## Clinical Assessment This patient has a **low-risk squamous cell carcinoma** of the skin. Key features supporting low-risk classification: - Well-differentiated histology - No perineural invasion - No regional lymph node involvement - Size < 4 cm - Non-facial location (dorsum of hand is relatively low-risk) ## Management Strategy for Low-Risk SCC **Key Point:** Low-risk SCC of the skin is managed by **wide local excision (WLE) with adequate margins**, followed by clinical surveillance. Sentinel lymph node biopsy (SLNB) and adjuvant chemotherapy are NOT indicated for low-risk disease. ### Recommended Surgical Margins by Risk Category | Risk Category | Recommended Margin | Rationale | |---|---|---| | **Low-risk SCC** | 4–5 mm | Adequate for well-differentiated, small, non-facial lesions without high-risk features | | **Intermediate-risk SCC** | 6–10 mm | Larger margin for moderately differentiated or larger lesions | | **High-risk SCC** | 10–15 mm or Mohs | For poorly differentiated, large (>4 cm), perineural invasion, immunocompromised, or facial lesions | ## Why WLE with Clinical Surveillance is Correct 1. **Histology is favorable:** Well-differentiated SCC with no perineural invasion has a low risk of lymph node metastasis (~5% or less). 2. **No nodal involvement clinically:** Physical examination shows no palpable regional lymph nodes; SLNB is unnecessary. 3. **Standard of care:** For low-risk SCC, WLE with 4–5 mm margins followed by clinical surveillance is the evidence-based approach [cite:Dermatology Textbook - SCC Management]. 4. **Cost-effective:** Avoids unnecessary sentinel node procedures and systemic therapy. ## Why Each Distractor Is Wrong **High-Yield:** SLNB is reserved for **high-risk SCC** (poorly differentiated, >4 cm, perineural invasion, immunocompromised patients, or those with clinical nodal involvement). This patient does not meet criteria. **Clinical Pearl:** Mohs micrographic surgery is the gold standard for **high-risk SCC** (especially facial lesions, recurrent tumors, or those with perineural invasion). It is not indicated for low-risk lesions on the hand. **Warning:** Do not confuse SCC management with melanoma — melanoma routinely requires SLNB even for intermediate-thickness lesions. SCC has a much lower propensity for occult nodal metastasis and does not follow the same staging algorithm. ## Surveillance Protocol Post-WLE - **Clinical examination** of the excision site and regional lymph nodes every 3–6 months for the first 2 years - **Patient education** on sun protection and self-examination - **Imaging** (ultrasound or CT) only if lymph nodes become palpable or symptomatic ```mermaid flowchart TD A[SCC of Skin Diagnosed]:::outcome --> B{Risk Stratification}:::decision B -->|Low-risk: Well-diff, <4cm, no PNI, no nodal involvement| C[Wide Local Excision 4-5mm margins]:::action B -->|High-risk: Poorly-diff, >4cm, PNI, facial, immunocompromised| D[Mohs or WLE 10-15mm + SLNB]:::action C --> E[Clinical Surveillance q3-6 months]:::action D --> F[Adjuvant therapy if nodal involvement]:::action E --> G[Recurrence-free survival]:::outcome ``` 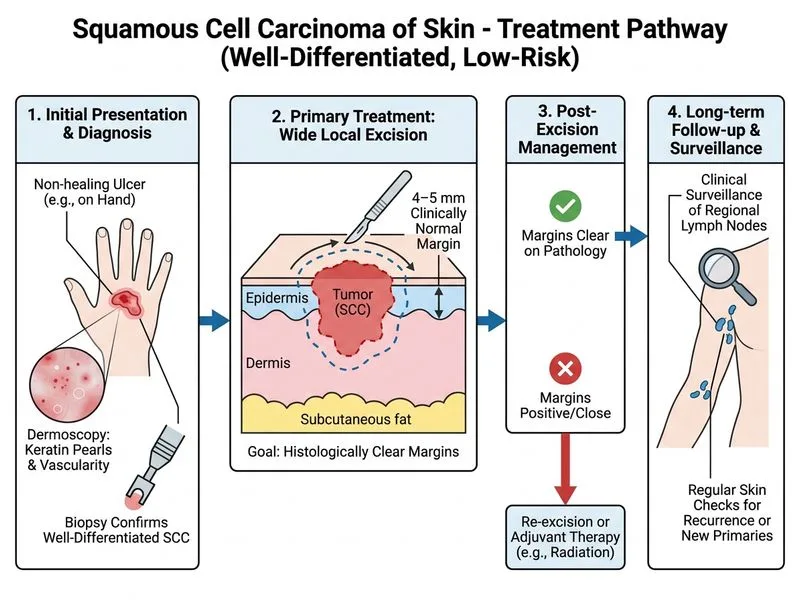
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.