## Mechanism of Functional Ankle Instability **Key Point:** The presence of positive anterior drawer and talar tilt tests with intact ligamentous structures on imaging indicates **functional (or mechanical) ankle instability** rather than structural ligamentous failure. ### Pathophysiology of Recurrent Sprains Despite Intact Ligaments When ligaments are structurally intact but the patient experiences recurrent instability, the underlying mechanism involves: 1. **Proprioceptive dysfunction** — damage to mechanoreceptors in the lateral ankle ligaments and peroneal tendons from previous sprains 2. **Impaired neuromuscular control** — delayed peroneal muscle activation (particularly fibularis longus and brevis) during inversion stress 3. **Postural control deficits** — inability to maintain dynamic ankle stability during sport-specific movements 4. **Sensorimotor integration failure** — loss of rapid reflex stabilization response **High-Yield:** Functional ankle instability is the most common cause of recurrent ankle sprains in athletes, even after the acute ligamentous injury has healed. This explains why imaging may appear normal despite clinical instability. ### Clinical Correlation **Clinical Pearl:** The positive anterior drawer and talar tilt tests indicate ligamentous laxity, but when MRI shows intact ATFL with only synovitis, the recurrence pattern is driven by neuromuscular insufficiency rather than structural failure. This is why proprioceptive training and peroneal strengthening are the cornerstones of prevention and rehabilitation. ### Management Implications **Tip:** Treatment should focus on: - Proprioceptive retraining (single-leg stance, balance board exercises) - Peroneal muscle strengthening (resistance band inversion/eversion) - Sport-specific agility drills - Ankle bracing or taping for return-to-sport Surgical reconstruction is NOT indicated in functional instability without structural ligamentous failure. ```mermaid flowchart TD A[Recurrent ankle sprains]:::outcome --> B{Ligaments intact on MRI?}:::decision B -->|Yes| C[Functional instability]:::outcome B -->|No| D[Structural instability]:::outcome C --> E[Proprioceptive deficit]:::action C --> F[Neuromuscular control impairment]:::action D --> G[Ligamentous repair/reconstruction]:::action E --> H[Proprioceptive training + strengthening]:::action F --> H ``` [cite:Delorme et al. Sports Med 2021; Campbell's Operative Orthopaedics Ch 83] 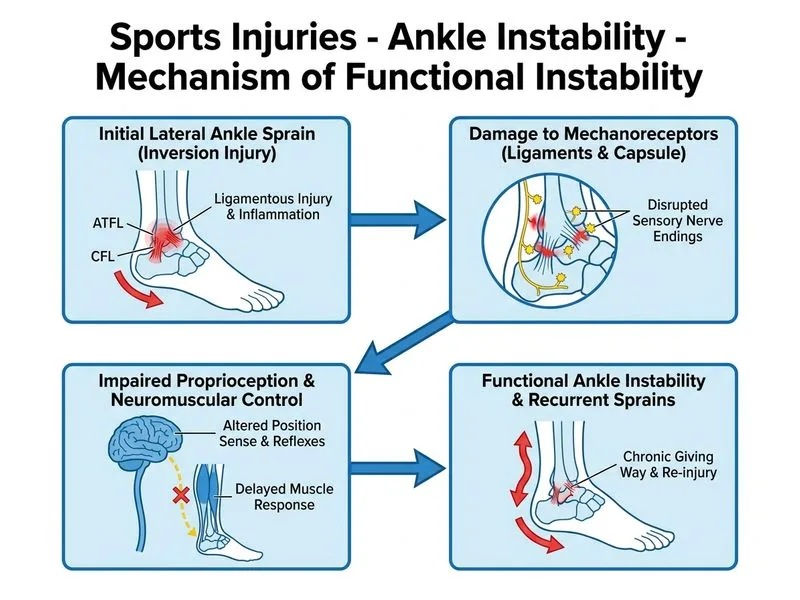
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.