## Risk Stratification in Cutaneous SCC: Perineural Invasion ### Clinical Context This 62-year-old farmer has a high-risk SCC on the hand (non-face site, >2 cm, depth 8 mm). The question asks for the BEST discriminator between high-risk and low-risk variants. **Key Point:** Perineural invasion (PNI) is the SINGLE MOST IMPORTANT prognostic factor that distinguishes aggressive, high-risk SCC from indolent low-risk disease, independent of size, grade, or depth. ### High-Risk vs Low-Risk SCC: Comparison Table | Feature | Low-Risk SCC | High-Risk SCC | | --- | --- | --- | | **Perineural invasion** | Absent | Present (BEST DISCRIMINATOR) | | **Depth** | <4 mm | >4 mm | | **Differentiation** | Well to moderate | Moderate to poor | | **Location** | Face, ear, scalp (paradoxically lower risk) | Non-face (hand, trunk, leg) | | **Size** | <2 cm | >2 cm | | **Ulceration** | Absent | Present | | **5-year recurrence** | <5% | 30–50% | | **Metastatic risk** | <1% | 5–15% | **High-Yield:** PNI is present in only 2–5% of low-risk SCC but in 25–50% of high-risk SCC. Its presence ALONE upgrades prognosis and mandates aggressive treatment (Mohs surgery or wide excision + sentinel lymph node biopsy consideration). ### Why PNI Is the Best Discriminator 1. **Strongest independent prognostic factor:** Presence of PNI increases local recurrence 5-fold and metastatic risk 3-fold, regardless of other factors. 2. **Changes management:** PNI-positive SCC requires: - Wider margins (6–10 mm vs 4–6 mm) - Consideration of adjuvant radiotherapy - Sentinel lymph node biopsy if other high-risk features present 3. **Specific to aggressive phenotype:** PNI indicates tumor cells tracking along nerve sheaths — a sign of biological aggressiveness not captured by grade or depth alone. ### Refutation of Other Options **Depth >4 mm (Option A):** While depth is important for staging (T2 vs T3 in AJCC), it is NOT more discriminatory than PNI. A 5 mm SCC without PNI may behave indolently; a 3 mm SCC WITH PNI is high-risk. **Well-differentiated histology (Option C):** This is INVERSELY related to risk — well-differentiated SCC is LOW-risk. This option is a trap. **Absence of ulceration (Option D):** Ulceration is a clinical sign but is less prognostically powerful than PNI. A non-ulcerated SCC with PNI is still high-risk. ### Mnemonic: HIGH-RISK SCC Features **"DEPTH-PNI"** - **D**epth >4 mm - **E**ar, lip, non-face location - **P**erineural invasion ← STRONGEST - **T**hickness >4 mm - **H**istologic grade III–IV - **P**oor differentiation - **N**on-face, high-risk site - **I**mmunosuppression **Clinical Pearl:** In this patient (farmer, hand location, 8 mm depth, ulcerated), if PNI is present on biopsy, the 5-year recurrence risk jumps from ~10% to 40–50%. This mandates Mohs micrographic surgery or wide excision with intraoperative margin assessment, not simple excision. [cite:Robbins 10e Ch 25; AJCC Cancer Staging Manual 8e] 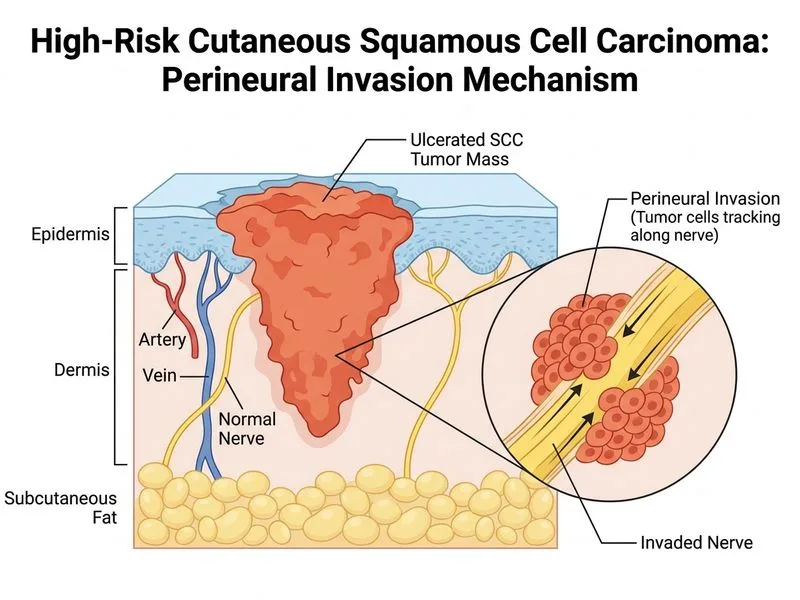
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.