## Differentiation of Shock Types: Cardiogenic vs. Distributive **Key Point:** Transthoracic echocardiography with assessment of left ventricular ejection fraction (LVEF) and regional wall motion abnormalities is the most appropriate non-invasive investigation to differentiate cardiogenic shock from distributive shock in acute MI. ### Clinical Context: Acute Anterior MI with Shock This patient presents with: - Acute chest pain + ST elevation (acute MI) - Hypotension + tachycardia (shock) - Bilateral crackles (pulmonary edema → left heart failure) - These features strongly suggest **cardiogenic shock** due to acute MI ### Why Transthoracic Echocardiography? **High-Yield:** Echocardiography provides: 1. **LVEF measurement** → directly assesses systolic function - LVEF <40% in cardiogenic shock - LVEF normal in distributive shock (sepsis, anaphylaxis, pancreatitis) 2. **Regional wall motion abnormalities** → identifies infarcted myocardium - Anterior MI: anterior wall, septum, apex involvement - Confirms acute coronary event 3. **Diastolic dysfunction** → assesses filling pressures 4. **Mechanical complications** → rules out rupture, VSD, papillary muscle rupture 5. **Non-invasive, bedside, rapid** → no delay in resuscitation ### Shock Type Differentiation Table | Parameter | Cardiogenic Shock | Distributive Shock | |-----------|------------------|-------------------| | **LVEF** | Reduced (<40%) | Normal (>50%) | | **Wall motion** | Regional abnormalities (MI) | Global, normal contraction | | **Pulmonary edema** | Present (pulmonary crackles) | Absent initially | | **Skin** | Cold, clammy | Warm, flushed | | **CVP/PCWP** | Elevated | Low to normal | | **Cardiac output** | Low | Low initially, then high (sepsis) | | **Cause** | MI, cardiomyopathy, arrhythmia | Sepsis, anaphylaxis, pancreatitis | **Clinical Pearl:** In cardiogenic shock from acute MI: - Pulmonary edema occurs because the failing left ventricle cannot eject blood → backup into pulmonary circulation - Bilateral crackles + hypotension + reduced LVEF = classic cardiogenic shock - In distributive shock (e.g., sepsis), pulmonary edema is absent initially because the problem is vasodilation and maldistribution, not pump failure ### Why Other Options Are Suboptimal **Pulmonary Artery Catheter (Option A):** - Invasive, requires central line placement → delays resuscitation - PCWP elevation is seen in both cardiogenic AND acute respiratory distress syndrome (ARDS) from sepsis - Does not directly visualize myocardial function or wall motion - Rarely used in modern practice for shock differentiation; echocardiography has largely replaced it **Serum Procalcitonin and Blood Cultures (Option B):** - Used to diagnose septic shock (distributive shock from infection) - In this case, the clinical presentation (acute MI with ST elevation, pulmonary edema, anterior wall involvement) is clearly cardiogenic, not septic - Procalcitonin elevation would be a red herring; it does not assess cardiac function - Blood cultures are appropriate for sepsis but not for acute MI **Chest X-ray and BNP (Option D):** - CXR shows pulmonary edema but does NOT differentiate cardiogenic from distributive shock (ARDS also shows infiltrates) - BNP is elevated in heart failure but also in sepsis, renal failure, and other conditions → not specific for cardiogenic shock - Neither test assesses LVEF or wall motion directly - BNP is useful for chronic heart failure diagnosis, not acute shock differentiation ### Echocardiography: The Gold Standard **Mnemonic:** ECHO = **E**jection fraction **C**larifies **H**eart function **O**utcome Echocardiography is: - **Rapid** (can be done at bedside in <5 minutes) - **Non-invasive** (no delay in resuscitation) - **Specific** (directly visualizes myocardial function and wall motion) - **Prognostic** (LVEF predicts mortality in cardiogenic shock) - **Therapeutic** (identifies mechanical complications requiring urgent intervention) 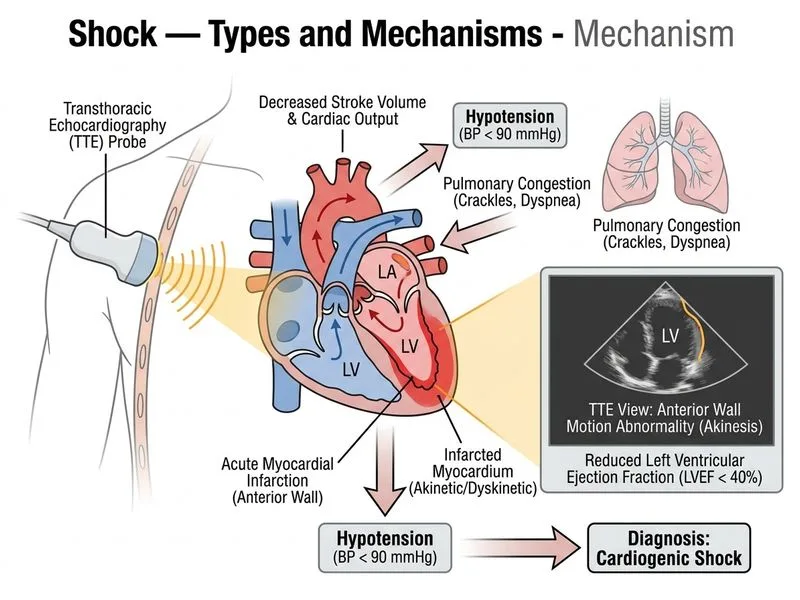
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.