## Risk Stratification of This SCC This patient has a **high-risk squamous cell carcinoma** with multiple adverse prognostic factors: | Risk Feature | Present? | Significance | |---|---|---| | **Histologic grade** | Poorly differentiated | High-risk | | **Perineural invasion (PNI)** | Yes | Major adverse feature; increases local recurrence and metastasis risk | | **Location** | Ear (high-risk site) | Ear, lip, and perioral areas have higher recurrence rates | | **Size** | 2.5 cm | Intermediate-to-large | | **Nodal involvement** | Clinically negative | But high-risk for occult metastasis | **High-Yield:** Perineural invasion is a **critical prognostic factor** that mandates aggressive management and staging. ## Why Mohs + SLNB Is Correct ### Mohs Micrographic Surgery 1. **Highest cure rate (95–99%)** for high-risk SCC, especially with perineural invasion 2. **Intraoperative margin assessment** allows real-time visualization of tumor extent and complete margin clearance 3. **Tissue-sparing:** Removes only tumor and minimal normal tissue, important for the ear where function and cosmesis matter 4. **Indicated for:** Poorly differentiated SCC, perineural invasion, facial/ear location, recurrent tumors, immunocompromised patients ### Sentinel Lymph Node Biopsy 1. **Indicated in high-risk SCC** to stage the regional lymph nodes 2. **Perineural invasion** significantly increases the risk of occult regional metastasis (10–20%) 3. **Guides adjuvant therapy:** If SLNB is positive, adjuvant radiotherapy ± chemotherapy is recommended 4. **Prognostic value:** Positive nodes indicate need for close surveillance or completion lymph node dissection **Clinical Pearl:** Unlike melanoma, SLNB in SCC is **not routine** for all tumors—it is reserved for high-risk disease. This patient qualifies due to perineural invasion and poorly differentiated histology. ## Management Algorithm for High-Risk SCC ```mermaid flowchart TD A[SCC with High-Risk Features]:::outcome --> B[Mohs Micrographic Surgery]:::action B --> C[Complete Margin Clearance]:::outcome C --> D{SLNB Performed?}:::decision D -->|Negative| E[Observation + Surveillance]:::action D -->|Positive| F[Adjuvant Radiotherapy ± Chemotherapy]:::action E --> G[Clinical follow-up q3 months]:::action F --> G G --> H[Recurrence-free survival]:::outcome ``` ## Why Each Distractor Is Wrong **Warning:** Standard WLE (even with 10–15 mm margins) is **inferior to Mohs** for high-risk SCC because it lacks intraoperative margin assessment and has higher recurrence rates (10–15% vs. 1–5% with Mohs). **Key Point:** Neoadjuvant chemotherapy is **not standard** for resectable SCC. It is reserved for unresectable, metastatic, or palliative settings. This patient has a resectable tumor and should undergo surgery first. ## Adjuvant Radiotherapy Indications Adjuvant radiotherapy is considered for: - Positive surgical margins (if re-excision not possible) - Positive regional lymph nodes (SLNB or CLND) - Perineural invasion with nodal involvement - Recurrent tumors - Immunocompromised patients with high-risk features In this case, radiotherapy decisions should be made **after** Mohs excision and SLNB results. 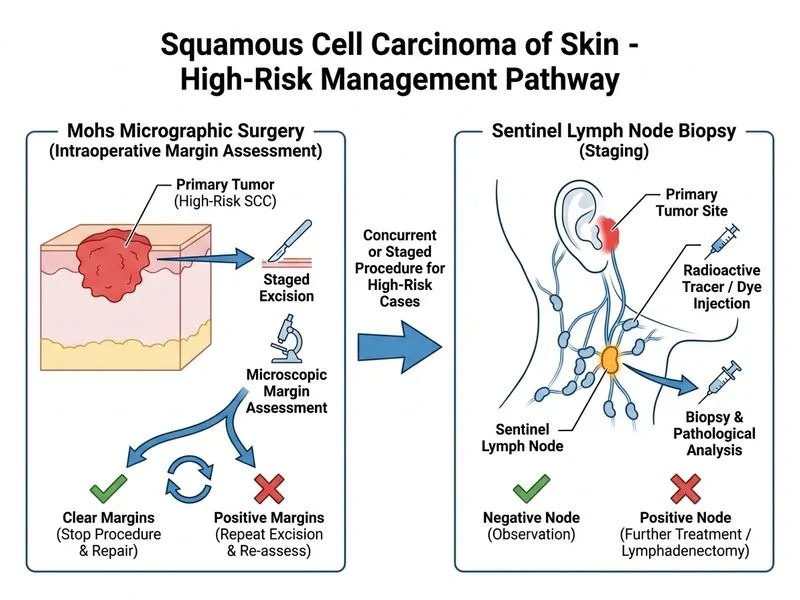
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.