## Pathophysiology of Osteomyelitis in Sickle Cell Disease ### Why Functional Asplenia? **Key Point:** Patients with sickle cell disease develop **functional asplenia** by age 5–6 years due to repeated splenic infarction from vaso-occlusion. This is the PRIMARY mechanism predisposing to encapsulated and atypical infections. ### Mechanism of Functional Asplenia 1. **Sickling in splenic microvasculature** → vaso-occlusion 2. **Repeated splenic infarction** → fibrosis and autoinfarction 3. **Loss of splenic function** → impaired: - **Opsonization** (coating of pathogens with IgG and complement) - **Complement-mediated killing** (especially alternative pathway) - **Clearance of unopsonized bacteria** - **Marginal zone B-cell function** (antibody production to polysaccharide antigens) ### Why *Salmonella* Specifically? **High-Yield:** *Salmonella* (non-typhi species) is the **classic pathogen of osteomyelitis in SCD**, occurring 50–100 times more frequently than in the general population. **Clinical Pearl:** While *Staphylococcus aureus* is the most common cause of osteomyelitis overall, *Salmonella* is the **most common in SCD**—a critical distinction for NEET PG. ### Comparison of Osteomyelitis Pathogens in SCD | Pathogen | Frequency in SCD | Reason | Clinical Feature | |----------|------------------|--------|------------------| | ***Salmonella* (non-typhi)** | Most common | Asplenia + gut translocation | Metaphyseal | | *Staphylococcus aureus* | Second most common | Still occurs; asplenia is not absolute | Metaphyseal/diaphyseal | | *Streptococcus pneumoniae* | Encapsulated; asplenia | Sepsis/meningitis more than osteomyelitis | Systemic | | *Haemophilus influenzae* | Encapsulated; asplenia | Rare post-vaccination | Systemic | ### Why Not the Other Options? **Increased bone marrow cellularity** does occur in SCD (extramedullary hematopoiesis), but it does not directly impair blood flow to bone or predispose to infection. It is a consequence of chronic hemolysis, not a cause of osteomyelitis. **Defective neutrophil chemotaxis** is not a feature of SCD. Neutrophil counts are often elevated due to chronic hemolysis and inflammation. The problem is not neutrophil function but rather the loss of splenic opsonization. **Chronic hypoxia-induced impaired wound healing** is not the mechanism. Bone is well-vascularized in SCD (paradoxically, due to chronic anemia-driven hyperemia), and the issue is immunologic, not vascular. ### Mnemonic: ASPLENIA in SCD **A** — Autoinfarction of spleen (repeated vaso-occlusion) **S** — Susceptibility to encapsulated organisms (*Streptococcus pneumoniae*, *Haemophilus*) **P** — Predisposition to *Salmonella* osteomyelitis **L** — Loss of opsonization and complement-mediated killing **E** — Encapsulated pathogens + atypical organisms (*Mycoplasma*, *Salmonella*) **N** — Neisseria meningitidis also increased risk **I** — Impaired IgG and complement responses **A** — Asplenic crisis (acute hemolytic episode) ### Clinical Management - **Prophylaxis:** Penicillin V (or amoxicillin) from infancy until age 5, then reassess - **Vaccination:** Pneumococcal, *Haemophilus influenzae* type b, meningococcal (before asplenia develops) - **Acute osteomyelitis:** Broad-spectrum antibiotics covering *Salmonella*, *Staph*, and atypical organisms **Warning:** Do not assume *Staph aureus* in SCD osteomyelitis—always include *Salmonella* coverage. [cite:Robbins 10e Ch 14; Harrison 21e Ch 104] 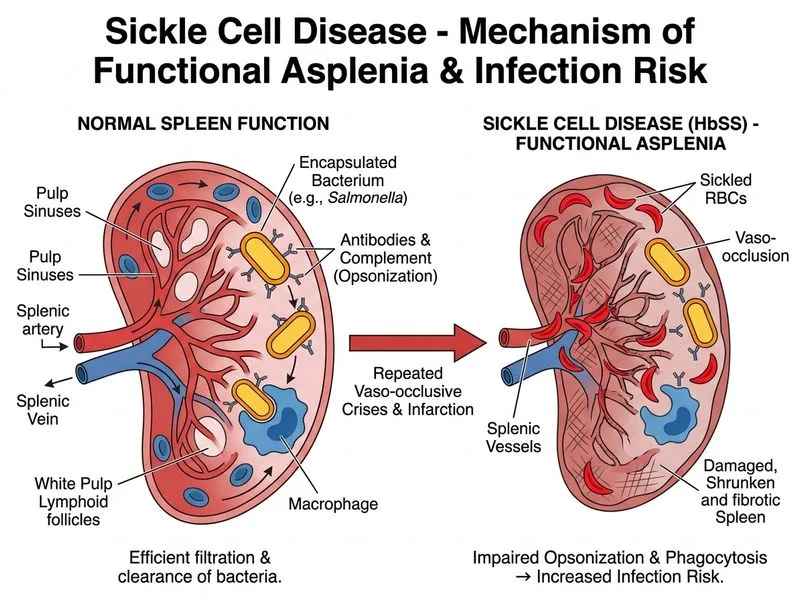
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.