## Clinical Scenario Analysis This is an **anterior wall STEMI** (ST elevation V1–V4, reciprocal changes in inferior leads) in a **PCI-capable hospital** presenting **6 hours after symptom onset** with established myocardial necrosis (elevated troponin). ## Key Decision Points **High-Yield:** The presence of: 1. **STEMI on ECG** (diagnostic, not requiring troponin confirmation) 2. **PCI facility available** (in-house catheterization lab) 3. **Symptom onset within 12 hours** (still within therapeutic window) 4. **Haemodynamic stability** (no cardiogenic shock) All point to **immediate primary PCI** as the standard of care. ## Time Window for Reperfusion **Key Point:** Although the patient is 6 hours from symptom onset, **primary PCI remains the gold standard** because: - Door-to-balloon time can be achieved within 90 minutes (patient is already in a PCI-capable hospital). - PCI is superior to thrombolysis even in the 6–12 hour window if haemodynamically stable. - Anterior STEMI (LAD territory) carries high mortality; reperfusion is critical. **Clinical Pearl:** The 12-hour window is a guideline threshold. PCI is indicated up to 12 hours in stable patients; beyond 12 hours, PCI is reserved for haemodynamic instability or mechanical complications. ## Why Not Thrombolysis? Thrombolysis is **not indicated** in this scenario because: 1. **Primary PCI is available and superior** — thrombolysis is only used when PCI is unavailable or cannot be performed within 120 minutes. 2. **Anterior STEMI has higher mortality** — PCI provides better outcomes than thrombolysis in this territory. 3. **Patient is haemodynamically stable** — no indication for "rescue" thrombolysis followed by PCI. **Warning:** Administering thrombolysis when primary PCI is available is a **common exam trap**. Thrombolysis is second-line, not first-line, in PCI-capable centres. ## Why Not Delayed Angiography? **High-Yield:** The option to "perform angiography after 48 hours" is **incorrect** because: - STEMI is a **time-critical emergency**. Reperfusion must occur within hours, not days. - Delaying angiography results in **irreversible myocardial necrosis** and poor left ventricular function. - Troponin elevation does not change the urgency — it confirms necrosis has already begun; reperfusion must be expedited, not delayed. **Mnemonic:** **STEMI = Time is Myocardium** — every minute of ischaemia results in irreversible damage. ## Management Algorithm ```mermaid flowchart TD A[Anterior STEMI on ECG]:::outcome --> B{PCI-capable hospital?}:::decision B -->|Yes| C{Time from symptom<br/>onset < 12 hours?}:::decision B -->|No| D[Transfer for PCI<br/>or thrombolysis]:::action C -->|Yes| E[Primary PCI<br/>door-to-balloon < 90 min]:::action C -->|No| F{Haemodynamically<br/>stable?}:::decision F -->|Yes| G[PCI still indicated<br/>for mechanical complications]:::action F -->|No| H[PCI for cardiogenic shock]:::urgent E --> I[Reperfusion achieved]:::outcome G --> I H --> I ``` ## Adjunctive Medications **Key Point:** The patient has already received **DAPT (aspirin + clopidogrel)**, which is correct. Additional management includes: - **Unfractionated heparin** (bolus 60–70 U/kg IV) or **enoxaparin** during PCI. - **Glycoprotein IIb/IIIa inhibitor** (e.g., abciximab, tirofiban) — considered in high-risk STEMI (anterior wall, large infarct). - **High-intensity statin** (e.g., atorvastatin 80 mg daily) — initiated immediately, not deferred. - **Beta-blocker** — if no contraindications (haemodynamically stable). These are **adjuncts to PCI**, not alternatives. 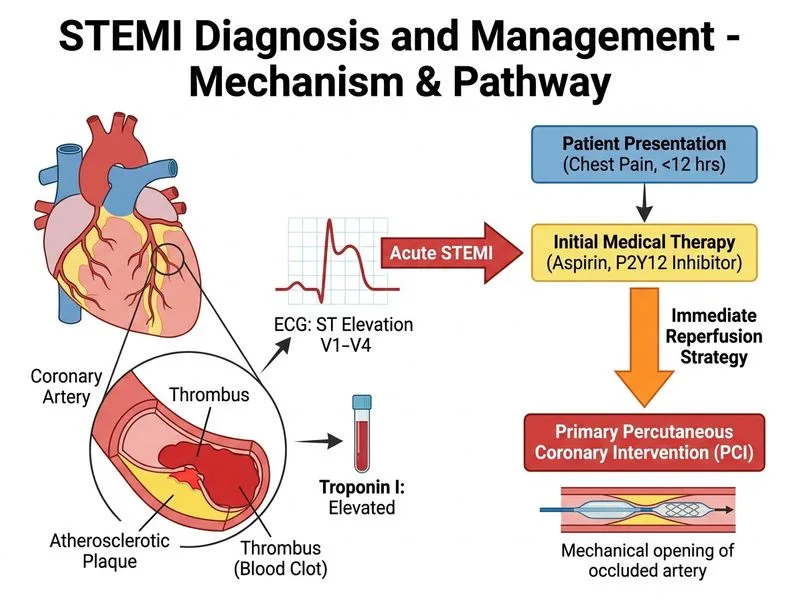
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.