## Clinical Diagnosis: Acute Chest Syndrome (ACS) ### Definition and Pathophysiology **Key Point:** Acute chest syndrome (ACS) is a vaso-occlusive crisis involving the lungs, characterized by acute chest pain, dyspnea, fever, and new pulmonary infiltrate(s) in a patient with sickle cell disease. **High-Yield:** ACS is caused by: 1. **Vaso-occlusion** in pulmonary microvasculature → infarction 2. **Fat embolism** from bone marrow necrosis 3. **In situ thrombosis** and inflammation 4. **Infection** (secondary, not primary cause) ### Clinical Presentation | Feature | Finding | Significance | |---------|---------|---------------| | Chest pain | Acute, severe | Pleuritic, from pulmonary infarction | | Dyspnea | Present | From hypoxemia and reduced lung compliance | | Fever | 39.2°C | Inflammatory response; can occur without infection | | Cough | Present | From airway irritation and inflammation | | Infiltrate | New on CXR | Pulmonary infarction, consolidation, or edema | | O₂ saturation | 88% (low) | Indicates significant pulmonary involvement | | Hemoglobin drop | 6.8 (from 7.5) | Acute hemolysis; worsening anemia | | Reticulocyte count | 12% (elevated) | Compensatory response to hemolysis | | LDH | Markedly elevated | Marker of tissue damage and hemolysis | ### Diagnostic Criteria (Modified from NIH) **Clinical Pearl:** ACS diagnosis requires: - Fever OR respiratory symptoms (cough, dyspnea, chest pain) - **NEW** pulmonary infiltrate on imaging (not pre-existing) - In the context of sickle cell disease **Warning:** ACS is a **clinical diagnosis**; do NOT wait for blood cultures or imaging to initiate treatment. Cultures are often negative (sterile infarction), though secondary infection can occur. ### Management Algorithm ```mermaid flowchart TD A[SCD patient + chest pain + dyspnea + fever]:::outcome --> B{New infiltrate on CXR?}:::decision B -->|Yes| C[Acute Chest Syndrome]:::outcome C --> D[Immediate management]:::action D --> E[Oxygen to target SpO₂ >94%]:::action D --> F[Aggressive hydration]:::action D --> F --> G[Analgesia]:::action G --> H[Empiric antibiotics if infection suspected]:::action H --> I[Consider exchange transfusion if severe]:::action B -->|No| J[Consider other diagnoses]:::action ``` ### Key Distinguishing Features **Mnemonic:** **ACS = Acute + Chest + Syndrome + (Sickle Cell) = Anemia + Crisis + Sickling + (Pulmonary) = Acute + Crisis + Systemic** | Feature | ACS | Bacterial Pneumonia | PE | |---------|-----|-------------------|----| | **Fever** | Yes (inflammatory) | Yes (infection) | No (unless infarction) | | **CXR infiltrate** | New, often bilateral lower lobes | Focal consolidation, lobar | Wedge-shaped or normal | | **Blood culture** | Negative (sterile) | Positive (organism isolated) | N/A | | **Hemoglobin trend** | Drops acutely | Stable or mild drop | Stable | | **Reticulocyte count** | Elevated (>8%) | Normal to mildly elevated | Normal | | **LDH** | Markedly elevated | Mildly elevated or normal | Elevated | | **Response to antibiotics** | Partial (supportive care key) | Rapid improvement | No response | **High-Yield:** ACS is the **second leading cause of death** in adults with sickle cell disease (after stroke). Mortality is 5–10% even with treatment. ### Why ACS, Not Bacterial Pneumonia? - **Sterile infarction:** Blood cultures typically negative; fever is from tissue necrosis, not infection. - **Acute hemolysis:** Hemoglobin drop and elevated reticulocytes indicate vaso-occlusive crisis, not infection. - **Elevated LDH:** Marks tissue damage and hemolysis, not typical of uncomplicated pneumonia. - **Clinical context:** In a patient with known SCD presenting with chest pain + dyspnea + new infiltrate, ACS is the default diagnosis until proven otherwise. [cite:Harrison 21e Ch 135] 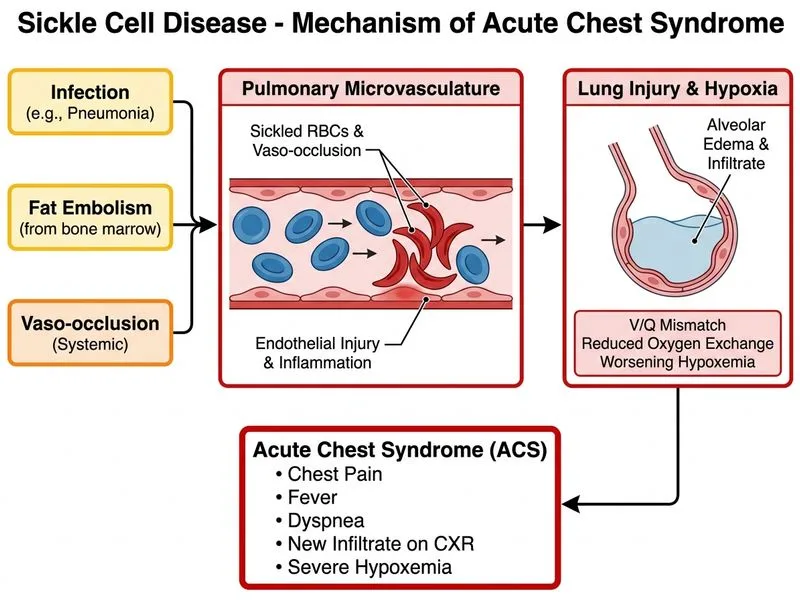
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.