## Management of Refractory Lateral Epicondylitis with Partial Tendon Tear ### Clinical Context This patient has **chronic lateral epicondylitis (tennis elbow) with imaging-confirmed partial ECRB tear** that has failed first-line conservative therapy. The decision now lies between biological augmentation, repeat injections, shock wave therapy, or surgery. ### Why PRP Injection is the Best Next Step **Key Point:** Platelet-rich plasma (PRP) is a Class 2b recommendation (moderate evidence) for refractory lateral epicondylitis and is increasingly preferred as a bridge therapy before surgery because it: - Promotes tendon healing through growth factors (PDGF, TGF-β, VEGF) - Addresses the underlying pathophysiology (degenerative tendinopathy + partial tear) - Avoids the morbidity of open surgery in a patient with only partial tear - Has demonstrated superior outcomes to repeat corticosteroid injections in prospective studies - Allows continued functional rehabilitation alongside biological intervention **Clinical Pearl:** In refractory lateral epicondylitis with partial tendon tears, the evidence hierarchy is: 1. **PRP/biologic augmentation** (first choice for failed conservative care) 2. ESWT (alternative, less evidence than PRP in recent meta-analyses) 3. Surgery (reserved for complete tears, failed PRP, or persistent symptoms >3–6 months post-PRP) ### Why Other Options Are Suboptimal **Immediate surgical debridement and repair (Option 1):** - Premature in a patient with only partial tear - ECRB repair is indicated for complete tears or failed conservative management lasting >6–12 months - Carries risk of stiffness, re-rupture, and prolonged rehabilitation - Should be reserved as a second-line surgical option after PRP failure **Repeat corticosteroid injection (Option 2):** - Multiple corticosteroid injections are associated with increased risk of tendon rupture - Current evidence (2020 meta-analyses) shows diminishing returns after 1–2 injections - Corticosteroids suppress inflammation but do NOT promote healing; they may worsen degenerative changes - Not recommended as sole repeat therapy in refractory cases **ESWT followed by surgery (Option 3):** - ESWT has moderate evidence (Class 2b) but is less favored than PRP in recent guidelines - Sequencing ESWT before surgery is reasonable but adds delay without clear superiority over PRP - PRP has better-quality RCT evidence in partial tears - ESWT is more commonly used in countries with limited access to PRP ### Treatment Algorithm ```mermaid flowchart TD A[Lateral epicondylitis]:::outcome --> B[Conservative: NSAIDs, PT, activity modification]:::action B --> C{Response at 6 weeks?}:::decision C -->|Yes| D[Continue PT, return to sport]:::action C -->|No| E{Imaging: tear present?}:::decision E -->|No tear| F[Corticosteroid injection ± ESWT]:::action E -->|Partial tear| G[PRP injection + supervised PT]:::action E -->|Complete tear| H[Surgical repair]:::urgent G --> I{Improvement at 3 months?}:::decision I -->|Yes| J[Continue PT, gradual return]:::action I -->|No| K[Consider ESWT or surgery]:::action F --> L{Improvement at 3 months?}:::decision L -->|Yes| M[Discharge]:::outcome L -->|No| G ``` **High-Yield:** PRP is increasingly the standard of care for **refractory lateral epicondylitis with imaging evidence of tendon pathology** (partial tear, degeneration). It bridges the gap between failed conservative care and surgery, offering biological healing potential without surgical morbidity. **Mnemonic — ECRB Tear Management:** **PRSS** - **P**RP first (refractory cases with tear) - **R**epeat injection NOT recommended - **S**urgery if PRP fails (3–6 months later) - **S**hock wave as alternative in select cases ### Evidence Summary - **PRP in lateral epicondylitis:** Mishra et al. (2014) showed PRP superior to corticosteroid at 12 weeks in RCT - **Partial ECRB tears:** Respond better to PRP than complete tears - **Timing:** PRP injection followed by 4–6 weeks of supervised physiotherapy is standard **Tip:** In exam scenarios, always ask: "Has conservative care failed?" → "Is there imaging evidence of tear?" → "If yes, PRP is the bridge to surgery." 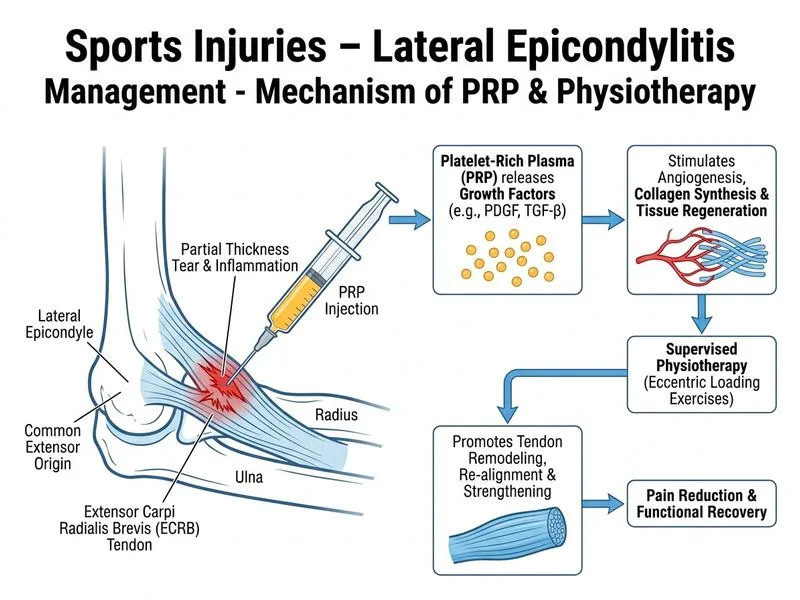
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.