## Clinical Scenario Analysis This patient presents with **cardiogenic shock** secondary to acute anterior MI with severe LV dysfunction. The clinical triad is present: - Hypotension (SBP <90 mmHg) - Evidence of hypoperfusion (altered mental status implied by presentation) - Pulmonary congestion (elevated JVP, bilateral crackles) ## Pathophysiology of Cardiogenic Shock **Key Point:** Cardiogenic shock occurs when cardiac output falls below the level needed to maintain tissue perfusion, despite adequate or elevated filling pressures. In acute MI, loss of >40% of LV mass typically precipitates shock. ## Management Algorithm for Cardiogenic Shock ```mermaid flowchart TD A[Acute MI + Hypotension + Pulmonary edema]:::outcome --> B{Cardiogenic shock?}:::decision B -->|Yes| C[Establish IV access, O2, monitoring]:::action C --> D[Inotropic support: Dobutamine or Milrinone]:::action D --> E[Urgent coronary angiography + PCI]:::action E --> F[Revascularization achieved]:::outcome B -->|No| G[Medical management alone]:::action ``` ## Rationale for Correct Answer **High-Yield:** In cardiogenic shock from acute MI, the immediate management triad is: 1. **Inotropic support** (dobutamine) to improve cardiac contractility and peripheral perfusion 2. **Urgent revascularization** (PCI) to restore coronary flow and salvage myocardium 3. **Hemodynamic monitoring** to guide therapy Dobutamine is preferred over dopamine in this setting because it provides: - Positive inotropic effect (β₁ receptors) - Peripheral vasodilation (β₂ receptors) — reduces afterload - Minimal tachycardia compared to dopamine Emergency angiography with PCI is the definitive therapy and should be arranged immediately, as revascularization within 12 hours of symptom onset significantly improves survival in cardiogenic shock. ## Why Fluid Bolus Is Contraindicated **Warning:** The presence of elevated JVP and bilateral crackles indicates **pulmonary edema** — the patient is NOT hypovolemic. Fluid administration would worsen pulmonary congestion and respiratory distress. This is a common trap: hypotension + shock does NOT always mean hypovolemia. ## Why Vasodilators Alone Are Inadequate Nitroprusside and high-dose furosemide reduce preload and afterload but do NOT address the fundamental problem: severely reduced cardiac contractility. Without inotropic support, further reduction in preload will cause worsening hypotension and organ hypoperfusion. 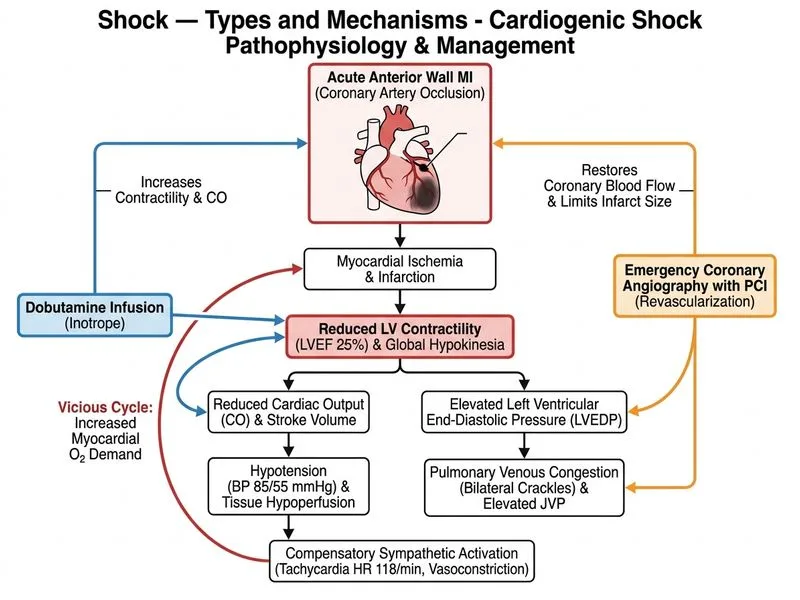
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.