## Diagnosis Confirmation in Suspected Cutaneous SCC **Key Point:** Histopathological examination via tissue biopsy is the gold standard for diagnosing squamous cell carcinoma and determining grade, depth of invasion, and perineural involvement — all critical for staging and treatment planning. ### Why Incisional Biopsy is the Investigation of Choice 1. **Diagnostic certainty**: Histology demonstrates malignant keratinocytes, degree of differentiation (well/moderately/poorly differentiated), and architectural patterns. 2. **Prognostic assessment**: Depth of invasion (Clark level, Breslow thickness equivalent) guides surgical margins and need for sentinel lymph node biopsy. 3. **Perineural invasion detection**: Present in ~5–10% of cutaneous SCC; presence upgrades risk and influences adjuvant therapy. 4. **Margin assessment**: Incisional biopsy from the lesion edge and center ensures representative sampling. **High-Yield:** In a fixed, indurated lesion with ulceration and 8-month duration, clinical suspicion for SCC is high. Biopsy is non-negotiable before any definitive treatment. ### Biopsy Technique Considerations | Biopsy Type | Indication | Limitation | |---|---|---| | **Incisional** | Large/deep lesions, assess depth & margins | Requires suturing | | **Excisional** | Small lesions (<1 cm), therapeutic intent | May not assess depth adequately if lesion extends beyond specimen | | **Punch** | Superficial lesions only | Inadequate for depth assessment in suspected invasive SCC | **Clinical Pearl:** In a farmer with chronic sun exposure and a non-healing ulcer, SCC is the leading diagnosis. The fixed, indurated nature and central ulceration suggest invasion beyond the dermis, making depth assessment via biopsy essential for Mohs micrographic surgery vs. wide excision vs. adjuvant radiation planning. 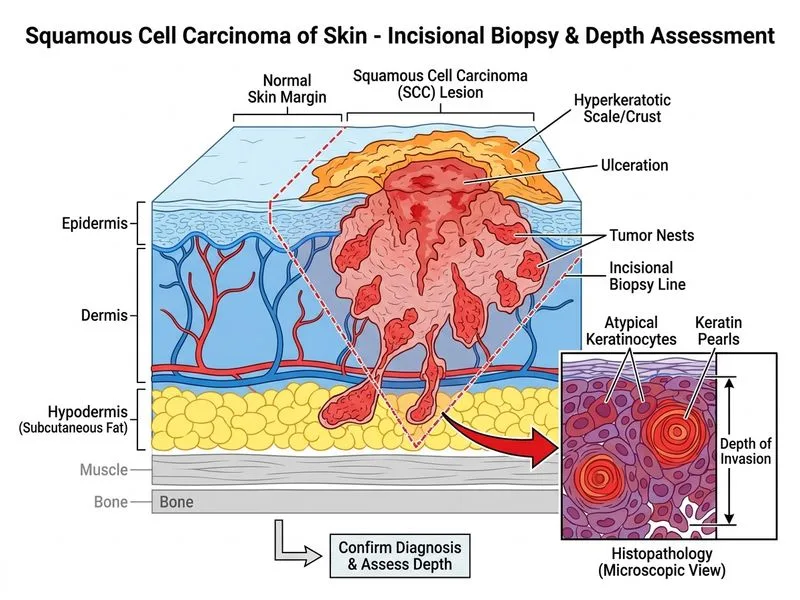
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.