## Prognostic Factors in Cutaneous SCC **Key Point:** Not all prognostic factors are equally important. Anatomical location and histological features like perineural invasion are the strongest predictors of recurrence and metastasis in cutaneous SCC. ## High-Risk Features in SCC | Feature | Prognostic Impact | Clinical Significance | |---------|------------------|----------------------| | **Lip location (vermillion)** | **Very high** | Increased perineural invasion, higher recurrence (5–20%), higher metastatic risk (5–15%) | | **Perineural invasion** | **Very high** | Indicates aggressive biology, requires wider margins, higher recurrence | | **Depth > 4 mm (Clark level IV–V)** | **High** | Associated with increased metastatic risk | | **Poor/undifferentiated** | **High** | Worse prognosis than well/moderate differentiation | | **Size > 2 cm** | **Moderate** | Increased risk, but less predictive than location/PNI | | **Ki-67 expression** | **Low–Moderate** | Proliferation marker, but not independent prognostic factor in cutaneous SCC | | **Age** | **Low** | Age alone is not a strong prognostic factor | **High-Yield:** Lip SCC (especially vermillion border) is a **distinct entity** with significantly worse prognosis than trunk/extremity SCC: - Higher propensity for perineural invasion - Higher local recurrence rate (10–20% vs. 2–5% for non-lip SCC) - Higher metastatic rate (5–15% vs. 0.5–5% for non-lip SCC) - Requires more aggressive treatment (wider margins, possible neck dissection if nodal involvement) ## Why Location on the Lip Is the Most Important Prognostic Factor ```mermaid flowchart TD A[SCC of lip vermillion]:::outcome --> B{Anatomical factors}:::decision B -->|Rich vascular supply| C[Higher metastatic potential]:::urgent B -->|Thin mucosa| D[Deeper invasion risk]:::urgent B -->|Perineural invasion common| E[Higher recurrence]:::urgent C --> F[Aggressive treatment needed]:::action D --> F E --> F F --> G[Wide excision + neck assessment]:::action ``` **Clinical Pearl:** Lip SCC should be treated more aggressively than SCC of other skin sites. Standard margins are 5–10 mm, but lip lesions often require 10 mm or more. Sentinel lymph node biopsy or neck dissection should be considered even for T1 lesions if perineural invasion is present. ## Why Each Distractor Is Incorrect ### Option 0: High Ki-67 Expression **Warning:** Ki-67 is a proliferation marker and may correlate with cell cycle activity, but it is **not an independent prognostic factor** in cutaneous SCC. While high Ki-67 may suggest aggressive behavior, it does not override anatomical and histological factors (location, differentiation, perineural invasion) that are far more predictive of outcome. ### Option 2: Moderate Differentiation Differentiation grade (well vs. moderate vs. poor) is important, but **location and perineural invasion are more powerful predictors**. A well-differentiated SCC on the lip with perineural invasion has worse prognosis than a moderately differentiated SCC on the trunk without perineural invasion. ### Option 3: Age and Sun Exposure Age is a weak prognostic factor in cutaneous SCC. Cumulative sun exposure is a risk factor for development, but once the tumor is present, age does not significantly influence recurrence or metastasis rates. Tumor biology (location, histology, invasion) matters far more than patient age. [cite:Robbins 10e Ch 25; AJCC Cancer Staging Manual 8th Edition] 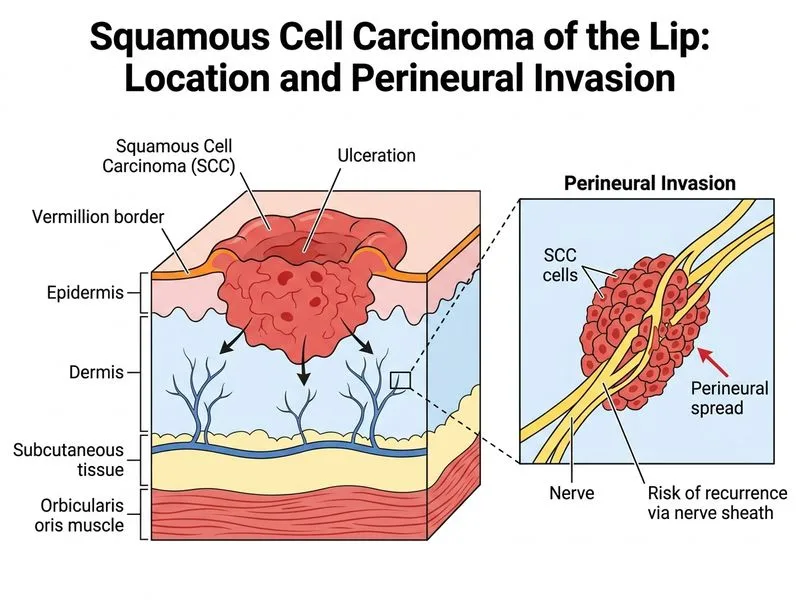
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.