## Squamous Cell Carcinoma (SCC) — High-Risk Features & Prognostic Factors ### Clinical Presentation & Diagnosis The patient presents with a classic high-risk cutaneous SCC on the temple with: - Indurated plaque with ill-defined borders - Central erosion/ulceration - Surrounding erythema - Infiltrative histological pattern - **Perineural invasion (PNI)** — a hallmark aggressive feature ### Key Prognostic Factors in Cutaneous SCC | Factor | Risk Category | Significance | |--------|---------------|---------------| | **Perineural invasion** | High-risk | Strong predictor of local recurrence, regional spread, and worse OS | | **Depth >4 mm (Clark level IV–V)** | High-risk | Correlates with increased metastatic potential | | **Poorly differentiated grade** | High-risk | Associated with aggressive behavior | | **Location (ear, lip, temple)** | High-risk | Higher recurrence and metastasis rates | | **Size >2 cm** | Intermediate-risk | Modest increase in recurrence | | **Immunosuppression** | High-risk | Dramatically increases aggressive phenotype | ### Why Perineural Invasion Mandates Adjuvant Therapy **Key Point:** Perineural invasion (PNI) is the single most important adverse prognostic factor in cutaneous SCC, indicating: 1. Tumor cells tracking along nerve sheaths → higher local recurrence 2. Potential for skip lesions and occult disease beyond clinical margins 3. Increased risk of regional lymph node metastasis (up to 47% in some series) 4. Worse overall survival compared to non-PNI tumors **Clinical Pearl:** When PNI is present, especially in combination with depth >4 mm, adjuvant radiotherapy is strongly recommended to reduce local recurrence and improve disease-free survival [cite:NCCN Cutaneous SCC Guidelines 2023]. ### Treatment Algorithm ```mermaid flowchart TD A[Cutaneous SCC diagnosed]:::outcome --> B{Risk stratification}:::decision B -->|Low-risk: <2cm, well-diff, no PNI| C[Mohs or wide excision]:::action B -->|High-risk: PNI, depth >4mm, poor diff| D{Margins clear?}:::decision D -->|Yes| E[Consider adjuvant RT]:::action D -->|No| F[Re-excision or Mohs]:::action E --> G[Improved local control & DFS]:::outcome F --> H{Margins clear now?}:::decision H -->|Yes| I[Adjuvant RT strongly recommended]:::action H -->|No| J[Consider chemotherapy + RT]:::urgent ``` ### Why Other Options Are Incorrect **Option 1 (Correct):** Perineural invasion + depth >4 mm = highest-risk phenotype requiring adjuvant radiotherapy. **Option 2 (Fitzpatrick type + facial location):** While facial location is a risk factor, Fitzpatrick skin type alone is NOT a primary determinant of adjuvant therapy decisions in SCC. The presence of PNI overrides skin type considerations. **Option 3 (Age + gender):** Age and male gender are epidemiological risk factors for SCC development but do NOT independently dictate adjuvant therapy. PNI status is far more prognostically relevant. **Option 4 (Size + ulceration):** Size >1 cm and ulceration are intermediate-risk features, but neither is as powerful a predictor of aggressive behavior as PNI. A 1.5 cm SCC without PNI has a much better prognosis than a smaller tumor with PNI. **High-Yield:** PNI is present in 2–5% of cutaneous SCCs but is found in up to 50% of high-grade or recurrent tumors. Its presence alone justifies consideration of adjuvant radiotherapy regardless of other factors [cite:Robbins & Cotran Pathologic Basis of Disease 10e Ch 25]. ### Clinical Management Summary - **Mohs micrographic surgery** is preferred for high-risk SCC (allows margin assessment) - **Adjuvant radiotherapy** is indicated when: - Perineural invasion is present - Depth >4 mm - Positive or close margins despite re-excision - Poorly differentiated histology - High-risk anatomical sites (ear, lip, temple) - **Follow-up:** Regional lymph node examination every 3–6 months for 2 years 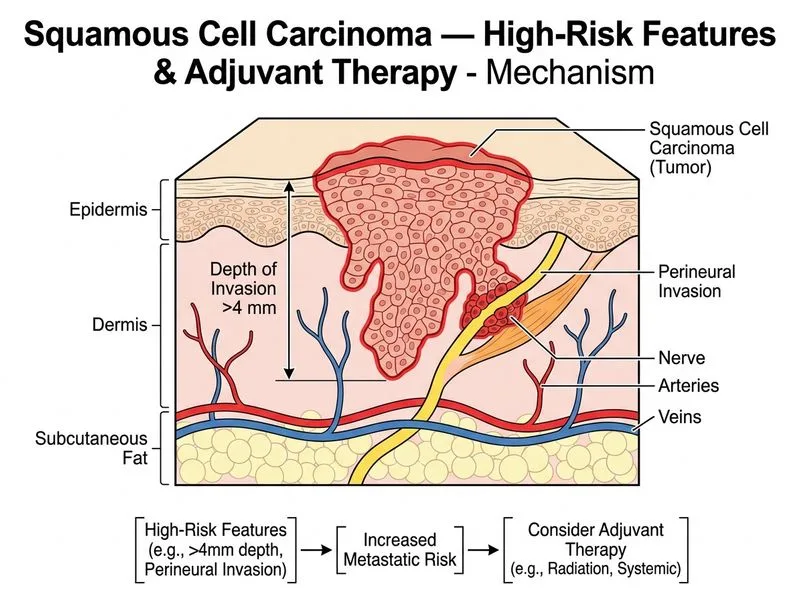
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.