## Management of High-Risk Cutaneous SCC ### Risk Stratification in This Case **Key Point:** This patient has multiple high-risk features: 1. **Location:** Ear (H-zone) — high-risk anatomical site with increased recurrence and metastasis risk 2. **Depth:** Reticular dermal invasion (Clark IV) — 5–10% metastasis risk 3. **Grade:** Moderately differentiated — intermediate biological aggressiveness 4. **Regional lymphadenopathy:** Suggests nodal involvement (clinical Stage IIIB–IV) ### High-Risk SCC Definition | Feature | Risk Category | |---|---| | Clark IV–V invasion | High-risk | | Poorly differentiated histology | High-risk | | Diameter >2 cm | High-risk | | Location: ear, lip, eyelid, nose | High-risk | | Immunosuppression (transplant, HIV, CLL) | High-risk | | Perineural invasion | Very high-risk | | Regional lymphadenopathy | Advanced disease | ### Recommended Management Algorithm ```mermaid flowchart TD A[High-risk SCC: Clark IV, ear location, regional LN]:::outcome --> B{Surgical approach?}:::decision B -->|Mohs preferred| C[Mohs micrographic surgery]:::action B -->|Mohs unavailable| D[Wide local excision 10-15mm]:::action C --> E{Regional LN involvement?}:::decision D --> E E -->|Yes/Clinically suspicious| F[Sentinel lymph node biopsy]:::action E -->|No| G[Clinical observation q3-6 months]:::action F --> H{Positive nodes?}:::decision H -->|Yes| I[Neck dissection + adjuvant RT]:::action H -->|No| G ``` ### Why Mohs Micrographic Surgery? **High-Yield:** Mohs surgery is the gold standard for high-risk SCC because: - **Margin control:** Real-time histological assessment of 100% of margins (vs. 5–10% in standard excision) - **Tissue preservation:** Removes only tumor-bearing tissue, sparing maximum normal skin - **Recurrence rates:** 1–3% for high-risk SCC vs. 5–15% with standard excision - **Particularly indicated:** Ear, lip, periocular, perineural invasion, recurrent lesions ### Sentinel Lymph Node Biopsy Indications **Clinical Pearl:** SLNB is indicated when: - Clark IV–V invasion with high-grade histology - Clinically suspicious regional lymphadenopathy (as in this case) - Diameter >2 cm with high-risk features - Perineural invasion - Immunosuppressed patients In this patient, the palpable cervical lymph node makes SLNB mandatory to: 1. Confirm nodal involvement 2. Stage the disease accurately (AJCC Stage IIIB vs. IV) 3. Guide adjuvant therapy (radiation ± chemotherapy if nodes are positive) ### Adjuvant Therapy Considerations - **Radiation therapy:** Reserved for: - Positive lymph nodes after SLNB/neck dissection - Perineural invasion - Close/positive margins that cannot be re-excised - Recurrent disease - NOT as primary treatment for resectable disease - **Chemotherapy:** Indicated only for: - Unresectable disease - Distant metastases - Palliative care - NOT for localized high-risk SCC without systemic disease 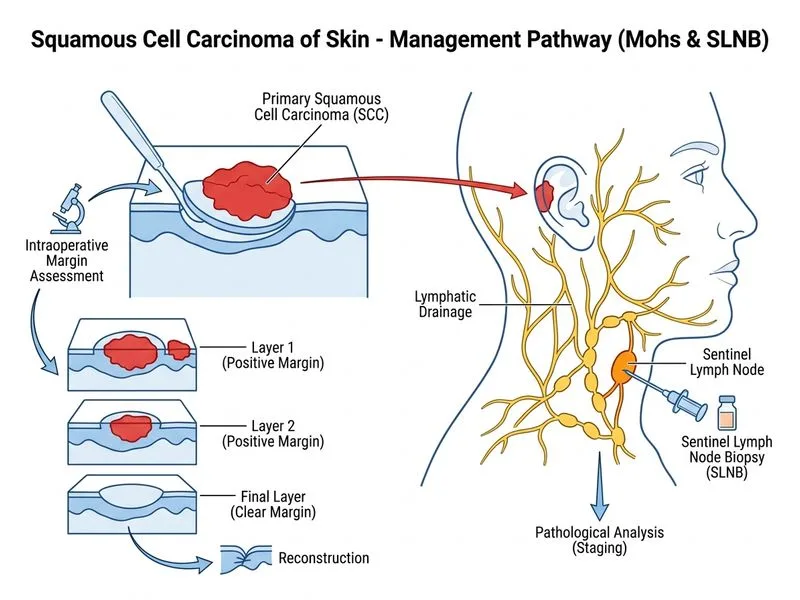
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.