:::action B -->|No| D[Cardiogenic Shock]:::urgent D --> E[Insert IABP immediately]:::action E --> F[Arrange emergency surgical repair]:::action F --> G[Transport to OR]:::action G --> H[Surgical repair/replacement]:::action H --> I[Outcome]:::outcome ``` **Clinical Pearl:** The phrase "clear lung fields" with hypotension and elevated JVP suggests the regurgitant jet is directed posteriorly into the pulmonary veins, not causing pulmonary edema acutely. However, acute mitral regurgitation still causes rapid decompensation and shock. **Mnemonic:** **IABP for Mechanical Complications** = **I**ntra-Aortic **B**alloon **P**ump is the **bridge** to **P**erfusion and surgical **P**rocedure. [cite:Harrison 21e Ch 297; Braunwald's Heart Disease 12e Ch 41] 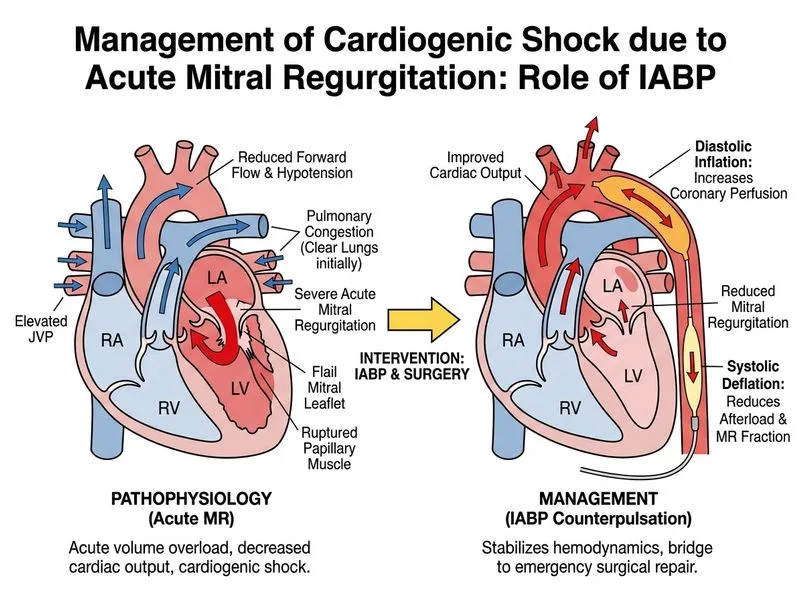
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.