## Clinical Presentation: Anterior STEMI with Cardiogenic Shock **Key Point:** This patient has acute anterior wall STEMI complicated by cardiogenic shock (hypotension, tachycardia, pulmonary oedema, reduced ejection fraction). This is a high-risk presentation requiring urgent revascularization. ## Diagnostic Features | Finding | Significance | |---------|-------------| | ST elevation V1–V4 | Anterior wall STEMI (LAD territory) | | Hypotension (88/56) + tachycardia | Cardiogenic shock | | Bilateral crackles | Pulmonary oedema (LV failure) | | EF 28% | Severe systolic dysfunction | | Elevated troponin | Myocardial necrosis confirmed | ## Why Primary PCI is Mandatory **High-Yield:** In STEMI with cardiogenic shock, primary PCI is the gold standard reperfusion strategy. Thrombolysis has been shown to be inferior in this subset (SHOCK trial). **Mnemonic: SHOCK Trial Lesson — **S**urgical/percutaneous revascularization, **H**igh-risk STEMI, **O**utcome improved, **C**ardiogenic shock, **K**ey: PCI > thrombolysis** ## Management Algorithm ```mermaid flowchart TD A[Anterior STEMI + Cardiogenic Shock]:::outcome --> B{PCI-capable centre available?}:::decision B -->|Yes, <120 min| C[Immediate Primary PCI]:::action B -->|No| D[Consider thrombolysis + transfer]:::action C --> E{Haemodynamic support needed?}:::decision E -->|Yes| F[IABP or mechanical support]:::action E -->|No| G[Standard PCI + dual antiplatelet]:::action F --> G G --> H[Intensive post-PCI monitoring]:::action D --> I[Thrombolysis door-to-needle <30 min]:::action ``` ## Mechanical Support Considerations **Clinical Pearl:** In cardiogenic shock from acute MI, intra-aortic balloon pump (IABP) can: - Reduce afterload (improves cardiac output) - Augment diastolic pressure (improves coronary perfusion) - Bridge to PCI or definitive therapy **Warning:** Do NOT use vasodilators (nitrates) as monotherapy in cardiogenic shock — they worsen hypotension. Nitrates are adjunctive only after haemodynamic stabilization. ## Why NOT Thrombolysis? 1. **SHOCK Trial (1999):** Showed PCI superior to thrombolysis in cardiogenic shock (30-day mortality: 46.7% thrombolysis vs. 38.6% PCI) 2. **Anterior STEMI:** Higher risk of mechanical complications (rupture, VSD); needs angiographic assessment 3. **Haemodynamic instability:** Thrombolysis may worsen shock; PCI allows direct assessment and mechanical support ## Inotropes: Adjunctive Only **Key Point:** Dobutamine or milrinone are temporizing measures, not definitive therapy. They increase myocardial oxygen demand and may worsen ischaemia if coronary flow is not restored. Revascularization must be the priority. 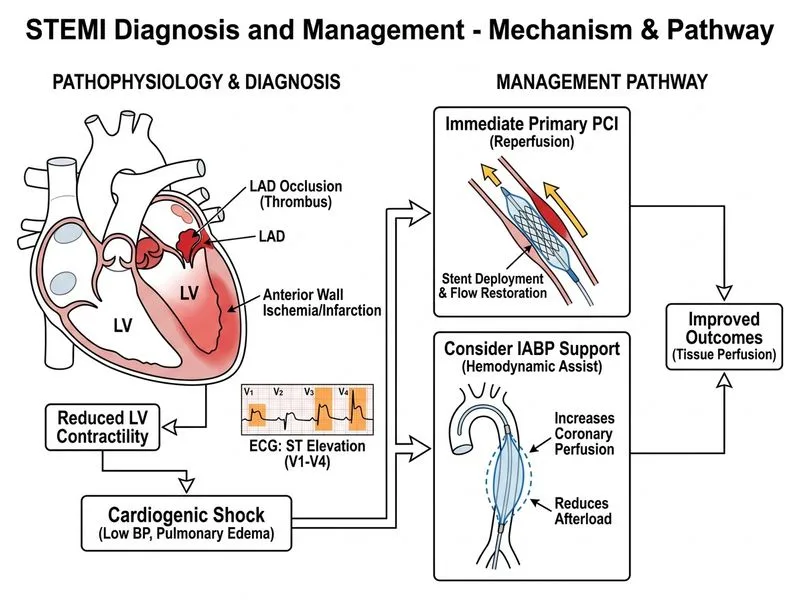
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.